This course aims to ensure that nurses of all licensure levels understand the components and the delivery process of palliative care (PC) with specific strategies and interventions to utilize as a means to control distressing symptoms of serious illness, enhance comfort, and improve quality of life for the duration of the illness.
Course preview
Palliative Care
Disclosure Statement
This course aims to ensure that nurses of all licensure levels understand the components and the delivery process of palliative care (PC) with specific strategies and interventions to utilize as a means to control distressing symptoms of serious illness, enhance comfort, and improve quality of life for the duration of the illness.
Upon completion of this activity, learners should be able to:
- define the distinguishing features of palliative care, compare and contrast with hospice care and end-of-life (EOL) care, and describe models of PC delivery
- discuss the eight domains of PC and the advanced practice registered nurse’s (APRN) or nurses’ role in care delivery as aligned with clinical practice guidelines
- identify the role of advance care planning as a core component of PC and demonstrate an understanding of the essential documents and features comprising advance care planning
Definitions
The definition of PC has evolved over the last several decades. The World Health Organization (WHO, 2023) defines PC as an approach that improves the quality of life of all patients and their families facing problems associated with life-threatening illness. It prevents and relieves suffering through the early identification, correct assessment, and treatment of pain and other symptoms, whether physical, social, psychological, or spiritual. The National Coalition for Hospice and Palliative Care (NCHPC, 2018) defines PC as follows: beneficial at any stage of a serious illness, PC is an interdisciplinary care delivery system designed to anticipate, prevent, and manage physical, psychological, social, and spiritual suffering to optimize quality of life for patients, their families, and caregivers. PC can be delivered in any care setting through the collaboration of many types of care providers. Through early integration into the care plan of seriously ill patients, PC improves quality of life for both the patient and the family.
Palliative Care
While the term PC is widely utilized throughout health care settings, it is often misunderstood. Many people confuse PC with EOL or hospice care. The need for PC is heightened at the EOL due to increased symptom burden; however, it is appropriate at any point during a chronic illness. Unlike hospice care, PC can be provided simultaneously with curative treatment. It is based on the patient’s need, not prognosis. The primary goal is to focus on improving the quality of life and quality of care for patients with life-threatening or life-limiting illness and their families by reducing suffering, alleviating pain, and managing any other distressing symptoms such as depression, dyspnea, fatigue, nausea and vomiting, diarrhea or constipation, incontinence, inability to perform activities of daily living, insomnia, anxiety, restlessness, and loss of appetite. Pain management is a core PC component but also exists as a stand-alone medical subspecialty. Pain is subjective and is often complicated by the uniqueness of the individual’s experience. The etiology of pain is usually complex and multifaceted, thereby heightening the importance of proper clinical assessment, diagnosis, and identification of underlying and contributing conditions to reduce pain to an acceptable level. With the rise of the opioid epidemic that continues to plague the United States, all healthcare providers (HCPs) must ascertain an accurate and comprehensive understanding regarding best practices for pain management to preserve the integrity of clinical practice, safeguard patient care, and reduce the risk for opioid use disorders (Bischoff et al., 2026; Center to Advance Palliative Care [CAPC], n.d.).
PC aids in encouraging, promoting, and facilitating communication about goals of care and advance care planning (ACP). While PC is always a component of hospice care, it should not be reserved only for EOL. PC is appropriate at any stage in a severe illness and ideally should be employed throughout the active treatment of the disease. It does not intend to hasten or postpone death but offers a support system to help patients live as actively and comfortably as possible. Hospice is within the continuum of PC (refer to Figure 1) and is the most intensive, refined form of PC. Hospice denotes that the disease is incurable, acknowledges that attempts to slow disease progression have not been effective or have caused more suffering than benefit, and accepts that time is limited. It is reserved for terminally ill patients with a life expectancy of no greater than 6 months when the burdens of life-prolonging treatment outweigh the benefit, or no life-prolonging treatments are available. Death is the expected outcome of hospice, and the preeminent goals focus on enhancing the quality of life, comfort, and alleviation of suffering for patients and their families. Research consistently demonstrates a pattern of late referral to hospice for eligible patients, which leads to decreased benefits for patients and caregivers at EOL. When PC services are utilized earlier in the disease process, there is a notable improvement in the timely transition of patients into hospice care. In an attempt to resolve the long-standing confusion between PC and hospice care, the term nonhospice PC is emerging to more accurately reflect the broader scope that PC represents. Nonhospice PC was designed to address the limits placed on hospice eligibility and the clear need to improve the quality of care to those with serious illness that may not be terminal. Through education, planning, and leadership, PC programs have grown significantly (DeVita et al., 2023; WHO, 2023). A reported 7% of hospitals with 50 beds or more had a PC program in 2001, and in 2019, 72% of these hospitals had a PC program (Cross & Kavalieratos, 2023). By 2020, more than 83% of these hospitals reportedly had a PC program (CAPC, 2022).
Figure 1
The Continuum of Palliative, End-of-Life, and Hospice Care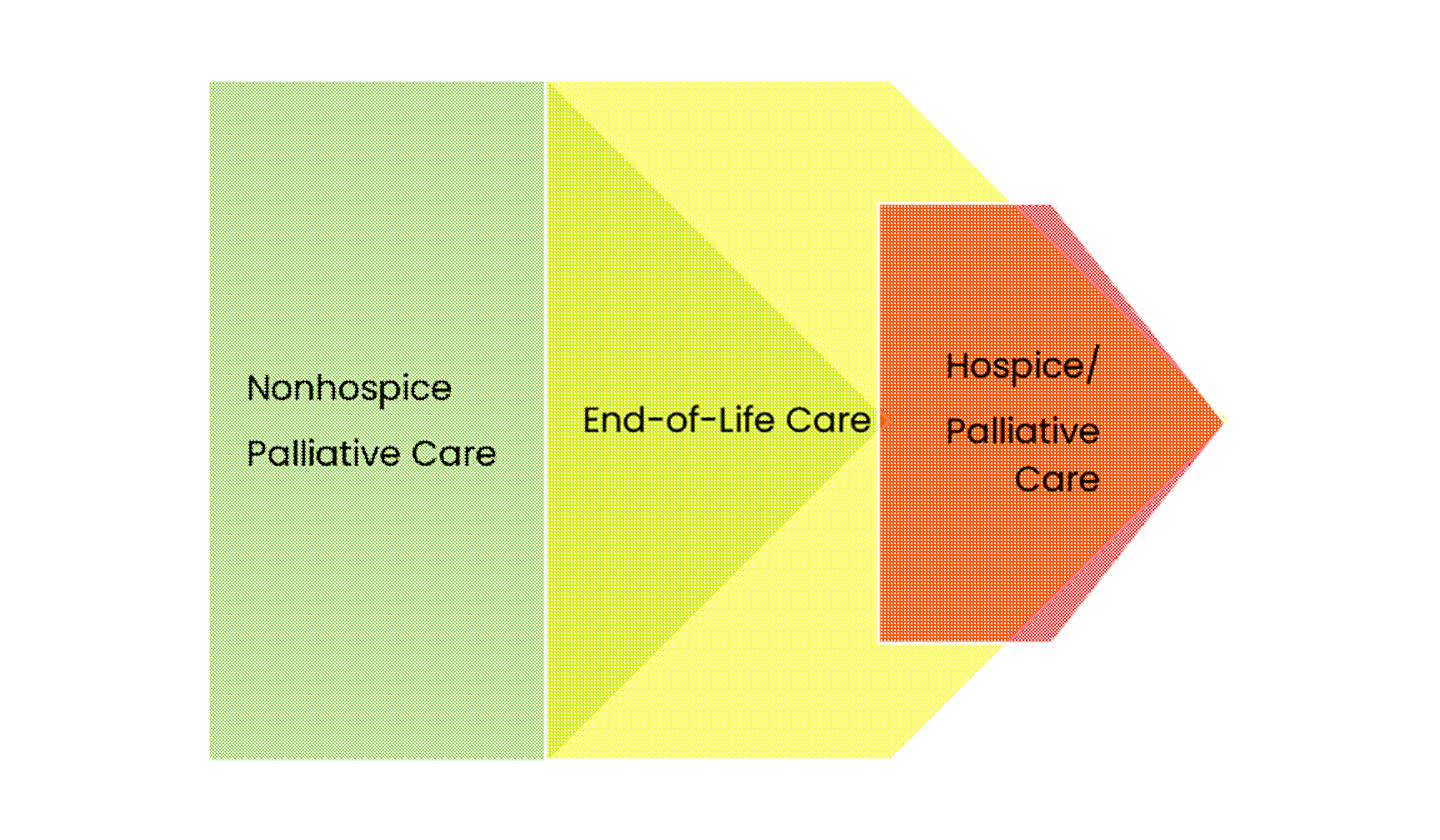
PC strives to fulfill the following objectives in patients with serious illnesses:
- to improve the patient’s quality of life and positively influence the course of illness with the goal of the patient living fully and at an acceptable comfort level throughout life
- to be utilized early in the patient’s disease trajectory and offered in conjunction with therapies and medications that are intended to prolong life (i.e., chemotherapy, radiation, and clinical trial drugs)
- to provide relief from pain and other distressing symptoms
- to integrate the psychological and spiritual aspects of patient care
- to address goals of care and ensure all care provided is aligned with patient wishes, including ACP and decision-making in preparation for the EOL
- to enhance care coordination through a team approach to care and facilitate communication among the health care team, patient, and family/caregiver
- to offer a support system to help the patient and family cope during serious illness (CAPC, n.d.; Meier & McCormick, 2024; WHO, 2023)
Models of Palliative...
...purchase below to continue the course
g>
PC is provided by specially trained HCPs, APRNs, registered nurses, and other clinical specialists who deliver additional patient support. Other clinical specialists that are often part of the PC interprofessional team include social workers, chaplains, physical therapists, massage therapists, occupational therapists, music and art therapists, and touch/energy therapists. Some health care institutions employ fully staffed PC teams comprising many of these multidisciplinary support services. In contrast, other institutions may have only one individual who is deemed responsible for delivering PC. PC is not setting-specific, as it can be provided through various channels (CAPC, n.d.; NCHPC, 2018). Although hospital-based inpatient PC services are the most common care delivery modality, PC can also be provided in outpatient settings such as:
- medical clinics or HCP offices
- long-term care facilities, including long-term acute care facilities
- skilled nursing facilities
- assisted living facilities
- group homes
- the patient’s home
- inpatient hospice facilities (Meier & McCormick, 2024; National Alliance for Care at Home, 2026)
PC is covered under Medicare Part B and Medicaid and may have a required copayment due at the time of service. Many private insurance providers also cover PC services. Despite what insurance provider the patient has, some treatments or medications may not be covered. Once the patient is eligible and elects hospice care, their care falls under the hospice benefit of Medicare Part A, Medicaid, or private insurance. Medicare and Medicaid cover all costs related to the terminal diagnosis, except that Medicare does not cover room and board if the patient lives in a care facility. The services covered include clinical and support services, medications, medical equipment (e.g., hospital bed, oxygen, walker, wheelchair, bedside commode), and supplies (e.g., dressing, ostomy, and incontinence). Most private insurances also cover all care related to the terminal diagnosis when the patient is in hospice; however, for some private insurance companies, the patient must first meet their deductible or pay a copayment (Kaye & Teshale, 2023; Meier & McCormick, 2024; National Alliance for Care at Home, 2026; US Centers for Medicare and Medicaid Services, n.d.).
The APRN and Nurse’s Roles in Palliative Care
Data from the US Centers for Disease Control and Prevention (CDC, 2025) reports that 90% of adults 65 years of age and older, 75% of adults 35–64 years of age, and 60% of adults 18–34 years of age have at least one chronic health condition. Over half of adults in the United States have at least two chronic health conditions. Heart disease, diabetes, and cancer are among the leading causes of death and disability, and annual health costs in the United States from these conditions are around 4.9 trillion dollars (CDC, 2025). With the continued growth of the aging population, these numbers are expected to rise over the next decade, and PC’s core principles and practices must be incorporated into routine clinical practice. PC lowers costs by reducing unnecessary hospitalizations, minimizing invasive diagnostic testing and interventions, and reducing emergency department visits at the end of life (EOF). Early involvement of PC can also reduce the length of stay in the intensive care unit (Meier & McCormick, 2024).
The NCHPC (2018) recommends that all clinicians and support staff working in patient care settings, especially primary care settings, acquire the core skills and knowledge regarding PC practice to reduce suffering. APRNs and nurses practice at the forefront of primary care across clinical settings and are, therefore, well-positioned to serve critical roles as members of the PC team. The NCHPC refers to these advanced practice providers as having the “ability to expand the capacity to deliver complex care and provide direct care” (NCHPC, 2018, p. 1). HCPs must first develop and continuously evaluate the plan to monitor and address psychological responses, emotions, or changes in cognition as prognosis and goals of care evolve during the trajectory of the illness. All nurses should serve as advocates for their patients’ sense of dignity and self-esteem by providing PC interventions to promote comfort and reduce suffering. The Hospice and Palliative Credentialing Center (n.d.) offers APRNs and nurses specializing in PC certification as an Advanced Certified Hospice and Palliative Nurse (ACHPN) or Certified Hospice and Palliative Care Nurse (CHPN). The role and specific interventions devised to meet the physical, spiritual, emotional, and psychosocial needs of the patient and family dealing with serious illness are summarized according to the NCHPC’s (2018) eight domains below.
Clinical Practice Guidelines for Quality Palliative Care
The NCHPC released the fourth edition of the Clinical Practice Guidelines for Quality Palliative Care in 2018. The guidelines are organized into eight domains and offer tools and resources to help clinicians provide optimal relief from symptoms and stressors associated with severe illness. These are generally applicable to both advanced practice and licensed nurses, indicated below with the umbrella term HCP (NCHPC, 2018). The eight domains are described in Table 1.
Table 1
The Eight Domains of Palliative Care
Domain 1: Structure and Processes of Care | - The healthcare provider (HCP) serves as a member of the interdisciplinary palliative care (PC) team, obtaining professional qualifications, education, and necessary training to acquire the core skillset.
- The HCP performs a comprehensive assessment and develops the PC plan aligned with the patient’s wishes.
- The HCP facilitates early referrals to PC and coordination of care, recognizing that communicating and collaborating with professional colleagues dramatically improves patient and family outcomes.
|
Domain 2: Physical Aspects of Care | - The HCP focuses on the screening, assessment, and treatment of symptoms, offering interventions to relieve distressing physical manifestations of the illness, as well as anticipating and preventing the symptoms associated with serious illness and its treatment.
- The HCP performs a comprehensive pain assessment and provides pain control that meets a level acceptable to the patient or the health care surrogate if the patient cannot report distress.
- The HCP performs ongoing assessments to determine the effectiveness of treatment and the need for modifications of the treatment plan, which serves as a means to effectively manage the symptoms associated with serious illness and treatments to improve well-being, functionality, and quality of life to a level acceptable to the patient or health care surrogate.
|
Domain 3: Psychological and Psychiatric Aspects of Care | - The HCP uses therapeutic communication to develop, maintain, and facilitate communication between the patient, family, and health care team to support the comprehension of information regarding disease progression and treatment choices.
- The HCP assesses the psychological and psychiatric aspects of care in the context of serious illness, including mental health assessment, suicidal ideation, preexisting psychiatric diagnoses, psychiatric diagnoses stemming from serious illness, or side effects of medications.
- The HCP uses clinical judgment and assessments to determine if referrals to mental health professionals, psychologists, or psychiatrists may be indicated; the advanced practice registered nurse (APRN) places referrals to mental health professionals, psychologists, and/or psychiatrists if indicated.
- The HCP advocates for patients when treating psychological issues such as anxiety, depression, hopelessness, posttraumatic stress disorder, substance use disorder, and withdrawal symptoms.
- The HCP performs ongoing monitoring and assessment of long-term and evolving psychological and psychiatric responses and mental health issues throughout the trajectory of illness and through end of life (EOL).
|
Domain 4: Social Aspects of Care | - The HCP integrates social assessments into the care plan to identify the social and practice needs, such as patient strengths; availability of caregiving and social support; access to reliable food, housing, and transportation; need for adaptive equipment; and other social or environmental issues.
- The HCP assesses and addresses social support needs, including family structure and function, roles, responsibilities, quality of relationships, communication, decision-making preferences, practical resources, and safety.
- The HCP assesses coping strategies and develops a care plan for social services and support congruent with the patient’s condition, goals, social environment, culture, and setting to maximize patient and family coping and quality of life.
|
Domain 5: Spiritual, Religious, and Existential Aspects of Care | - The HCP recognizes that spirituality is a core component of PC, through which patients and families may seek meaning, purpose, and transcendence while enduring serious illness and contemplating death.
- The HCP performs a spiritual assessment, ensuring that spiritual, religious, and existential aspects of care are addressed, including screening for unmet needs and referring to chaplains or other spiritual leaders as indicated.
- The HCP acknowledges that spirituality can be expressed through values, beliefs, traditions, rituals, or practices.
- The HCP understands that the patient may have beliefs that contrast with those of close family members; fosters the patient and family wishes regarding cultural rituals, customs, or practices; and avoids imposing individual beliefs on others.
|
Domain 6: Cultural Aspects of Care | - The HCP assesses and respects the patient and family values, beliefs, and traditions related to health and illness and acknowledges the impact of cultural influences on the PC delivery process.
- The HCP delivers culturally-sensitive care and avoids imposing personal biases or beliefs.
- The HCP practices cultural humility (“a process of openness, self-awareness, being egoless, and incorporating self-reflection and critique after willingly interacting with diverse individuals and embracing diversity”) (NCHPC, 2018, p. 61).
- The HCP participates in ongoing continuing education through cultural sensitivity training to acquire the skills to recognize how culture influences decision-making; their approach to illness; pain, psychological, social, and spiritual factors; and grief, death, and bereavement.
|
Domain 7: Care of the Patient Nearing the End of Life | - The HCP facilitates timely referrals to hospice in response to patients’ changing needs and ongoing adjustments to the care plan to meet all of the patient’s needs when nearing death.
- The HCP offers counseling and education about approaching death and the dying process and ensures adequate bereavement and grief support services are available to the family and care team.
- The HCP plays a vital role as death approaches and must be skilled in recognizing the signs and symptoms at EOL, including in the final days and weeks of life. HCPs should be aware of these changes:
- decreased level of consciousness
- muscle relaxation of the face
- labored breathing (dyspnea, apnea, Cheyne-Stokes respirations)
- hearing is not diminished
- touch is diminished, but the patient can feel the pressure of touch
- mucus collecting in large airways (i.e., terminal secretions, death rattle)
- incontinence of bowel or bladder
- mottling (cyanosis) occurring with poor circulation
- pupils no longer reactive to light
- bradycardia, weak pulse, and/or hypotension
- cool extremities
- perspiration
- decreased urine output
- inability to swallow
|
Domain 8: Ethical and Legal Aspects of Care | - The HCP applies the core ethical principles of PC, which include autonomy, substituted judgment (ethical duty of guardians and surrogate decision makers), beneficence, justice, and nonmaleficence, striving to prevent, identify, and resolve ethical dilemmas common to PC, such as:
- forgoing or discontinuing treatments
- establishing do not resuscitate (DNR) orders
- instituting state-specific portable medical orders, such as provider orders for life-sustaining treatment (POLST) and medical orders for life-sustaining treatment (MOLST)
- the application of sedation or pain control in the imminently dying patient
- The HCP facilitates appropriate referrals to ethics consultants or committees for decision-making and conflict-resolution assistance.
- The HCP honors patient autonomy by supporting patient preferences and decisions made by legal proxies or health care surrogates and is well-versed in the local and state laws related to advance care planning (ACP) and decisions regarding life-sustaining treatments.
- The HCP facilitates goals of care discussions and ACP, including discussing the importance of completing advanced directives.
|
(NCHPC, 2018)
Benefits of Palliative Care
Despite strong evidence that patients benefit from early integration of PC services and EOL discussions incorporating ACP, these concepts are still not routinely addressed in clinical practice. Prognosis affects patients’ choices about cardiopulmonary resuscitation (CPR) and additional life-sustaining measures at the EOL when adequately informed about their diagnosis. Unfortunately, many HCPs do not discuss goals of care due to a lack of time, discomfort, minimal experience discussing difficult topics such as death and dying, and fear of negatively affecting the patient’s and family’s hopes and coping with their diagnosis. However, EOL discussions do not cause emotional harm to patients and their families when done thoughtfully. When open communication regarding prognosis, treatment options, and goals of care occurs, there is an increase in patient satisfaction, decreased patient anxiety, improved outcomes and quality of life, and an increased likelihood that the patient will ultimately die in their preferred location. Bereaved families also report higher satisfaction and increased comfort of their loved ones when EOL and options for future care are discussed openly and honestly with the care team. They also report a better understanding of what to expect as their family member declines and ultimately dies due to disease progression. Thorough and open ACP also increases patient autonomy and reduces hospitalizations and the use of unwanted or unnecessary treatments, leading to decreased health care costs. ACP discussions have also led to decreased rates of ventilator use, resuscitation efforts, and intensive care unit admissions. These discussions can also lead to an appropriate change in code status and early referral to hospice. APRNs and nurses are often well-positioned to facilitate these open, honest conversations with patients and families to ensure a timely referral to hospice services. There is evidence that ACP discussions led by APRNs lead to an increase in the completion of advance directives, including clarified code status (LeBlanc & Tulsky, 2025; Meier & McCormick, 2024; Silveira, 2026).
The psychosocial support and coordination of care from the interdisciplinary PC team are other key benefits. Depression is more prevalent among patients with life-limiting serious illnesses, and it is linked to increased rates of mortality. An estimated 15%–60% of patients with a terminal illness have depression, but it is often underdiagnosed or undertreated due to the myth that this is expected. Depression that is not treated is associated with poor quality of life, decreased functioning, and a request for hastened death. Psychological support for family members and caregivers is also essential due to excess stress and caregiver strain. Spirituality often plays a vital role in how patients process their serious or terminal illness, with spiritual distress also contributing to requests for hastened death. Asking about a patient’s spiritual or religious beliefs benefits the care of patients with serious illness. Furthermore, PC is associated with support in navigating the complex, often fragmented health care system, including multiple specialists, treatment options, diagnostic testing results, and different care settings (Meier & McCormick, 2024).
For additional information regarding this topic and care at the EOL, please refer to the NursingCE.com courses, Ethical Considerations at the End-of-Life.
Advance Care Planning
ACP is a process that involves making decisions and having conversations about the types of health care treatment a person would want when they cannot make those decisions for themself. ACP can be completed at any age. Various factors, such as a mild chronic medical condition or a terminal illness with a limited life expectancy, can influence the timing of completion. ACP should be proactive, as its purpose is to ensure that individuals receive medical care that aligns with their values and goals. Regardless of the patient’s clinical picture, ACP should be incorporated into the care plan. As the patient’s clinical picture changes, ACP documents should be addressed and adjusted to meet the current needs and goals of the patient (Silveira, 2026).
ACP is a core aspect of PC, allowing patients to articulate and document their goals, values, and preferences. It supports shared decision-making and helps clinicians formulate a treatment plan and provide care that aligns with the patient’s preferences through EOL. Goals of care discussions and ACP are essential components of PC at all stages of illness but become increasingly dire as the patient’s health status declines. Ideally, primary care providers should encourage patients to identify a surrogate health care decision-maker (health care proxy) before the onset of illness or the loss of decision-making capabilities (Meier & McCormick, 2024; Silveira, 2026).
The COVID-19 pandemic emphasized the need for future planning and training for HCPs to conduct effective ACP discussions. One mnemonic used to support these discussions is GUIDE. This stands for:
- graph trajectory: draw or show a trajectory graph
- understand: assist in the patient’s understanding of the trajectory
- impact: assist patients in their understanding of how this impacts their lives
- death: review that death is a part of the disease, but does not need to be included in every conversation
- expect uncertainty: acknowledge that uncertainty is likely with associated emotional responses as changes occur (James & Lewin, 2024)
As with all aspects of care, there are legal and ethical dimensions surrounding ACP for the EOL. These are critical discussions that encompass serious decision-making during highly stressful times. Fundamental concepts of ACP include assessing the readiness of the patient and family to have these discussions, identifying a surrogate decision-maker(s), gauging patient and family understanding of the diagnosis and disease trajectory, discussing goals of care and treatment options, documenting the patient’s preferences in the electronic medical record, and readdressing as the disease progresses or treatment options change. Some of the fundamental components of ACP include advance directives, such as living wills and durable power of attorney for health care (DPOAHC; Meier & McCormick, 2024; Silveira, 2026).
Advance Directives
Advance directives are legally valid documents that address the specific treatments or medical care the patient wants and does not want if/when they cannot make decisions. These documents may also name secondary decision-makers authorized to speak for the patient if they are unable. The most common advance directives include a living will and a DPOAHC. It is important to note that a completed advance directive does not imply that an ACP was completed, and an in-depth ACP discussion does not also result in an advance directive, as patients may choose not to make choices or choose not to have these choices recorded. These documents do not go into effect until the patient loses the capacity to make their own decisions and can be changed at any point by the patient, either orally or in writing, as long as they have the cognitive function to do so.
- These must be completed while the patient maintains the mental capacity to make decisions.
- They should be reviewed yearly, if new major life events occur, and/or if there is a vital change in health status or a new diagnosis.
- Advance directives may be subject to state regulations. For instance, one state’s advance directive may not work in another state. Therefore, HCPs should counsel patients on the legal implications of traveling and the role of advance directives per their state’s guidelines.
- CaringInfo, a program of the National Alliance for Care at Home, offers free resources to help patients and clinicians make decisions about EOL care. CaringInfo also provides a website allowing patients and clinicians to download their state’s advance directive forms (CaringInfo, n.d.; National Institute on Aging, 2022; Silveira, 2026).
Living Will
A living will outlines the patient’s wishes regarding future medical treatment, including life-sustaining measures and procedures. It enables the patient to outline legal instructions regarding preferences for specific medical care when they cannot make decisions for themselves. For example, a living will may address CPR, mechanical ventilation, dialysis, and enteral nutrition and hydration. The document is known as a living will since it goes into effect while the patient is still living. For a living will to be valid, it must adhere to state guidelines. These guidelines differ from one state to another; some states require a living will to be standardized following a set outline, whereas others are more flexible and allow the individual more freedom in the language used as long as the document is signed and witnessed. Some states have specific guidelines regarding who can witness the signing of a living will. HCPs involved in an individual’s treatment are often not permitted to function as witnesses. Once the individual cannot make their own health care decisions, their living will go into effect. Many states have specific guidelines that dictate criteria to deem a patient unable to make medical decisions (National Institute on Aging, 2022; Silveira, 2026).
Durable Power of Attorney for Health Care
A DPOAHC identifies an individual whom the patient has elected to make health care decisions on their behalf. The terminology used to describe this individual varies from state to state, but examples include the health care proxy, health care agent, health care representative, or surrogate decision-maker. This individual is only given the authorization to make health care decisions once the patient becomes incapable of making their own decisions. When an individual chooses not to assign a surrogate, there is a specific legislation or process to authorize who is assigned this role (National Institute on Aging, 2022; Silveira, 2026).
For additional information regarding this topic, please refer to the NursingCE.com course titled Advance Care Planning.
References
Bischoff, K. E., Nouri, S., Rabow, M. W., Shah, A., Poree, L., & Sinavsky, K. (2026). CURRENT medical diagnosis & treatment 2026. McGraw-Hill. https://accessmedicine.mhmedical.com/book.aspx?bookid=3594
CaringInfo. (n.d.). What is an advance directive? National Alliance for Care at Home. Retrieved March 26, 2026, from https://www.caringinfo.org/planning/advance-directives/what-is-an-advance-directive
Center to Advance Palliative Care. (n.d.). What is palliative care? Retrieved March 26, 2026, from https://getpalliativecare.org/whatis
Center to Advance Palliative Care. (2022). Growth of palliative care in U.S. hospitals: 2022 snapshot (2000-2020). http://www.capc.org/documents/download/1031/
Cross, S. H., & Kavalieratos, D. (2023). Public health and palliative care. Clinics in Geriatric Medicine, 39(3), 395–406. https://doi.org/10.1016/j.cger.2023.04.003
DeVita, V. T., Jr., Lawrence, T. S., & Rosenberg, S. A. (2023). DeVita, Hellman, and Rosenberg’s cancer principles & practice of oncology (12th ed.). Wolters Kluwer.
Hospice and Palliative Credentialing Center. (n.d.). Certification. Retrieved March 26, 2026, from https://www.advancingexpertcare.org/hpcc
James, H., & Lewin, W. H. (2024). A GUIDE to help patients and families better understand serious illnesses: Mnemonic device provides way to teach learners about advance care planning. Canadian Family Physician, 70(1), 68–70. https://doi.org/10.46747/cfp.700168
Kaye, N. & Teshale, S. (2023). Paying for palliative care. National Academy for State Health Policy. https://nashp.org/paying-for-palliative-care
LeBlanc, T. W., & Tulsky, J. A. (2025). Discussing goals of care. UpToDate. Retrieved March 26, 2026, from https://www.uptodate.com/contents/discussing-goals-of-care
Meier, D. E., & McCormick, E. (2024). Benefits, services, and models of subspecialty palliative care. UpToDate. Retrieved March 26, 2026, from https://www.uptodate.com/contents/benefits-services-and-models-of-subspecialty-palliative-care
National Alliance for Care at Home. (2026). Facts and figures: 2025 edition. https://allianceforcareathome.org/wp-content/uploads/Facts-and-Figures-2025.pdf
National Coalition for Hospice and Palliative Care. (2018). Clinical practice guidelines for quality palliative care (4th ed.). https://www.nationalcoalitionhpc.org/wp-content/uploads/2020/07/NCHPC-NCPGuidelines_4thED_web_FINAL.pdf
National Institute on Aging. (2022). Advance care planning: Advance directives for health care. https://www.nia.nih.gov/health/advance-care-planning/advance-care-planning-advance-directives-health-care
Silveira, M. J. (2026). Advance care planning and advance directives. UpToDate. Retrieved March 26, 2026, from https://www.uptodate.com/contents/advance-care-planning-and-advance-directives
US Centers for Disease Control and Prevention. (2025). About chronic disease. https://www.cdc.gov/chronic-disease/about/index.html
US Centers for Medicare and Medicaid Services. (n.d.). Hospice care: Medicare Part A (hospital insurance) covers hospice care if you’re eligible. Retrieved March 26, 2026, from https://www.medicare.gov/coverage/hospice-care
World Health Organization. (2023). Palliative care. https://www.who.int/europe/news-room/fact-sheets/item/palliative-care#
Powered by Froala Editor
