About this course:
This course will provide an overview of the pathophysiology of pain, the components of a comprehensive pain assessment, and discuss nonpharmacological and non-opioid pharmacological management of pain. It will also discuss the core aspects of opioids for pain, proper monitoring of patients on long-term opioid therapy, and the clinical features of opioid misuse/OUD.
Course preview
Pain Management for RNs
This course will provide an overview of the pathophysiology of pain, the components of a comprehensive pain assessment, and discuss nonpharmacological and non-opioid pharmacological management of pain. It will also discuss the core aspects of opioids for pain, proper monitoring of patients on long-term opioid therapy, and the clinical features of opioid misuse/OUD.
By the completion of this module, the learner should be able to:
- define pain, discuss the pathophysiology of pain, and recognize the four main categories of pain
- identify the core components of a comprehensive pain assessment and describe the use of pain assessment scales and tools
- review the different types of nonpharmacological pain management strategies and interventional pain management procedures
- discuss the pharmacological management of pain using non-opioid and adjuvant analgesics
- define opioids and distinguish between opioid agonists, partial agonists, mixed agonist-antagonists, and opioid antagonists, and identify specific medications within each category
- demonstrate competency in monitoring patients on long-term opioid therapy
- recognize the potential for opioid misuse and abuse, the key features of opioid use disorder (OUD), and strategies to mitigate opioid misuse and OUD
Pain is a subjective individual experience for each person. In 1968, Margo McCaffery, a pioneer and world-renowned expert in pain management, defined pain as "…whatever the experiencing person says it is, existing whenever he says it does" (McCaffrey, 1968). In 2020, the International Association for the Study of Pain (IASP) revised its definition of pain for the first time since 1979 to the following: "an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage" (IASP, 2020). Pain cannot be objectively measured and depends on the individual's self-report. It is a complex perception with physiological, behavioral, and psychological components, with wide variability in each person's experience. Nevertheless, pain is the most common reason people seek medical care. Nurses must understand pain's underlying mechanisms and clinical features to deliver safe, effective, and personalized treatment plans (National Institute of Neurological Disorders and Stroke [NINDS], 2023a; Raja et al., 2020; Wager, 2022).
Pathophysiology of Pain
The purpose of pain is to prevent tissue damage and protect the body while healing, although its etiology is complex and multifaceted. The mechanism by which a stimulus is perceived as painful by the brain is not fully understood. Pain can be caused by mechanical, chemical, or thermal means. Mechanical pain is induced by trauma, injury, or overuse. It may be constant, variable, or intermittent. Chemical pain is associated with inflammatory disorders, and thermal pain is due to excessive heat or cold exposure. Neurons are messengers in the body responsible for connecting, receiving, and processing pain. They use electrical and chemical signals to transfer information between the brain, the spinal cord, and the rest of the body. Fundamentally, pain is felt when sensory nerve endings called nociceptors (or pain receptors) come in contact with a noxious (painful) stimulus. The noxious stimulus triggers three chief events: transduction, transmission, and modulation (see Table 1). A nerve impulse travels from the sensory nerve ending to the spinal cord, rapidly propelling it to the brain via the spinal cord and brainstem. The brain processes the painful sensation and responds with a motor response to terminate the inciting event. There are three primary types of neurons. Primary sensory neurons in the peripheral nervous system conduct painful sensations from the periphery to the dorsal root of the spinal cord. Secondary sensory neurons in the spinal cord or brainstem transmit the painful sensation to the thalamus. Tertiary sensory neurons communicate the painful sensation from the thalamus to the somatosensory areas of the cerebral cortex. Table 1 defines the primary pain processes and reviews important terminology (NINDS, 2023a; Wager, 2022; Watson, 2022a).
Table 1
Pain Processes: Terms and Definitions
Transduction is the conversion of noxious stimuli to an electrical impulse through specialized peripheral nerve fibers, also called nociceptors. Nociceptors are found throughout the body and activate a series of events in response to painful stimuli. The nerve endings detect mechanical, thermal, or chemical stimuli. Transduction occurs before the next process, transmission. |
Transmission occurs as the electrical impulse travels along the nerve fibers, where neurotransmitters regulate it. The signal is then transmitted to the dorsal horn of the spinal cord, where they are either dampened or amplified before being sent to the brain.
|
Modulation is the final process in the spinal cord; it causes muscles to contract reflexively, moving the body away from the painful stimuli. |
Perception occurs in various areas of the brain, with influences from thought and emotional processes. It refers to the patient's conscious awareness of pain as a culmination of pathophysiological processes and prior experiences. |
The pain threshold is the point at which a person feels pain. |
A person's pain tolerance is the maximum intensity of a pain-producing stimulus they are willing to accept in a given situation. |
Neurotransmitters are chemicals located throughout the nervous system released by neurons in response to cellular damage. They bind to and activate protein receptors on the surface of cells, which function as a gate to inhibit (block) or excite (transmit) a signal. Some of the neurotransmitters involved in the pain process include the following:
|
(Ignatavicius et al., 2020; NINDS, 2023a; Watson, 2022a; Yam et al., 2018)
The two major classes of nerve fibers associated with pain transmission include unmyelinated C fibers and myelinated A-delta fibers. Unmyelinated C fibers conduct impulses slowly and respond to thermal, mechanical, and chemical stimuli. They generate dull, aching, burning, diffuse, and delayed pain sensations. Myelinated A-delta fibers conduct impulses more rapidly, respond to mechanical (pressure) stimuli, and generate sharp, localized, and fast pain sensations. The spinothalamic tract is one of the central pain pathways. It originates in the spinal cord and extends to the thalamus. It transmits sensory information regarding pain, temperature, and touch. The spinoreticular tract is excited by similar sensory fibers as the spinothalamic tract, but instead of ascending to the thalamus, it terminates in the brainstem. Typically, there are two routes for conducting signal transmissions: ascending and descending. The ascending pathway travels upward, carrying sensory information from the body via the spinal cord toward the brain. The descending path travels downward from the brain to the organs via the spinal cord (NINDS, 2023a; Yam et al., 2018).
Categories of Pain
Pain is primarily categorized by duration (acute [less than one month], subacute [one to three months], and chronic [greater than three months]). It is also classified by origin (nociceptive or neuropathic) or the disease or condition that causes it (e.g., cancer, diabetes, rheumatoid arthritis [RA], etc.). Nociceptive pain includes somatic pain (skin, muscles, and soft tissues) and visceral pain (internal organs and lining of body cavities; Dowell et al., 2022; Ignatavicius et al., 2020; NINDS, 2023a).
Acute Pain
Acute pain is a warning sign or protective response that something in the body has been damaged, notifying the individual to respond to or escape the painful stimuli. It usually has a direct cause, resulting from disease, inflammation, or tissue injury. The etiology of acute pain is infinite, such as surgery, burns, invasive procedures, childbirth, or trauma. It is temporary and self-limiting, meaning it is confined to a defined period and often resolves with tissue healing. Acute pain may be accompanied by anxiety or emotional distress. Physiological responses to acute pain include activating the sympathetic nervous system or the body's inherent fight or flight response. Manifestations of the sympathetic response may include tachycardia, hypertension, increased respiratory rate, dilated pupils, diaphoresis, anxiety, and muscle tension. Behavioral responses to acute pain may consist of restlessness, moaning, flinching, grimacing, guarding, apprehension, and an inability to concentrate. Acute pain is usually treatable, and interventions strive to correct the underlying problem. However, if left untreated or unrelieved, acute pain can become maladaptive and lead to chronic pain (Ignatavicius et al., 2020; NINDS, 2023a).
Subacute Pain
Subacute pain is a subset of acute pain where the duration of pain falls between acute and chronic pain. It is a relatively newer concept recently incorporated into the updated Centers for Disease Control and Prevention (CDC) guidance on pain management. Subacute pain continues for 4 to 12 weeks, and common causes include low back pain, neck pain, and muscle strains (CDC, 2023a; Chou, 2023).
Chronic Pain
Chronic pain is a widely prevalent condition and is one of the most common reasons people seek healthcare services. According to the 2021 National Health Interview Survey, an estimated 51.6 million US adults (20.9% of the adult population) have chronic pain, and 17.1 million (6.9%) experience high-impact chronic pain (i.e., chronic pain that results in a substantial restriction to daily activities; Rikard et al., 2023). Chronic pain does not serve a protective function and is instead a pathologic (or dysfunctional) process. The onset is typically gradual, and symptoms are ongoing, unrelenting, persisting beyond tissue healing, and lasting longer than three months. Chronic pain is often poorly localized and can be challenging to describe. While chronic pain does not have the physiological response on the sympathetic nervous system that acute pain does, it is associated with significant morbidity, including disparaging physical and mental health conditions. In the US, chronic pain has been linked with depression, Alzheimer's disease (and related dementias), higher suicide risk, and substance use disorders (SUDs). Patients with chronic pain are also at higher risk for fatigue, functional impairment, disability, and financial burden. Chronic pain can interfere with personal and intimate relationships and contribute to social isolation or emotional distress. Management is aimed at symptomatic relief, although it is more resistant to medical treatment than acute pain and does not always respond to conventional interventions. If the underlying etiology cannot be identified, controlling the long-term effects of the pain is very challenging. Chronic pain can be idiopathic without an identifiable cause (Ignatavicius et al., 2020; Taylor et al., 2022; Watson, 2022a).
Some of the most common conditions causing chronic pain include low back pain (lumbago) and fibromyalgia. Low back pain is one of the leading causes of disability in Americans, as nearly 80% of adults are affected at some point in their lives. Low back pain profoundly affects patients, families, work productivity, and the economy. Determining the cause of low back pain can be difficult and expensive, costing the US nearly $100 billion annually. Low back pain can result from a prior injury that did not resolve or heal properly, poor body mechanics and posture, or wear-and-tear associated with aging (e.g., osteoarthritis [OA] and degenerative disc disease). Cancer-related pain is often considered a chronic pain condition attributed to tumor invasion, nerve compression, bone metastases, or as a byproduct of treatment, such as radiation therapy (Ignatavicius et al., 2020; NINDS, 2020; Taylor et al., 2022).
Fibromyalgia is a poorly understood chronic pain condition characterized by abnormal pain perception processing that affects about 4 million adults in the US. The etiology is not known. Patients experience many symptoms, including diffuse musculoskeletal pain, stiffness, fatigue, exercise intolerance, headaches, sleep disturbance, and cognitive impairment (e.g., memory and concentration problems). Fibromyalgia more commonly affects middle-aged women and patients with RA or lupus. The condition is treated with a combination of pharmacological and nonpharmacological interventions. Recommended lifestyle modifications include aerobic exercise, stress management, cognitive-behavioral therapy, and sleep hygiene (CDC, 2020a). Table 2 provides a comparison chart of acute and chronic pain features.
Table 2
Acute versus Chronic Pain
Acute Pain | Chronic Pain |
Short duration, temporary, reversible | Longer duration (usually lasts more than three months), ongoing, long-lasting, may be irreversible |
Localized and generally has a well-defined etiology | Often poorly localized and may not have a well-defined etiology |
Pain is acute and declines with tissue healing | Pain is gradual and persists, even without identifiable injury or cause |
May ignite the sympathetic nervous system's “fight or flight” response | Does not impact the sympathetic nervous system function |
(Ignatavicius et al., 2020; Rikard et al., 2023; Taylor et al., 2022)
Nociceptive Pain
Nociceptive pain is the physiologic response arising from tissue injury or damage caused by a noxious stimulus. There are two main categories of nociceptive pain: somatic and visceral. Somatic pain is further subdivided by the location of the pain receptors, which includes cutaneous or superficial (skin and subcutaneous tissues) and deep somatic (fascia, musculoskeletal, blood vessels, bone, joint capsules, and connective tissues). Stimulation of somatic pain receptors typically produces well-localized pain that may be described as sharp, dull, aching, or burning. Examples of somatic pain include incisional pain, wound complications, muscle spasms, and peripheral vascular disease. Visceral pain receptors are located within internal organs, the lining of the body cavities (e.g., stomach or intestines), and surrounding connective tissue. Visceral pain is poorly localized, diffuse, and described as deep cramping, sharp, or shooting. Examples of visceral pain include colitis, pancreatitis, bladder spasms, and appendicitis. Visceral pain from an injury to an organ capsule or other deep connective tissues may also be described as sharper and more localized. As shown in Figure 1, visceral pain can cause referred pain in different body locations separate from the site of the noxious stimulus (Ignatavicius et al., 2020; Watson, 2022a).
Figure 1
Map of Referred Visceral Pain

Neuropathic Pain
Neuropathic pain results from damage to or dysfunction of the nervous system, inducing hyperalgesia (i.e., pain out of proportion to the injury). Neuropathic pain is usually described as intense, shooting, or burning and can be characterized by sensory abnormalities, such as paresthesia (e.g., numbness, tingling, or "pins and needles"). Allodynia, or pain due to a stimulus that does not normally provoke pain, is another common manifestation of neuropathic pain. The pain may occur in an area other than the one stimulated. Opioid use in patients with neuropathic pain is controversial, as opioids are not typically effective. First-line pharmacologic therapy typically includes antiepileptic drugs (AEDs), antidepressants, antispasmodics, and skeletal muscle relaxants. Many types of neuropathic pain conditions are chronic and relentless. Four common neuropathic pain conditions are described below (postherpetic neuralgia, trigeminal neuralgia, diabetic neuropathy, and phantom limb pain; Ignatavicius et al., 2020).
Postherpetic Neuralgia (PHN)
PHN is a highly painful and debilitating complication of the herpes zoster (Shingles) virus. Shingles is caused by varicella-zoster virus (VZV) reactivation, which lies dormant in the dorsal root ganglia of the spinal cord following varicella (chickenpox) infection. While a typical shingles rash resolves within a few weeks, PHN results from damage to the sensory nerves, affecting the nerve fibers and skin, and can persist for weeks, months, or longer. According to the CDC (2019), up to 18% of people diagnosed with shingles will experience PHN. The risk for PHN increases with age, as people younger than 40 rarely experience this condition. Hyperalgesia and allodynia following the resolution of the skin rash are among PHN's most prominent clinical manifestations. Antiviral medicines are recommended to treat shingles as they shorten the length and severity of the illness. Antivirals are most effective if initiated immediately (ideally within 48 hours) after the first symptoms appear (CDC, 2019, 2022b; Ignatavicius et al., 2020).
Treatment of PHN is challenging, and effective relief often requires a multidisciplinary approach. Nonpharmacologic strategies to reduce pain include warm, wet compresses to the site, calamine lotion, and colloidal oatmeal baths (a lukewarm bath mixed with oatmeal). Commonly prescribed pharmacologic agents include the following:
- lidocaine (Lidoderm) patches
- tricyclic antidepressants (TCAs) such as nortriptyline (Pamelor) and amitriptyline (Elavil)
- serotonin-norepinephrine reuptake inhibitors (SNRIs) such as duloxetine (Cymbalta) and venlafaxine (Effexor)
- gabapentinoids such as gabapentin (Neurontin) and pregabalin (Lyrica)
To prevent this debilitating condition and its associated complications, the CDC (2022b) recommends all adults aged 50 and older receive the recombinant (inactivated) zoster vaccine (RZV, Shingrix). Shingrix is administered as a two-dose series, two to six months apart. It is also recommended for adults aged 19 and older with weakened immune systems from disease or therapy. The live zoster vaccine (ZVL, Zostavax) has been unavailable in the US since November 2020 (CDC, 2019, 2022b; Wald & Johnston, 2022).
Trigeminal Neuralgia (TN)
TN, or tic douloureux, is a severe pain condition affecting the fifth cranial nerve, inducing excruciating, shock-like burning pain. It usually affects one side of the face near the jaw or cheek, and the intensity of the pain is so severe that it can be physically and mentally debilitating. TN pain can be sporadic and intermittent, often called "attacks of pain,” that occur regularly for days to weeks or longer. Pain attacks occur several times daily and can be triggered by contact with the face or cheek (such as brushing teeth, applying makeup, eating, or light touch). Diagnosis and treatment of the condition are equally complex. Management involves a combination of pharmacological and nonpharmacologic strategies. Most patients do not find relief from traditional pain-relieving medications such as acetaminophen (Tylenol), nonsteroidal anti-inflammatory drugs (NSAIDs), or opioids. Carbamazepine (Tegretol), an AED, is considered the gold standard for the initial pharmacologic treatment of TN. AEDs such as carbamazepine (Tegretol), oxcarbazepine (Trileptal), and topiramate (Topamax) are used to block nerve firing. TCAs such as nortriptyline (Pamelor) and amitriptyline (Elavil) can also be effective. TCAs inhibit the reuptake of serotonin and norepinephrine at the synapse. Increasing the level of these neurotransmitters in brain tissue inhibits the chemical processes in the brain that cause people to feel this type of neuropathic pain. Common nonpharmacological therapies used alongside medications for TN include acupuncture, biofeedback, and electrical stimulation of the nerves. Surgical treatment may be advised if all other management strategies fail (NINDS, 2023b).
Diabetic Neuropathy
Diabetic neuropathy is nerve damage caused by diabetes or poor blood glucose control over time. It can develop slowly after many years of elevated blood glucose levels or occur relatively early in the disease. There are a few types of diabetic neuropathies depending on which nerves are damaged, but the most common is peripheral neuropathy, which affects the legs, feet, and toes. Diabetes is the most common cause of peripheral neuropathy, responsible for up to 53% of cases, and painful diabetic neuropathy occurs in more than 16% of patients with diabetes (Price et al., 2021). Diabetic neuropathy can impair movement and cause problems with balance and coordination. It can also affect how people process sensations (e.g., hot and cold), leading to muscle weakness and other complications such as foot infections and ulcers. People with diabetes may also experience focal neuropathies, such as damage to a single nerve in a specific body part, called entrapment syndromes. The most common entrapment syndrome is carpal tunnel syndrome. Autonomic neuropathy is also seen in people with diabetes, which damages the nerves that control the internal organs. Autonomic neuropathy can lead to digestive dysfunction, bladder dysfunction, or ocular retinopathy. These conditions can contribute to the overall morbidity among this population. Nonpharmacologic treatment strategies include proper foot hygiene, wearing appropriate footwear, weight loss, and physical therapy (including balance and gait training; Castelli et al., 2020; National Institute of Diabetes and Digestive Kidney Diseases [NIDDK], 2018).
The American Academy of Neurology (AAN) 2021 practice guideline update on the treatment of painful diabetic neuropathy supports the following treatment options for diabetic neuropathy:
- TCAs, such as nortriptyline (Pamelor), amitriptyline (Elavil), and imipramine (Tofranil)
- gabapentinoids such as gabapentin (Neurontin) and pregabalin (Lyrica)
- SNRIs, such as duloxetine (Cymbalta), venlafaxine (Effexor), and desvenlafaxine (Pristiq)
- AEDs such as oxcarbazepine (Trileptal), lamotrigine (Lamictal), and valproic acid (Depakene; Price et al., 2021)
Topical medications, including lidocaine (Lidoderm patches) and capsaicin, can also be added to oral medications. As with other neuropathic pain conditions, opioids should not be used routinely because of their limited effectiveness (Castelli et al., 2020).
Phantom Limb Pain
Phantom limb pain is the perception of pain in a limb that no longer exists. After losing a body part, affected individuals describe phantom limb pain as stabbing, shooting, burning, and throbbing. Allodynia is a common manifestation. Risk factors include older age at the time of amputation, lower limb amputation, and bilateral limb amputation. Treatment is complex and often requires a combination of strategies. Nonpharmacologic therapies include heat application, physical therapy, biofeedback, transcutaneous electrical nerve stimulation (TENS), message, and acupuncture. Pharmacologic treatments include injections with local anesthetics and/or steroids, nerve blocks, NSAIDs, opioids, antidepressants, AEDs, and muscle relaxants (Amputee Coalition, n.d.; Ignatavicius et al., 2020).
Risk Factors for Pain
Several risk factors have been reported to increase the risk for pain conditions. Some of the most common include the following:
- advancing age
- lower socioeconomic status, such as those living in poverty
- occupational-associated risks (e.g., manual labor involving heavy lifting or inactivity due to a desk job, poor posture, and improper body mechanics)
- less than a high school education
- public health insurance
- sedentary lifestyle, being overweight or obese
- presence of specific underlying health conditions such as cancer (tumor invasion, nerve compression, bone metastases, associated infections, immobility, prescribed treatments), arthritis, fibromyalgia, and neuropathy
- trauma
- surgery
- invasive diagnostic or treatment procedures (Rikard et al., 2023; NINDS, 2023a)
Factors Affecting the Pain Experience
Nurses must be cognizant of the various factors affecting a patient's pain experience, which can complicate the diagnostic workup. Some of the most common factors that impact the individual pain experience are listed in Table 3.
Table 3
Factors Impacting the Pain Experience
Age | Age can influence how pain is perceived, diagnosed, and treated.
|
Cognitive function | Cognitively impaired patients may be unable to report pain or describe it accurately. |
Fatigue | Fatigue can heighten pain sensitivity. |
Genetic sensitivity | Genetics can increase or decrease pain tolerance. |
Prior experience | Prior experiences with pain can increase or decrease sensitivity, depending on whether adequate pain relief was obtained. |
Anxiety | Anxiety and fear can increase pain sensitivity. |
Support and coping | Support systems and coping styles can impact the pain experience positively or negatively. For example, positive coping skills and robust social support systems can decrease sensitivity to pain, whereas poor coping skills or lack of support can heighten pain sensitivity. |
Culture | Culture influences how patients may express pain or the meaning they attach to pain. For example, some cultures see pain as a sign of weakness and discourage people from openly reporting or describing pain. |
(Rabow et al., 2020)
Risk Factors for the Undertreatment of Pain
The undertreatment of pain is a severe problem across the US that has been intensified by the opioid epidemic and restrictions on opioid prescribing guidelines in recent years. In 2021, the American Medical Association (AMA) released a letter calling for the CDC to modify its 2016 opioid prescribing guidelines, which limit access to opioids by imposing dosage limitations on prescribers. According to the AMA (2021), physicians have reduced opioid prescribing by more than 44% since 2012, yet the drug overdose epidemic has worsened. Therefore, they have asked the CDC to restructure the guidelines and incorporate the view that pain sufferers must be “treated as individuals” (AMA, 2021). This led to the recently updated 2022 CDC’s Clinical Practice Guideline for Prescribing Opioids for Pain, which will be discussed later in this course (Dowell et al., 2022).
Undertreated pain severely impacts physical and mental health, such as increased anxiety with acute pain and depression with chronic pain. According to the US Department of Health and Human Services (HHS, 2019b), some of the most common risk factors associated with the undertreatment of pain include:
- cultural and societal attitudes toward pain (stigma)
- lack of knowledge and education regarding pain and appropriate management
- fear of addiction among patients and healthcare providers
- reduced healthcare provider willingness to prescribe opioids due to legislative changes and perceived liability and legal consequences
- the exaggerated fear of respiratory depression
- barriers to accessing care (lack of insurance coverage and payment for pain modalities or access to pain specialists)
- specific populations: infants and children, older adults, and patients with SUD (HHS, 2019b)
Pain Assessment
All patients should be screened for pain as the first step in a comprehensive pain assessment. The most valid pain assessment is self-report, although this can be influenced by several factors (e.g., mood, culture, cognitive abilities, etc.). Since pain is a subjective experience, a thorough and reliable assessment is vital to accurately diagnosing it and determining the most effective treatment plan. A pain assessment is comprised of the following components:
- a pain interview using a validated pain assessment scale
- a thorough history, including a review of all prior pain experiences, medications, and treatments
- physical examination, including a functional assessment of abilities and deficits
- psychosocial assessment
- assessment of past and current opioid use and opioid tolerance (Rabow et al., 2020).
Scales and Tools
The patient's self-report of pain severity should be evaluated using an appropriate scale, such as the Numeric Rating Scale (NRS), where 0 refers to "no pain" and 10 denotes "the worst pain imaginable." Other pain severity scales include the Visual Analogue Scale (VAS) and the Defense and Veterans Pain Rating Scale (DVPRS). In addition, pain severity scales for individuals with verbal communication deficits related to cognitive impairment or dementia include the following:
- FACES Pain Scale (displayed in Figure 2)
- Adult Non-Verbal Pain Scale (NVPS)
- Pain Assessment in Advanced Dementia Scale (PAINAD)
The FACES scale is also widely utilized in pediatric pain assessment. Pain severity scales that allow for pain assessment using various physical features representative of pain include the Behavioral Pain Scale (BPS) and the Critical Care Pain Observation Tool (CPOT). In conjunction with the pain severity assessment scales described above, additional assessment tools help define and classify pain. The OPQRST tool is one of the most common instruments utilized. It reviews the following features of pain: onset, provocation and palliation of symptoms, quality, region, radiation, severity, and timing (University of Florida [UF] Health, n.d.). An overview of the clinical use and application of the OPQRST tool is outlined in Table 4.
Figure 2
The VAS, FACES, and NRS Pain Assessment Tools

Table 4
Symptom Analysis Using the OPQRST Tool
Onset Ask the patient about the onset of the pain.
|
Provocation/Palliation of symptoms Document associated findings: fatigue, depression, nausea, anxiety.
Aggravating/relieving factors
|
Quality Quality refers to how the pain feels: sharp, dull, aching, burning, stabbing, pounding, throbbing, shooting, gnawing, tender, heavy, tight, tiring, exhausting, sickening, terrifying, torturing, nagging, annoying, intense, or unbearable.
|
Region and Radiation Use anatomical terminology and landmarks to describe the location of pain (superficial, deep, referred, or radiating).
|
Severity Intensity, strength, and severity are “measures” of the pain.
|
Timing Timing includes the duration and frequency of the pain.
|
(UF Health, n.d.)
In addition to the above, it is also helpful to ask patients about the setting of pain, such as how it affects their daily life, activities of daily living (ADLs), sleep, and school or work. Some questions to ask may include:
- “Where are you when the symptoms occur?”
- “What are you doing when the symptoms occur?”
- “How does the pain affect your sleep?”
- “How does the pain affect your ability to work or interact with others?”
(UF Health, n.d.)
History and Physical Examination
The patient's medical and surgical history should be evaluated, including a detailed account of all prior trauma or injuries. An allergy and medication history, including the use of OTC medications and supplements, is essential. The nurse should inquire about the patient’s history with prior or current pain relief measures, including pharmacological and nonpharmacological modalities and the success or failure of each strategy. Information regarding the patient's previous experience with opioids should be explored during the initial pain assessment to determine if the patient is opioid-tolerant. It is critical to identify risks for OUD prior to opioids becoming part of the patient’s treatment plan. Behaviors complement self-report and assist in pain assessment of nonverbal and verbal patients. Direct observation of the patient's nonverbal behavioral manifestations may indicate the presence of pain. Facial expressions (grimacing, wrinkled forehead, wincing), body movements (restlessness, pacing, guarding), and audible expressions (crying, wincing, moaning) can all indicate the presence of pain. Other physical examination findings indicating pain include decreased attention span and altered vital signs. Blood pressure, pulse, and respiratory rate increase temporarily with acute pain. However, vital signs will eventually stabilize with the persistence of pain. Therefore, physiologic indicators might not accurately measure chronic pain or pain that is present over time (Bickley et al., 2020).
The nurse should perform a focused physical assessment related to the reported pain, including the neurological and musculoskeletal systems. In patients with clinical suspicion of neuropathic pain, signs of nerve injury may or may not be seen on the neurological exam. Some patients may demonstrate sensory deficits, such as dull, pinprick, sharp touch, temperature, or vibration alterations. Allodynia or hyperalgesia may be displayed as an exaggerated response to stimuli. Autonomic changes in the temperature and color of the extremities and hair and nail growth can accompany neuropathic pain. The patient should be evaluated for impairments in mobility, such as gait disturbance, imbalance, loss of muscle tone, reflexes, coordination, and strength (Bickley et al., 2020).
Psychosocial Examination
Pain can impair many aspects of an individual’s psychological function and social well-being. The patient should be screened for psychosocial impacts of pain, such as disturbances in sleep, mood, activity, energy, appetite, and overall functioning. In addition, the patient's ability to fulfill ADLs, work, or school responsibilities should be explored. Pain can also impair cognition and memory or negatively impact relationships with significant others, family, friends, and colleagues. Patients should be screened for suicidal ideation due to the increased risk with chronic pain conditions (Bickley et al., 2020).
Assessment of Pain in Older Adults
It is well-cited that the incidence of pain is higher among the older adult population, who are more likely to experience pain at multiple sites. Yet, they receive fewer analgesics, and pain management is suboptimal. Older adults tend to report less pain than younger adults, which may be related to beliefs about pain, concerns about reporting pain, or cognitive deficits. They may underestimate their pain by attributing it to the ‘normal’ aging process. Research demonstrates that many older adults believe pain must be lived with, and reporting pain is an unacceptable sign of weakness. Pain may be associated with being a "bad" patient or signify impending death or severe illness, which is therefore ignored. Fear of becoming addicted to opioids may also contribute to the older adult's reluctance to report pain. Patients and their caregivers may also be concerned about the side effects of medications or polypharmacy. Those with cognitive impairments, hearing or visual deficits, and dementia are at increased risk for undertreated pain. Special consideration should be given to the older adult population when evaluating pain. Appropriate pain scales should be utilized based on the patient’s cognitive functioning. Pain should be reassessed at each visit, and the scale should be explained each time. Attention should be paid to nonverbal indicators of pain, such as facial expressions, body movements, grimacing, guarding, and behavioral changes. In some patients, it may be helpful to avoid using the word pain and replace it with alternative verbal descriptions such as "ache," "sore," or "hurt" (Hosseini et al., 2022; Ignatavicius et al., 2020).
Developing the Pain Management Treatment Plan
An ideal pain management plan should address the etiology of pain, control current pain, and manage pain that persists despite treatment. According to the HHS (2019b), a pain management treatment plan should incorporate a biopsychosocial model with individualized, multimodal, and multidisciplinary strategies, integrating treatments from different clinical disciplines. As depicted in Figure 3, the biopsychosocial model of health correlates the various biological, psychological, and social facets of pain. A multifaceted approach to pain has been shown to enhance pain control, reducing pain severity and improving mood, overall quality of life, and functionality (HHS, 2019b).
Figure 3
The Biopsychosocial Model of Health

(Adapted from MrAnnoying, 2016)
Pain treatments are considered in terms of efficacy, safety, tolerability, and invasiveness. There are two main classes of pain control: nonpharmacologic, which includes restorative therapies, interventional procedures, behavioral health approaches, and complementary therapies, and pharmacologic, which includes medications (opioid and non-opioid analgesics). Best practice guidelines recommend that pain interventions begin on the low end of invasiveness. These include psychological and physical treatments, such as restorative therapies and physical exercise programs, which will be outlined in the next section. However, the efficacy of a specific treatment does not necessarily match its degree of invasiveness (HHS, 2019b).
Nonpharmacological Pain Management Strategies
Nonpharmacological strategies should not replace pharmacological pain measures; they should be used alongside them for a synergistic effect. Nonpharmacologic pain management strategies serve as a means to restore functionality, enhance comfort, reduce pain, and diminish the amount and duration of analgesics required. These strategies also help to mitigate opioid exposure when clinically indicated (HHS, 2019b).
Restorative therapies include treatments provided by physical therapy (PT) and occupational therapy (OT) professionals to promote positive clinical outcomes in various acute and chronic pain conditions. Therapeutic exercise refers to movement therapies to recover from injury, reduce inflammation, and restore health under the guidance of a trained physiotherapist. Cutaneous (skin) stimulation includes TENS therapy, heat, cold, therapeutic touch, massage, acupuncture, and acupressure. These physical modalities increase circulation, reduce pain, and are self-care alternatives to narcotics. Some of the most common include:
- TENS therapy involves a small, battery-operated electric stimulator attached to the skin at the affected area(s). The device is used at home and administers a low-voltage electrical current to block the pain sensation (see Figure 4).
- Heat application causes vasodilation, promoting blood flow to the area, and is an easily accessible self-care pain relief modality. When using heating pads or other types of heating devices, it is essential to check the device policy regarding how long the treatment can be safely used. In most cases, the treatment is discontinued after 15 to 30 minutes. When applied for over one hour, the body reduces blood flow to the skin through a vasoconstrictive reflex response. Dry heat applications may include aquathermia and disposable heat pads, which are most commonly used in healthcare facilities. Moist heat can be applied using a lukewarm moist compress or soaking a body part using a sitz bath. Most healthcare settings do not use hot water bottles since improper use can lead to burns.
- Cold application reduces swelling and helps to alleviate pain. Ice bags, collars, and gloves are applied to localized ailments. As with heat application, the device policy should be followed regarding how long the treatment may be safely used. The treatment is generally discontinued after 5 to 10 minutes or when the area begins to feel numb. Prolonged exposure to cold, as with heat, results in reflex vasodilation.
- Therapeutic touch is considered a pain reduction technique as it is believed to reduce pain through balance in the body. The therapist places their hands near the patient's body to balance the patient's energy field. Reiki is a natural healing technique in which a therapist channels energy into a patient by touch to promote physical and emotional healing.
- Massage can help reduce pain using several types of massage therapy. Swedish massage uses long strokes, kneading, and deep, circular movements; deep tissue (myofascial release) focuses on myofascial trigger points and the deeper layers of tissue. Massage stimulates circulation, relaxing the patient's muscles, reducing anxiety, and decreasing pain. Massage should be avoided when skin integrity is impaired or if infection or blood clot is possible.
- Acupuncture and acupressure involve stimulating subcutaneous tissues using needles (acupuncture) or the digits (acupressure). Only individuals with specialized training should perform these techniques.
- Therapeutic ultrasound delivers heat and enhances blood flow to deep tissues for improved and accelerated injury healing (Berger & O’Neill, 2022; HHS, 2019b).
Figure 4
TENS therapy

Cognitive‑behavioral therapy (CBT) is another component of the multimodal pain management approach. CBT centers on developing a solid therapeutic relationship that encourages patients to adopt a problem-solving approach to cope with the challenges associated with chronic pain. It focuses on changing how patients perceive pain to reduce distress, alleviate or suppress discomfort, and improve coping skills. The overarching features of CBT include short-term, problem-focused, cognitive, and behavioral interventions. It is not a one-size-fits-all model, as there are several variations. CBT teaches patients to restructure cognitive distortions and self-defeating behaviors and replace them with more accurate thoughts and functional behaviors. CBT is time-limited and typically consists of 8 to 16 sessions. In addition to face-to-face and telephone, sessions can also be administered via computer-based programs, referred to as computer-based (Craske, 2017; Lim et al., 2018). Distraction techniques direct attention toward something other than the pain, as it is well-documented that decreased attention to the presence of pain can reduce the perceived pain level. Distraction techniques can be useful during painful diagnostic procedures or while waiting for an analgesic to take effect. Specific strategies include ambulation, deep breathing, visitors, television, games, prayer, and music (Berger & O’Neill, 2022).
Relaxation techniques are commonly used for pain management and may also be utilized during CBT. Relaxation strategies may include meditation, yoga, and progressive muscle relaxation. Meditation involves focusing on an object while sitting comfortably and clearing the mind of all thoughts. Meditating for 20 minutes twice daily decreases heart and respiratory rates and blood pressure. Yoga has been practiced in India for centuries and typically includes assuming poses, breathing exercises, and meditation. Yoga increases muscle strength and tone, reduces anxiety, and lowers blood pressure. Progressive muscle relaxation involves slow, deep abdominal breathing while progressively tightening and relaxing the muscles. The technique is typically performed in a logical sequence, beginning with the feet and moving up the rest of the body. Guided imagery involves pleasant and serene mental images such as the ocean or mountains. This technique shifts the patient's thoughts away from the pain. It can be useful during painful diagnostic procedures. However, patients must be able to concentrate to benefit from guided imagery, which makes this technique more difficult for patients with acute and severe pain. Biofeedback is a therapy that uses electric sensors to assist a patient in controlling physiological responses such as heart rate and blood pressure (Berger & O’Neill, 2022; HHS, 2019b).
Interventional Pain Procedures
Interventional pain management uses minimally invasive interventions to alleviate pain and minimize pharmacological therapies. Most interventional pain procedures are performed on an outpatient basis and are, therefore, more cost-effective. Procedures vary in their degree of complexity and invasiveness. Some are considered minor procedures that can be performed in the outpatient office setting, whereas others require image guidance (using ultrasound, fluoroscopy, or computed tomography [CT]) in a radiology department. Commonly used interventional pain procedures include the following:
- Trigger point injections use dry needling or local anesthetic to inject and disrupt palpable, tense bands of skeletal muscle fibers to relax and lengthen the fibers. These may be done intramuscular or intrabursal (i.e., to treat bursitis).
- Joint injections use a corticosteroid and/or a local anesthetic injected into the facet joint(s) or intra-articular (such as the shoulder, elbow, wrist, knee, ankle, etc.) to manage arthritis or injury.
- Peripheral or sympathetic nerve blocks use a local anesthetic mixed with a corticosteroid. The mixture is injected or infused around a specific nerve or group of nerves to treat or diagnose postoperative pain, neuropathies, neuropathic pain, and chronic pain. An example is a celiac plexus block, which may help relieve abdominal pain related to chronic pancreatitis.
- Epidural steroid injections involve injecting corticosteroids into the epidural space (outside the dural sac in the spine) to treat neuropathic leg pain (related to a nerve root irritation in the low back) or arm pain (less common, related to a nerve root irritation in the neck).
- Radiofrequency ablation uses high-frequency energy waves (conventional or pulsed) to ablate or stun nerves contributing to pain.
- Neuromodulation involves activating the central or peripheral nerves using electrical, ultrasound, or magnetic stimulation devices to relieve pain or reduce sensitivity. An example includes vagus nerve stimulation to treat cluster and migraine headaches (Figure 5).
- Spinal cord stimulators utilize the concept of neuromodulation (above) in a permanently implanted stimulator along the lower spinal cord to manage lower extremity neuropathic pain.
- Implanted intrathecal pain pump allows for the delivery of opioids, baclofen (Lioresal), or other medications directly into the spinal fluid to receptors on the spinal cord or the brain using a fraction of the dose required with oral administration, reducing many of the adverse drug effects. Risks include infection/meningitis, delayed respiratory depression, granuloma formation, and hypogonadism (HHS, 2019b).
Figure 5
Vagus Nerve Stimulation
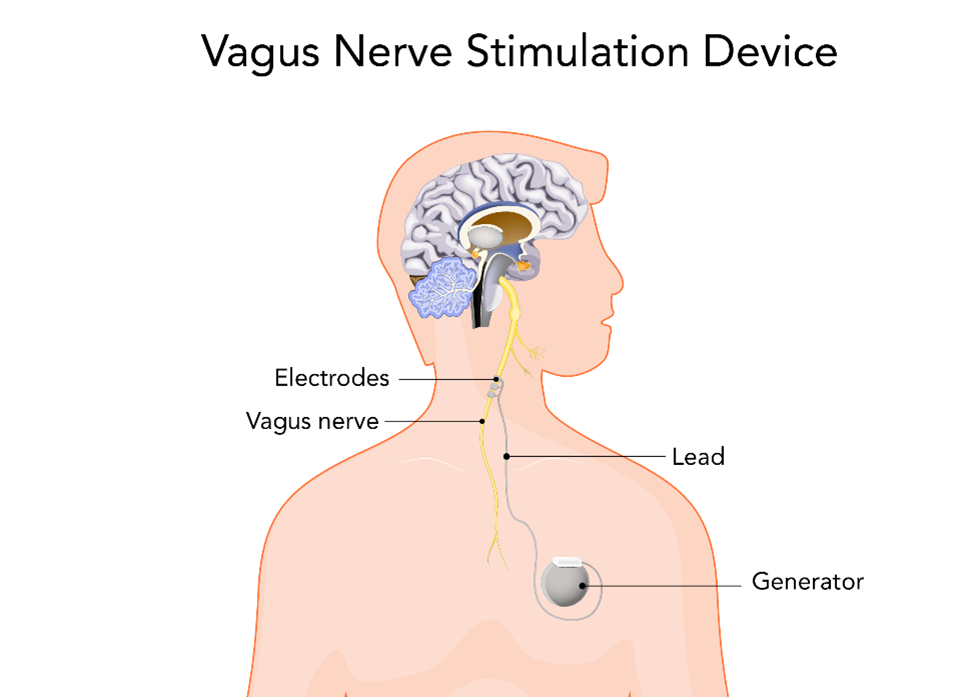
Pharmacological Interventions
Pharmacologic therapy is usually a component of an effective, multimodal pain management plan, particularly for treating chronic pain. Analgesics are a mainstay for relieving pain and are comprised of two main categories: nonopioids and opioids (HHS, 2019b).
Nonopioid Analgesics
Nonopioid analgesics have anti-inflammatory, antipyretic, and analgesic effects. However, the properties of the different medications vary, as each drug has its independent mechanism of action, risks, benefits, and potential side effects. Non-opioid medications can mitigate and minimize opioid exposure (HHS, 2019b). Two of the most common nonopioid analgesics are NSAIDs and acetaminophen (Tylenol). These medications are appropriate for the treatment of mild to moderate pain. They are easily accessible to patients since they do not require a prescription. First-generation NSAIDs include ibuprofen (Motrin, Advil), indomethacin (Indocin), diclofenac (Zorvolex), ketorolac (Toradol), and meloxicam (Mobic). First-generation NSAIDs inhibit COX-1 and COX-2, which are forms of the enzyme cyclooxygenase (COX). COX creates prostanoids (i.e., prostaglandins, prostacyclins, and thromboxanes), which are responsible for the inflammatory response. While COX-1 and COX-2 are integral to the inflammatory process, COX-1 also affects the gastrointestinal (GI) tract and kidney and platelet function. Therefore, when COX-1 is inhibited by first-generation NSAID therapy, inflammation, pain, and fever are reduced, but gastric ulceration, renal impairment, and bleeding can occur. First-generation NSAIDs are also given to prevent stroke and myocardial infarction (MI) and to treat pain caused by arthritic conditions such as OA and RA. Second-generation NSAIDs, such as celecoxib (Celebrex), inhibit only COX-2, decreasing inflammation, pain, and fever without impacting platelet aggregation. Second-generation NSAIDs are commonly prescribed for pain caused by arthritis, ankylosing spondylitis, and dysmenorrhea (Ghlichloo & Gerriets, 2022; HHS, 2019b; U.S. Food & Drug Administration [FDA], 2020a).
While NSAIDs can significantly relieve many types of pain, they are not without risks. NSAIDs are associated with GI, cardiovascular, and renal effects. The most common side effects include GI bleeding, gastric ulcers, acute kidney injury, bleeding events, heart failure from sodium retention, MI, and stroke. Not all NSAIDs pose the same severity of risk. Cardiovascular risks, including thrombosis and MI, are heightened in COX-2 selective NSAIDs such as celecoxib (Celebrex); the GI side effects are reduced. While semi-selective NSAIDs such as meloxicam (Mobic) and indomethacin (Indocin) pose less cardiovascular risk than COX-2 selective agents, they should still be used cautiously in patients with cardiovascular risk factors. GI risks such as bleeding and ulcers are increased in nonselective NSAID medications, including ibuprofen (Motrin) and naproxen (Naprosyn; Ghlichloo & Gerriets, 2022).
The American Geriatrics Society (AGS) Beers Criteria (BC) for Potentially Inappropriate Medication Use in Older Adults publishes medications that should be avoided in this population. The BC recommends avoiding indomethacin (Indocin), ketorolac (Toradol), ibuprofen (Motrin), and meloxicam (Mobic) due to the risk of GI bleeding, peptic ulcer disease, and kidney damage. Instead, they recommend replacing these medications with celecoxib (Celebrex), naproxen (Aleve), or ibuprofen (Motrin) in combination with a proton pump inhibitor (PPI) for GI protection. Misoprostol (Cytotec) and PPIs such as omeprazole (Prilosec) or pantoprazole (Protonix) reduce the GI risk but do not eliminate them (AGS, 2019).
Aspirin, also known as acetylsalicylic acid (ASA), is the oldest NSAID. It is the most widely used drug globally and has proven to be lifesaving in preventing cardiovascular disease (Desborough et al., 2017). Due to its antiplatelet properties, many providers prescribe a dose of 81 mg to 325 mg once daily as prophylaxis for MI. The emergent treatment for acute MI includes the administration of chewable non-enteric coated aspirin (162 to 325 mg) at the first recognition of symptoms. Acetylsalicylic acid (ASA) is not without risks. While it is considered cardioprotective at low doses, it carries an increased risk for GI side effects, including gastric bleeding and ulcers (Desborough et al., 2017; Runde et al., 2022).
Salicylism toxicity (i.e., aspirin poisoning) is a medical emergency caused by the intentional or accidental overdose of salicylates. This potentially fatal condition develops when aspirin levels rise above the therapeutic range and can occur from the acute ingestion of large doses of aspirin at one time or from chronic intake of smaller quantities over an extended period. The most common signs of salicylism toxicity include ringing in the ears (tinnitus), dizziness, and headache. Serious symptoms include hyperventilation, agitation, fever, convulsions, disorientation, confusion, hallucinations, respiratory arrest, and coma. The condition has high morbidity and mortality; at least 1-2% of patients will die. Overdose of other NSAIDs such as ibuprofen (Motrin, Advil) can also occur and present with manifestations similar to aspirin poisoning; however, generally, they are not as severe. Reye syndrome is a rare but serious complication that occurs when aspirin is administered for fever reduction in children and adolescents with a viral illness, such as chickenpox or influenza. Reye syndrome affects all body organs but is most damaging to the brain and the liver. It causes increased intracranial pressure and substantial fat accumulation in the liver. Pediatric patients should never be given aspirin to manage a fever. Awareness of this syndrome has dramatically reduced its occurrence (Desborough et al., 2017; Runde et al., 2022).
Acetaminophen (Tylenol) is one of the most popular analgesics in the US, with over 60 million Americans consuming acetaminophen (Tylenol) products every week. Acetaminophen (Tylenol) alleviates pain, fever, allergy, cough, cold, flu, and sleeplessness. It is often an ingredient in OTC cough and cold remedies. Like aspirin, acetaminophen (Tylenol) blocks pain by inhibiting prostaglandin synthesis of COX-1 and COX-2, suppressing pain and fever. However, acetaminophen (Tylenol) does not suppress inflammation or platelet aggregation. The FDA also enforced the need for all acetaminophen (Tylenol) products to include boxed warnings, highlighting the potential for severe liver injury, including liver failure, with overuse (Agrawal & Khazaeni, 2023; FDA, 2018a; Orandi et al., 2023).
Acetaminophen (Tylenol) overdose is a significant cause of overdose-related liver failure and death in the US. It is responsible for more than 55,000 emergency department visits, 2,600 hospitalizations, and 500 deaths in the US annually; however, when identified early, mortality rates are low (Agrawal & Khazaeni, 2023). Patients should be encouraged to check the labels of all analgesics to determine the amount of acetaminophen (Tylenol) contained in the product. Further, frequent alcohol use while taking large doses of acetaminophen (Tylenol) heightens the risk of liver damage. Patients with preexisting liver conditions such as cirrhosis, fatty liver, or hepatitis, as well as those who consume more than three alcoholic drinks per day, should limit or avoid acetaminophen (Tylenol) as much as possible. Acetaminophen (Tylenol) is rapidly absorbed through the duodenum, and about 90% of the drug is metabolized in the liver. The onset of liver injury is rapid. Diagnosis is characterized by marked elevations in plasma aminotransferases (liver enzymes) and rising prothrombin time/international normalized ratio (PT/INR; Burns et al., 2023). The clinical course of acetaminophen (Tylenol) poisoning moves through four sequential stages as follows:
- Stage I (30 minutes to 24 hours): nausea, vomiting, lethargy, diaphoresis, and pallor
- Stage II (24 to 72 hours): laboratory evidence of hepatotoxicity and nephrotoxicity become apparent, including hyperbilirubinemia, elevated PT, and clinical manifestations such as right upper quadrant (liver) pain, tenderness, and hepatomegaly
- Stage III (72 to 96 hours): elevations in liver function enzyme tests peak by 96 hours (plasma alanine transaminase [ALT] and aspartate aminotransferase [AST] levels may exceed 10,000 IU/L), hyperbilirubinemia (bilirubin usually exceeds 4.0 mg/dL), and clinical manifestations such as jaundice, confusion (hepatic encephalopathy), bruising or bleeding, oliguria, and multiorgan system failure ensue. Death most commonly occurs during stage III.
- Stage IV (four days to two weeks): patients who survive stage III enter a recovery phase that usually begins on the fourth day following the overdose. Patients often develop chronic liver changes, including necrosis and chronic liver disease, and may eventually need a liver transplant (Agrawal & Khazaeni, 2023; Burns et al., 2023).
GI decontamination with activated charcoal (AC) is recommended for adults who present within four hours of potentially toxic acetaminophen (Tylenol) ingestion (i.e., a single dose of 7.5 g or greater). AC is a gastric lavage technique that induces emesis, limiting the absorption of acetaminophen (Tylenol) and reducing the need for N-acetylcysteine (Acetadote) treatment. N-acetylcysteine (Acetadote) is the antidote for acetaminophen (Tylenol) overdose/poisoning and should be given to all patients at significant risk for hepatotoxicity. However, severe hepatotoxicity is uncommon, and death is rare when this antidote is administered within eight hours of overdose. Acetylcysteine decreases the build-up of hepatotoxic metabolites to prevent or lessen liver damage. It can be given orally or intravenously, and several protocols available for administration vary according to institution policy and patient tolerance (Heard & Dart, 2022).
Adjuvant Analgesics
Adjuvant analgesics are medications prescribed alongside a primary analgesic, such as an opioid analgesic, to enhance pain control. Adjuvant analgesics include AEDs, topical analgesics, TCAs, SNRIs, anxiolytics, skeletal muscle relaxants (SMRs), glucocorticoids, and bisphosphonates. The goal is to generate a synergistic effect, heightening pain relief while reducing the need for and dosage of opioids. A reduced dosage of opioids minimizes the risk of adverse effects, opioid dependency, and subsequent OUD. Adjuvant medications can also help alleviate other symptoms that aggravate pain, such as depression, seizures, inflammation, and anxiety. While adjuvant analgesics are not opioids, they still carry risks for adverse effects and require close monitoring (Qaseem et al., 2017; Schwenk, 2023; Watson, 2022b).
AEDs
AEDs are medications initially developed to treat seizures but are also commonly used to treat specific pain syndromes. As mentioned, these drugs are particularly effective for treating neuropathic pain and migraines. Increasingly, they are being incorporated into a multimodal approach to managing perioperative pain to reduce the need for opioids postoperatively. Gabapentinoids such as gabapentin (Neurontin) and pregabalin (Lyrica) are commonly prescribed for chronic neuropathic pain such as PHN, diabetic neuropathy, and fibromyalgia (HHS, 2019b). They act as inhibitors of voltage-gated calcium channels and suppress neuronal excitability, which makes them optimal analgesia for neuropathic pain. Pregabalin (Lyrica) is similar to gabapentin (Neurontin) but contains a different active ingredient and has more stable pharmacokinetics. While gabapentin (Neurontin) and pregabalin (Lyrica) effectively treat nerve pain, they have several side effects, including sedation, fatigue, dizziness, visual disturbance, mood swings, depressive episodes, and suicide attempts. They are known to increase the risk of suicidal thoughts or behavior in about 1 in 500 people. Therefore, these medications should be used cautiously in patients with concomitant psychiatric conditions or those with a history of depression, suicidal thoughts, ideation, or attempt. Patients and caregivers should be counseled on monitoring for mood changes, such as new or worsening depression, anxiety, restlessness, panic attacks, anger, irritability, agitation, aggression, dangerous impulses, violence, and suicidal thoughts or behaviors (HHS, 2019b; Schwenk, 2023; Viatris Inc., 2022).
As mentioned earlier, carbamazepine (Tegretol) is the first-line treatment for the initial medical management of TN. Carbamazepine (Tegretol) inhibits voltage-gated sodium channels, reduces the excitability of neural membranes, and potentiates GABA receptors. The most common adverse effects include dizziness, sedation, disturbances in concentration, ataxia, and visual disorders such as diplopia. Other potentially severe but uncommon adverse effects include Stevens-Johnson syndrome, systemic lupus erythematosus, toxic epidermal necrolysis, hepatotoxicity, hyponatremia, and aplastic anemia. In addition, patients should be educated on the importance of avoiding grapefruit or grapefruit juice while taking carbamazepine (Tegretol) as it inhibits the drug’s metabolism and can increase adverse effects (Bendtsen et al., 2019; NINDS, 2023b; Schwenk, 2023).
Topical Analgesics
Topical lidocaine (Lidoderm) patches are FDA-approved for PHN but are also used for other pain conditions. Lidocaine (Lidoderm) is considered a safe, well-tolerated, and effective treatment option for certain types of localized pain. It poses a low risk for systemic effects as only a tiny fraction of the dose reaches the systemic circulation and may be used for extended periods. Furthermore, it eliminates the potential for abuse, addiction, dependence, or tolerance. Available by prescription only, it is dispensed as a medicated patch comprised of a 5% lidocaine-containing hydrogel adhesive. The patch is applied to the affected area and remains in place for 12 hours, exerting localized analgesic effects without inducing numbness. It decreases nerve membrane permeability to sodium ions, inhibiting depolarization and transmitting pain signals. In addition, there is an associated cooling effect that accompanies the application of the hydrogel to the affected area. Patients must be instructed to apply the patch to intact skin for no longer than 12 hours, then remove it for at least 12 hours before a new patch is applied. The most common adverse effects include local skin irritation, erythema, and inflammation at the application site. Lidocaine (Lidocaine viscous) is also available as a gel or cream (Endo Pharmaceuticals, 2018).
Capsaicin (Capsagel, Salonpas) is a topical analgesic derived from chili pepper extract, a neuropeptide-releasing agent that targets peripheral sensory neurons. It is applied to the skin to control peripheral nerve pain, and its benefits in managing chronic neuropathic pain have been widely studied. Available primarily OTC in the form of a gel or patch, it depletes neurotransmitters of substance P, thereby reducing pain perception. However, it has several potential adverse effects, such as pain, erythema, pruritus, skin eruptions (e.g., rash, lesions, vesicles, skin dryness, hives), and swelling at the application site (Derry et al., 2017).
TCAs
TCAs help reduce neuropathic pain and various other chronic pain conditions. Amitriptyline (Elavil) and nortriptyline (Pamelor) are the most prescribed TCAs for pain. They have independent analgesic properties and are also known to potentiate the effects of opioids. These medications block the reuptake of serotonin and norepinephrine at the synapse in the brain, which helps improve mood and treat depression. For pain, they act on the descending pain pathways involving serotonin, norepinephrine, and endogenous opioids. While TCAs are widely studied for their benefits in relieving pain, they are associated with several adverse effects which make tolerance difficult. Some of the most common include orthostatic hypotension, dry mouth, dizziness, weight gain, memory impairment, urinary retention, constipation, sedation, tachycardia, and cardiac conduction abnormalities (particularly QTc interval prolongation; Schwenk, 2023; Sheffler et al., 2023; Wang et al., 2018).
Patients should be advised to take the medication at bedtime to minimize the effects of orthostatic hypotension and sedation. Additional instructions for patients experiencing adverse effects while taking TCAs include the following:
- avoid sudden changes in position and sit or lie down if feeling dizzy
- increase fluid intake and sip fluids throughout the day
- increase fiber intake
- increase physical activity
- take a stimulant laxative and a stool softener as needed (Schwenk, 2023; Wang et al., 2018)
- TCAs should be avoided/used with caution in older adults secondary to their anticholinergic effects (AGS, 2019)
SNRIs
According to the HHS (2019b), SNRIs, such as duloxetine (Cymbalta) and venlafaxine (Effexor), are helpful for a variety of chronic pain conditions, including musculoskeletal pain, fibromyalgia, and neuropathic pain conditions. SNRIs block the reabsorption of serotonin and norepinephrine around nerve cells. This increases the amount of serotonin and norepinephrine available in the brain, which also helps improve mood. The primary benefit of SNRIs over TCAs is that they have better safety profiles and significantly fewer adverse effects, which leads to greater tolerability and increased compliance. In addition, SNRIs are associated with a reduced risk of drowsiness, cognitive impairment, and cardiac conduction abnormalities. However, these medications are not without risks, as they can potentially cause hepatotoxicity, anorexia, fatigue, and sexual dysfunction. Duloxetine (Cymbalta) is FDA-approved for diabetic neuropathy and fibromyalgia but is also used for chronic musculoskeletal pain. Venlafaxine (Effexor) is not FDA-approved for any pain conditions, but it is commonly used off-label for treating neuropathic pain and other chronic pain. A benefit of these medications is their concurrent effect on mood disorders. As with all antidepressants, patients must be assessed for suicidal thoughts or ideations before starting therapy and reassessed throughout treatment (CDC, 2020a; HHS, 2019b; Schwenk, 2023; Sheffler et al., 2023; Wang et al., 2018).
Anxiolytics
Anxiolytics, or antianxiety medications, are commonly prescribed to treat anxiety accompanying acute pain. In addition, they are sometimes used to manage anxiety from fluctuations in chronic pain. Most anxiolytics are classified as CNS depressants. They inhibit the activity of the GABA and create a calming effect. Benzodiazepines are one of the most common classes of anxiolytics used in patients for pain management. These include medications such as lorazepam (Ativan), alprazolam (Xanax), and triazolam (Halcion). Anxiolytics are usually prescribed to treat generalized anxiety, panic attacks, acute stress reactions, muscle spasms (e.g., diazepam [Valium]), seizure disorders (e.g., clonazepam [Klonopin]), and sleep disorders. In general, these drugs require great caution and monitoring. They are indicated for short-term use only due to their high risk of tolerance, dependence, and addiction. Concurrent use of benzodiazepines and opioid pain medications requires heightened caution due to the additive risks of interaction between them (National Institute on Drug Abuse [NIDA], 2020a).
Older adults have increased sensitivity to benzodiazepines and decreased metabolism of long-acting agents. Since all benzodiazepines increase the risk of cognitive impairment, delirium, falls, fractures, and motor vehicle crashes in older adults, the BC recommends avoiding use for insomnia, agitation, or delirium. However, they may be appropriate for other indications such as seizure disorders, rapid eye movement, sleep behavior disorder, severe generalized anxiety disorder, and periprocedural anesthesia (AGS, 2019). Benzodiazepines should also be avoided in pregnant and breastfeeding patients, as they are known to cross the placenta and are excreted in breast milk. In addition, they have been shown to increase the risk of congenital abnormalities, primarily if used during the first trimester (FDA, 2018a).
SMRs
SMRs are commonly prescribed agents for muscle spasms associated with painful conditions, such as low back pain. The American College of Physicians (ACP) recommends using SMRs before opioids if pharmacologic treatment is desired to treat low back pain (Qaseem et al., 2017). However, a recently published analysis of data from randomized studies showed that among patients in the emergency department with acute low back pain, SMRs do not improve outcomes over NSAIDs or placebo (Abril et al., 2022). SMRs, such as cyclobenzaprine (Flexeril) and carisoprodol (Soma), work by potentiating norepinephrine, antagonizing serotonin, and binding to acetylcholine receptors to block the neuromuscular junction. They are associated with CNS effects, such as sedation and dizziness, and carry anticholinergic effects, such as mouth, constipation, urinary retention, reduced muscle contraction, and blurred vision. Some SMRs have specific indications, such as baclofen (Lioresal), which is used to treat painful spasticity associated with specific underlying neurological conditions (e.g., stroke, spinal cord injury, or multiple sclerosis; Qaseem et al., 2017). The CDC (2020b) cautions against prescribing SMRs in combination with opioids due to the increased risk of synergistic CNS effects such as drowsiness and sedation. Further, SMRs should be avoided or used with extreme caution in older adults secondary to their anticholinergic and CNS effects (AGS, 2019).
Glucocorticoids
Glucocorticoids, otherwise known as corticosteroids, reduce pain by decreasing inflammation. They are efficacious in treating painful inflammatory conditions such as RA and gout. Some of the most common agents include dexamethasone (Decadron), methylprednisolone (Medrol Dosepack), and prednisone (Deltasone). Long-term systemic corticosteroid use poses several health consequences, including hyperglycemia, bone loss, skin thinning, cataracts, weight gain, elevated glucose, immunosuppression, and adrenal insufficiency. Corticosteroids can also cause mood and behavioral changes, including irritability and aggression. Therefore, these medications are not advised for long-term use and should be tapered down as soon as possible. Due to the risk of adrenal insufficiency and withdrawal symptoms, corticosteroids should not be discontinued abruptly or tapered down too quickly. Withdrawal symptoms include weakness, severe fatigue, body aches, lightheadedness, and irritability (Berger & O’Neill, 2022).
Bisphosphonates
Bisphosphonates, such as alendronate (Fosamax) and ibandronate (Boniva), are typically indicated for the prevention and treatment of osteoporosis. Specific medications, such as denosumab (Xgeva) and zoledronic acid (Zometa), are also used for cancer-related bone pain from bone metastases or primary bone cancer. They inhibit osteoclast cell activity, decrease bone turnover, and increase bone density. Bisphosphonates carry serious risks, including irritation of the upper GI tract, hypocalcemia, medication-related osteonecrosis of the jaw (MRONJ), and atypical femur fracture (AFF). Before starting bisphosphonate therapy, patients should be educated on the risks and warnings associated with bisphosphonate therapy. They should have a prophylactic dental evaluation and follow up regularly with their dentist during treatment (American Association of Clinical Endocrinologists and the American College of Endocrinology [AACE/ACE], 2020).
Opioid Administration and Monitoring
It is vital that nurses properly understand terms related to opioid use, such as tolerance, dependence, and addiction, as there are many misconceptions related to these concepts, which may contribute to the inadequate treatment of pain (Berger & O’Neill, 2022; Dowell et al., 2022). Key concepts associated with opioid use are defined in Table 5
Table 5
Terminology Associated with Opioid Use
Term | Definition |
Tolerance | Tolerance is a state of adaptation in which exposure to an opioid induces changes that decrease one or more of the drug's biological effects over time. As a result, the individual requires higher doses of the medication over time to maintain the same level of response or effects. |
Physical and psychological dependence | Physical dependence is the body's physical adaptation to a drug. The medication becomes necessary for normal body functioning, and symptoms of withdrawal develop when the drug is no longer present in the patient's body; this can be caused by abrupt cessation or rapid dose reduction of the drug or the administration of an antagonist (i.e., naloxone [Narcan]). Psychological dependence occurs when ingesting the medication becomes associated with alleviating pain, anxiety, or depression. The presence of the drug becomes a calming and reassuring presence in the patient's life, similar to a comfort or security object (NIDA, 2020b). According to the US Substance Abuse and Mental Health Services Administration (SAMHSA, 2021), dependence is defined when patients meet three or more of the following seven criteria:
|
Addiction | Addiction is a chronic, neurobiological disease that has contributing genetic, psychosocial, physical, and environmental factors and influences, manifested by behaviors that include one or more of the following:
|
Pseudotolerance | Pseudotolerance is the misconception that increasing doses are needed due to tolerance rather than disease progression or other factors. |
Pseudoaddiction | Pseudoaddiction is the faulty assumption of addiction in a patient seeking relief from pain. It is manifested by a patient becoming intensely fearful of being in pain. Pseudoaddiction is common in postoperative patients and usually manifests as clock-watching, asking to be awoken to receive pain medication, and hypervigilance with documenting and monitoring pain medication administration. Pseudoaddiction usually resolves with effective pain management treatments and the resolution of painful stimuli; for postoperative patients, this is the healing of the surgical site. |
Misuse | Misuse is the nonmedical use of opioids and is characterized by taking an opioid in a manner or dose other than prescribed (e.g., taking the drug to get high or taking someone else's prescription). |
Prescription drug diversion | Prescription drug diversion is the unlawful channeling of regulated pharmaceuticals from legal sources to the illicit marketplace; legitimately made controlled substances that are diverted from their lawful and medically necessary purpose into illegally trafficked drugs. |
(Berger & O’Neill, 2022; Hudspeth, 2016; NIDA, 2020b; SAMHSA, 2021; HHS, 2019b)
Opioids
Opioids are a group of controlled substance analgesics prescribed for moderate to severe pain. They can be natural (derived from the opium poppy plant), synthetic (human-made), or semi-synthetic. They interact with opioid receptors on nerve cells to reduce pain signals and sensation by binding to and activating opioid receptors (i.e., mu, delta, and kappa) spread diffusely throughout the CNS. Attaching to one of these receptors reduces or blocks the pain signals sent from the brain to the body, releasing dopamine throughout the body, thereby altering pain perception and response. Opioids can also affect receptors in the respiratory and GI tract, leading to occasional use for diarrhea and cough. Opioids are classified as agonists, partial agonists, and mixed agonist-antagonists. Opioid antagonists may be used to counteract the adverse effects of opioids. Although opiates and opioids may be used interchangeably, they have different meanings. Opiates include natural opioids such as heroin, morphine, and codeine, whereas opioids include all-natural, synthetic, and semi-synthetic opioids such as oxycodone (Roxicodone) and fentanyl (Duragesic; Berger & O’Neill, 2022; CDC, 2021a; NIDA, 2021).
Opioid Agonists
Opioid agonists produce a maximum biological effect between receptor binding and response. Opioids vary in the ratio of their analgesic potency and their potential for respiratory depression (Berger & O’Neill, 2022). Adverse reactions to opioid agonists include respiratory depression, drowsiness, mental confusion, nausea/vomiting, dizziness, headache, fatigue, pruritus, pinpoint pupils, urinary retention, and constipation. Since opioids induce euphoria, particularly when taken in higher doses than prescribed or ingested via snorting or injection, they carry an increased risk for abuse and addiction. In addition, long-term opioid use poses an increased risk of drug tolerance and hyperalgesia from damage to nociceptors (HHS, 2019b; NIDA, 2021; Paul et al., 2021). According to the HHS (2019b), the most common opioid agonists prescribed for moderate or severe pain include:
- Hydrocodone (Vicodin, Lortab, Norco): found only in combination products, usually combined with acetaminophen; may be oral tablet formulation or liquid cough syrup
- Oxycodone (Roxicodone, Oxycontin): available as an IR or ER formula, fast onset, available in oral tablet or solution form
- Morphine sulfate (Roxanol, MS Contin): available as an IR or ER formula in parenteral and oral formulations
- Oxymorphone (Opana, Opana ER): available as an IR or ER formula, long half-life in parenteral and oral formulations
- Hydromorphone (Dilaudid, Exalgo ER): derivative of morphine, but with a faster onset, available as an IR or ER formula in oral tablet, liquid, suppository, and parenteral preparations (HHS, 2019b)
Some of the most common opioid agonists are listed according to their origins in Table 6.
Table 6
Opioid Analgesics
Natural | Synthetic | Semi-Synthetic |
Morphine sulfate (Roxanol, MS Contin) | Fentanyl (Duragesic) | Oxycodone (Roxicodone) |
Codeine (Tylenol #3) | Hydrocodone (Vicodin) | |
Meperidine (Demerol) | Hydromorphone (Dilaudid) | |
| Levorphanol (Levo-Dromoran) | Oxymorphone (Opana) |
(Berger & O’Neill, 2022; CDC, 2021a)
Fentanyl (Duragesic) is a highly lipid-soluble opioid administered through various parenteral modalities, including transdermal, transmucosal, intranasal, spinal, and intravenous via patient-controlled devices. Fentanyl dosing is in micrograms due to its high potency; it is 50 to 100 times more potent than morphine sulfate (Roxanol, MS Contin). Methadone (Dolophine) is a long-acting opioid used for neuropathic pain and OUDs. The half-life of methadone (Dolophine) is significantly longer than morphine (8 to 59 hours), with lipophilic storage, so caution is advised when using this drug to treat pain safely. However, it is considerably cheaper than other medications and is widely dispensed in SUD clinics as a component of medication-assisted treatment (MAT) for OUD. Since it is long-acting, it can delay the opioid withdrawal symptoms that patients experience when taking short-acting opioids, allowing time for detoxification (Dydyk et al., 2023; Paul et al., 2021). Codeine is a relatively weak opioid agonist commonly used to treat mild to moderate pain or cough. It can be administered alone, combined with acetaminophen (Tylenol-Codeine #3), or as part of cough and cold formulas (HHS, 2019b; NIDA, 2021; Paul et al., 2021).
Partial Agonists
Partial agonists activate opioid receptors to a lesser degree than full agonists. Low doses provide similar effects to full agonists, but the analgesic activity plateaus when the doses are increased; thus, they have a ceiling effect. Therefore, increasing dosages of these medications typically lead to more adverse effects without improved pain relief. Examples of partial agonists include tramadol (Ultram) and buprenorphine (Suboxone). Tramadol (Ultra) is a synthetic analog of codeine with a low affinity for opioid receptors commonly used to treat moderate to severe pain. It has a dual mechanism of action and poses less abuse potential than other opioids. It is available in IR or ER oral formulations, with the ER used more commonly for chronic pain. Adverse effects include dizziness, vertigo, nausea, constipation, and headache (Berger & O’Neill, 2022).
Buprenorphine (Suboxone) is a semi-synthetic partial agonist used in MAT to treat OUD. It has unique pharmacological properties that help reduce the potential for misuse and diminish the effects of physical dependency on opioids, including withdrawal symptoms and cravings. Similar to opioids, it can lead to euphoria and respiratory depression when administered at low-to-moderate doses; however, these effects are weaker than with full opioid agonists. Therefore, buprenorphine (Suboxone) increases patient safety during overdose. It was first approved for use by the FDA in 2002, in combination with counseling and behavioral therapies to treat OUD. According to SAMHSA (2023), there are several types of FDA-approved buprenorphine (Suboxone) products, including buprenorphine/naloxone (Bunavail) buccal film, buprenorphine/naloxone (Zubsolv) sublingual tablets, and buprenorphine extended-release injection (Sublocade). Common side effects of buprenorphine (Suboxone) include nausea, vomiting, constipation, muscle cramps, inability to sleep, cravings, distress, irritability, and fever. Clinicians who prescribe these medications must undergo specialized training and certification due to the strict guidelines for dosing, administration, and monitoring to enhance patient safety. For more information, please refer to the following government-run and regulated website: https://www.SAMHSA.gov (SAMHSA, 2023).
Mixed Agonist-Antagonists
An agonist-antagonist is an opioid that has mixed actions. These drugs produce different activities at various receptors, acting on one opioid receptor to create a response and binding to another receptor to prevent a response. Medications in this class demonstrate varying activity depending on the target receptor and the drug dose. Common agonist-antagonists include pentazocine/naloxone (Talwin) and butorphanol (Stadol). Pentazocine/naloxone (Talwin) is a combination agent for moderate to severe pain. It acts by binding to and activating specific opioid receptors while simultaneously blocking the activity of other opioid receptors. The naloxone (Narcan) component of the medication helps to prevent misuse. Butorphanol (Stadol) is a mixed opioid agonist-antagonist available as a spray for treating migraine headaches. Similar to partial agonists, agonist-antagonist opioids have a ceiling effect. As a result, increased dosages offer lower analgesic efficacy and a higher risk for psychotomimetic or psychotogenic effects (e.g., hallucinations and delirium; Berger & O’Neill, 2022).
Opioid Antagonists
Opioid antagonists compete with opioids at receptor sites to reverse the acute adverse effects, primarily respiratory depression, caused by opioids or to treat OUD. The two most common opioid receptor antagonists are naloxone (Narcan) and naltrexone (Vivitrol). Naloxone (Narcan) is the most widely used opioid antagonist, as it is FDA-approved for acute opioid overdose. Naloxone (Narcan) is highly effective in reversing opioid overdose and respiratory depression. It is dispensed in various formulations (e.g., intravenous, intramuscular, subcutaneous, and intranasal). When administered intravenously, effects begin almost instantly and last for about an hour. The dose can be titrated to reverse respiratory depression without fully reversing the analgesic effects. Rapid medication infusion should be avoided to reduce the risk of hypertension, tachycardia, nausea, and vomiting. Vital signs should be monitored, especially respirations, and naloxone (Narcan) administration should be repeated until the manifestations of opioid toxicity have subsided. With intramuscular, subcutaneous, and intranasal administration, the drug takes effect in two to five minutes and lasts several hours. These administration routes are most commonly used by emergency medical services (EMS) personnel and civilians responding to opioid overdose in the community (CDC, 2023b; Theriot et al., 2023).
According to the CDC (2023b), approximately 50,000 people died from an opioid-involved overdose in 2019. Studies have demonstrated that bystanders were present in at least 1 in 3 overdoses involving opioids. Thus, the opioid epidemic has led to the widespread use of naloxone (Narcan) among EMS personnel and persons in the community. Bystanders can act to prevent overdose deaths as naloxone (Narcan) is now available in all 50 states (CDC, 2023b). The prescribing and dispensing of naloxone (Narcan) has become a central part of the public health response to the opioid overdose epidemic. Most states allow naloxone (Narcan) to be purchased from a pharmacy without a prescription. There are two types of naloxone (Narcan) that anyone can use without medical training: nasal spray (Narcan) and injectable (Zimhi). The nasal spray is a prefilled device that sprays 4 mg of the medication into one nostril once or 1 mg in each (see Figure 6). This may be repeated every 2-4 minutes until the patient becomes responsive. The injectable formulation is injected into the muscle or under the skin (see Figure 7). Pre-filled syringes with 5 mg per 0.5 mL or 1 mg/mL may be repeated every 2-3 minutes as above. Intranasal administration has chief advantages over injectable formulations when responding to overdose patients in the community. The safety profile of intranasal formulations appears to be equivalent to injectable formulations for treating opioid overdose (CDC, 2023b).
Figure 6
Naloxone (Narcan) Nasal Spray

Figure 7
Pre-filled Syringe of Naloxone (Zimhi) Injectable

Patients at the highest risk of narcotic overdose include those who meet any of the following criteria:
- doses of >90 morphine milligram equivalents (MME) per day
- chronic opioid use
- concurrent use of benzodiazepines
- personal history of SUD/OUD
- current treatment for substance abuse/opioid misuse disorders
- family history of SUD
- patients who live in isolated or rural areas
- patients with chronic respiratory, renal, hepatic, or cardiac disease or HIV/AIDS
- current or history of depression or other severe mental health conditions (Dowell et al., 2022; Webster, 2017)
Serious adverse effects of naloxone (Narcan) are rare, and usually, the benefit of using it for an overdose outweighs the risk for adverse effects. However, it can induce acute opioid withdrawal symptoms such as tachycardia, agitation, vomiting, body aches, and convulsions. Naloxone has no reversal effect on tramadol (Ultram), alcohol, or other CNS depressants such as benzodiazepines (CDC, 2023b).
Naltrexone (Vivitrol) is FDA-approved to treat opioid dependence and alcohol use disorder. Naltrexone (Vivitrol) binds to and blocks opioid receptors to suppress opioid cravings. It is not used to treat acute opioid overdose. Patients must detox from opioids before starting naltrexone (Vivitrol); they must be opioid-free for at least 7 to 10 days to prevent opioid withdrawal syndrome. When used for OUD, its purpose is to prevent euphoria and the desire to use opioids. Naltrexone (Vivitrol) is also used to reverse postoperative respiratory depression due to opioid use during the operative period (Vivitrol; Singh & Saadabadi, 2022; Theriot et al., 2023).
Opioid Routes of Administration
Opioids can be via oral, intravenous, intramuscular, transdermal, and subcutaneous routes. They are supplied in short-acting and long-acting preparations. Regardless of the route of administration, education regarding the adverse effects, risks, and benefits is vital in understanding clinical indications and patient outcomes. The oral administration of analgesics is generally preferred for patients whenever possible due to ease of administration, cost-efficacy, and monitoring. However, the duration of action for most short-acting oral opioids is only about 4 hours. ER formulations usually provide pain control for 8 to 12 hours or more. Intranasal analgesic administration is advantageous because the medication is rapidly absorbed. Topical analgesics are applied directly to the skin and are absorbed by vascular uptake. This route may reduce pain during a painful procedure, such as a lumbar puncture. Due to its rapid onset, lidocaine (Lidocaine viscous) is commonly used for dental procedures or other superficially invasive procedures such as skin biopsies. The transdermal analgesic route may also be used to treat chronic pain. Long-acting medication absorbed through the skin can control pain for several hours to days. Transdermal fentanyl (Duragesic) is indicated for patients who have severe pain and are opioid-tolerant (Berger & O’Neill, 2022).
The transmucosal analgesic route is frequently used for hospice patients experiencing breakthrough pain. The oral mucosa is highly vascular, providing rapid absorption. The rectal route for administering analgesics can also be used when immediate pain control is desired; the mucous membranes of the rectum are highly vascular, causing quick absorption of the medication. This route is helpful for unconscious patients, those who have difficulty swallowing, or are experiencing nausea and vomiting. When epidural analgesia is used, an anesthesiologist or nurse anesthetist inserts a catheter into the epidural space along the spine. An analgesic such as morphine (Roxanol, MS Contin) or fentanyl (Duragesic) is infused through the catheter. The patient should be monitored closely for respiratory depression, excessive sedation, hypotension, bradycardia, and urinary retention. The use of other opioids or CNS depressants should be avoided during the use of epidural analgesia. The healthcare team should closely monitor the patient and be prepared to administer naloxone (Narcan) for symptoms of respiratory depression or excessive sedation (Berger & O’Neill, 2022).
Patient-Controlled Analgesia (PCA)
PCA is a medication delivery system that allows patients to self-administer safe doses of opioids and is almost exclusively used in acute inpatient hospital and inpatient hospice settings. Some of the fundamental principles regarding the use of a PCA are represented in the bullet points below.
- A PCA provides small, frequent dosing to ensure consistent plasma levels.
- Patients have less lag time between an identified need and the delivery of medication, which increases their sense of control and can decrease the amount of medication needed.
- Morphine (Roxanol, MS Contin), hydromorphone (Dilaudid), and fentanyl (Duragesic) are typical opioids for PCA delivery.
- Patients should be encouraged to inform their healthcare team if the PCA pump does not adequately control the pain.
- It is widely recommended that caregivers and family members are educated on the potential for inadvertent overdosing when the PCA button is pressed by anyone other than the patient, also called PCA by proxy.
- Clear institutional criteria regarding which patients should receive PCA and careful patient assessment throughout PCA use are essential to ensure safety (Berger & O’Neill, 2022).
Opioid Assessment
There are several tools available for assessing opioid risk. To balance pain management and safety when prescribing opioids, evidence-based guidelines recommend that clinicians who prescribe opioids use risk assessment instruments in patients before starting opioid therapy. The most common tools used include:
- Opioid Risk Tool (ORT)
- Screener and Opioid Assessment for Patients with Pain-Revised (SOAPP-R)
- Screening Instrument for Substance Abuse Potential (SISAP)
- Diagnosis, Intractability, Risk, and Efficacy Score (DIRE; Cheattle, 2019).
The ORT, SOAPP-R, and SISAP are self-administered tools that the patient can complete. The ORT and SISAP are five-item questionnaires used to predict the risk for opioid misuse. The SOAPP-R is a 24-item instrument constructed to predict the development of problematic drug-related behaviors (PDRB). The DIRE is a clinician-administered instrument that predicts the efficacy of analgesia and adherence to long-term opioid therapy (Cheattle, 2019).
Opioid Use in Special Populations
Special considerations should be applied when administering opioids to populations at potentially higher risk for harm, such as older adults (over 65 years), those with renal or hepatic insufficiency, and those who are pregnant. Advancing age is often accompanied by physiological changes that affect medication absorption, metabolism, and excretion. Older adults are also at increased risk for falls and fractures related to opioids. When administering opioids to older adults, an appropriate bowel regimen should be initiated to prevent constipation (Dowell et al., 2022). According to the BC, opioids should be avoided in older adults with a history of falls or fractures (AGS, 2019).
While opioid use in pregnancy is not well studied, it has known risks to the mother and the fetus (Dowell et al., 2022). In 2014, the FDA removed the older system of ranking medications for pregnant women (Category A, B, C, D, and X), and now requires detailed specific information about pregnancy safety (including during labor and delivery), safety while breastfeeding, and safety for females and males of reproductive potential (FDA, 2021). Some studies have shown an association between opioid use during pregnancy and congenital disabilities, including neural tube defects, congenital heart defects, preterm delivery, poor fetal growth, stillbirth, and potential for neonatal opioid withdrawal syndrome (Dowell et al., 2022). Opioids are excreted in breast milk and increase the risk for CNS and respiratory depression in the infant if taken by the mother while breastfeeding. These risks can be minimized using the lowest effective dose to control pain. Acetaminophen (Tylenol) is generally considered safe during pregnancy and while breastfeeding. The FDA (2020b) issued a safety communication advising women to avoid using NSAIDs in pregnancy at 20 weeks or later due to the risk of bleeding, premature ductal closure, and rare but serious kidney problems in the unborn baby. There is limited data on the safe use of NSAIDs while breastfeeding, and the FDA advises breastfeeding women to consult with their healthcare professionals before taking these medications (FDA, 2020b).
Cancer Patients and Pain Management at the End-of-Life
The treatment of cancer pain is highly complex, and the patient's disease prognosis, concurrent medications, and individual goals of care should be carefully considered for all decision-making (Dydyk et al., 2023; Paul et al., 2021). Pain treatment within the specialty care of terminally ill patients does not typically conform to the aforementioned standard regulations. There is less concern for misuse, abuse, or addiction, and emphasis should be on ensuring effective pain relief (Dowell et al., 2022). However, fears continue to focus on overdose, respiratory depression, and potential loss of consciousness or hastening of end-of-life. According to the National Coalition for Hospice and Palliative Care (NCHPC) Clinical Practice Guidelines for Quality Palliative Care, analgesics should be increased gradually and as tolerated, with the patient's full consent or their healthcare proxy (or via their living will or advance directives). The patient and/or caregivers should be fully informed of the potential risks of increased opioid doses. If the patient and family prioritize pain relief over the length of life, the care team should accept and respect that decision. It is generally accepted that clinicians should never withhold needed pain medication from terminally ill patients for fear of hastening death if they have received informed consent from the patient to do so. Loss of consciousness should not always be assumed to be directly caused by high doses of opioid painkillers in the dying patient if those doses have been stable or slowly increasing, especially in chronic cancer pain (NCHPC, 2018).
Complications of Opioid Use
There are several adverse effects associated with opioid use, which vary in severity based on the dose and potency of the medication, administration route, and if the drug is self-administered or administered by a nurse or other caregiver. The most common side effects of opioids include orthostatic hypotension, urinary retention, nausea, and constipation. Patients should be advised to sit or lie down if experiencing orthostatic hypotension (e.g., lightheadedness or dizziness) and avoid sudden changes in positioning (e.g., moving slowly from lying to sitting or standing). To manage urinary retention, monitor intake/output, assess for bladder distention, administer bethanechol (Urecholine), and exhaust all noninvasive actions before catheterizing. Nausea and vomiting can be managed with antiemetic medications, oral hydration, dietary modifications, and elimination of offending odors. A preventative approach to constipation should be implemented with each patient receiving opioids. Strategies include monitoring bowel movements, increasing fluids, adding dietary fiber, increasing hydration, and engaging in daily exercise. In addition, patients should be given stool softeners, stimulant laxatives, and/or enemas as clinically indicated (Berger & O’Neill, 2022; SAMHSA, 2018; Theriot et al., 2023).
The most severe complication of opioid use is overdose which can be fatal if left untreated. A focused assessment, including respiratory rate, depth, and regularity, should be performed before and following opioid administration. In the Opioid Overdose Prevention Toolkit, SAMHSA (2018) recommends the following five primary strategies to prevent overdose deaths:
- Strategy 1: Encourage providers, persons at high risk, family members, caregivers, and others to learn how to prevent and manage opioid overdose.
- Strategy 2: Ensure access to treatment for individuals who are misusing opioids or who have a substance abuse disorder.
- Strategy 3: Ensure ready access to naloxone (Narcan).
- Strategy 4: Encourage the public to call 911.
- Strategy 5: Encourage prescribers to use state prescription drug monitoring programs (PDMPs).
Signs and symptoms of opioid toxicity and overdose include respiratory depression, coma, and pinpoint pupils (also referred to as the opioid triad). Sedation always precedes respiratory depression, so the patient's level of consciousness should be monitored closely so steps can be promptly taken to reduce the dose or administer a reversal agent if required. The initial treatment of respiratory depression and sedation is generally a reduction in the opioid dose, carefully titrating the dose while closely monitoring the patient’s respiratory status. When an overdose is suspected, naloxone (Narcan) should be administered to reverse the opioid effects until the patient can deep breathe with a respiratory rate of at least 8/minute. Most patients respond to naloxone (Narcan) by returning to spontaneous breathing within 2 to 3 minutes of administration. However, some patients may require ventilatory support, rescue breathing, and chest compressions while awaiting the return to spontaneous breathing. All patients should be monitored for at least 4 hours after the last dose of naloxone (Narcan) for signs of recurrence of opioid toxicity. Patients who overdose on long-acting opioids may require prolonged monitoring. Finally, opioid withdrawal triggered by naloxone (Narcan) causes several distressing symptoms in patients physically dependent on these agents. The most common signs and symptoms include agitation, irritability, tachycardia, fever, nausea, vomiting, diarrhea, rhinitis, diaphoresis, nervousness, restlessness, weakness, insomnia, and increased blood pressure (Berger & O’Neill, 2022; SAMHSA, 2018; Theriot et al., 2023).
Opioid Abuse and Misuse
Drug overdose is a leading cause of accidental death in the US, with opioids being the most common drug. Increased prescription of opioid medications in the 1990s led to the widespread misuse of prescription and non-prescription opioids, igniting the nationwide public health emergency known as the Opioid Epidemic (Schiller et al., 2022). According to the CDC (2022a), more than 932,000 people died from an opioid overdose since 1999. Data from the 2021 National Survey on Drug Use and Health revealed that among people aged 12 and older, 9.2 million misused opioids in the past year, and 5.6 million had an OUD. The survey also found that the percentage of adults aged 26 or older (2.2% or 4.9 million people) with an OUD was higher than the percentages of adolescents aged 12 to 17 (1.0% or 259,000 people) or young adults aged 18 to 25 (1.3% or 438,000 people). The most commonly abused medications were hydrocodone (46.9%), oxycodone (30.4%), and codeine (26.4%). Nearly 65% of users reported misuse as a means to ‘relieve physical pain,’ 10.7% to 'feel good' or 'get high,” and 7.3% to ‘relax or relieve tension.’ Nearly 45% of respondents got their medication from a relative or friend (e.g., given by, bought from, or taken from), and 43.2% obtained it by prescription from a healthcare provider. Approximately 1.8 million people aged 12 and older misused prescription pain relievers for the first time in 2021, and nearly 80% were older than 25 years (SAMHSA, 2021). More than 136 Americans die each day from opioid overdose, and these numbers continue to rise (National Center for Drug Abuse Statistics [NCDAS], 2023).
Contributing and Risk Factors for Potential Misuse/Abuse
The progressive rise in prescription drug misuse/abuse across the US is a byproduct of the complex interplay of many contributing factors. However, the CDC (2022a) cites the increased prescribing of opioid analgesics as the most preeminent contributing factor for the significant increase in drug availability and, in turn, misuse/abuse potential. According to the HHS (2019b), additional societal and environmental factors include aggressive marketing by the pharmaceutical industry, the explosion of illegal web-based pharmacies that disseminate these medications without proper prescriptions and surveillance, and greater social acceptability for medicating a growing number of conditions. Personal risk factors for potential drug misuse/abuse include untreated psychiatric disorders, younger age, past or current SUD (including alcohol and tobacco use), family history of SUD, and family or societal environments that encourage these behaviors (Webster, 2017). While prescription drug abuse can happen at any age, data reveals it can begin in teens as young as 12. Opioid mortality is higher in middle-aged people with comorbid substance abuse and psychiatric conditions (SAMHSA, 2021). Prescription drug abuse in older adults is a growing problem, especially when combined with alcohol. Having multiple health problems and taking multiple drugs can put the older adult population at risk of drug misuse or addiction. Also, a lack of knowledge about prescription drugs and their potential harm heightens the risk within this population (NIDA, 2020b).
Opioid Use Disorder (OUD)
OUD is defined in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition Text Revision (DSM-5-TR) as a destructive repetition or habit of ingesting or administering opioids that causes the following substantial anguish or drastically affects the patient’s ability to function professionally, socially, or otherwise, as evidenced by two or more of the conditions listed here within one year:
- ineffective attempts to reduce the use of opioids or a wish to do so
- an intense need or impulse to ingest or administer opioids
- persistent ingestion of opioids even though they have experienced repeated relational challenges (i.e., with surrounding friends and family members) related to its use
- persistent ingestion of opioids in environments where it is unsafe
- the development of tolerance, which is a gradual reduction in the physical impact/effect of the opioids when administered at a consistent amount, requiring an increase in the amount to achieve the prior effect
- persistent ingestion of opioids for a longer time and at a higher amount than planned
- a considerable investment of time related to opioids, procuring them, ingesting them, or recuperating from the consequences of their use.
- persistent ingestion of opioids, leading to interference with significant responsibilities and commitments (i.e., academic, professional, or familial)
- a decrease in attendance or participation in significant events at work, at home, or with friends/family due to the use of opioids
- persistent ingestion of opioids even though they are aware of a significant challenge directly related to opioid use
- the development of withdrawal as evidenced by the signs and symptoms of opioid withdrawal syndrome or the use of opioids to prevent these symptoms.
This diagnosis may be graded as mild (two or three symptoms), moderate (four or five), or severe (at least six symptoms). The diagnosis may be considered in early (3 or more months) or sustained (12 or more months) remission when all of the above symptoms have resolved, except for an intense need or impulse to use the substance. This diagnosis may also be qualified in a controlled environment if the patient lacks substance access.
This diagnosis may also be qualified as on maintenance therapy if the patient is currently on a prescribed opioid agonist (e.g., buprenorphine or methadone; American Psychiatric Association [APA], 2022, p. 608-9).
The Safe and Effective Administration of Opioids
Opioids and all other types of controlled substances are classified according to categories or "schedules" based on the perceived risk of addiction as outlined by the Drug Enforcement Administration (DEA). State laws, regulations, and policies further delineate prescriber responsibilities surrounding prescribing and dispensing controlled substances. In 2017, the HHS increased grant funding toward developing novel strategies to impede this growing and deadly problem. These efforts have brought a higher level of urgency to the matter, with heightened surveillance, restriction, and monitoring of patients on long-term opioid therapy (Schiller et al., 2022).
As part of the national movement to mitigate the opioid epidemic, all 50 states and the District of Columbia have implemented statewide electronic databases PDMPs to track and monitor opioid prescriptions (American Association of Nurse Practitioners [AANP], 2022). A PDMP is a statewide electronic database that collects data on controlled substances dispensed to or for each patient. The intent is to improve opioid prescribing, inform clinical practice, and protect high-risk patients. The key to the efficacy of PDMP systems is the mandate that all prescribers or an appropriate delegate (e.g., nurse) check the system before initiating opioid therapy. Reviewing the patient's history of controlled substance prescriptions using the PDMP database helps to determine whether the patient is already receiving opioids or potentially dangerous combinations that place them at risk for overdose. Differences exist between the states regarding how frequently providers should monitor this system and which controlled substances are included. Reporting systems help reduce the diversion of illegitimate opiate prescriptions (AANP, 2022; CDC, 2021b).
In addition to using PDMPs and monitoring instruments, other risk mitigation strategies include having patients return for more frequent monitoring intervals and performing random pill counts. Some states require healthcare providers to monitor for signs of abuse, misuse, or diversion by performing unannounced urine drug testing (UDT) at least twice yearly. The CDC (Dowell et al., 2022) recommends that UDTs are performed before starting opioid therapy and at least once annually to assess for prescribed medications and other controlled prescription drugs and illicit drugs.
Patient-Provider Agreements and Opioid Contracts
Some states have laws mandating patient-provider agreements (PPA) or opioid contracts. PPAs are written agreements between prescribers and patients outlining and clarifying the conditions for prescribing opioids over the long term, and they can help formalize safer approaches to opioid prescribing. The contract underscores the critical importance of properly taking pain medications, outlining the standards of care and treatment expectations (CDC, 2021b). It promotes collaboration and mutual commitment from both parties, sets realistic expectations with measurable goals for therapy, and also states reasons for which the agreement may be terminated. In addition, these contracts should address the potential adverse effects, possible overdose, respiratory depression, development of physical dependence or tolerance, drug interactions, inadvertent ingestion by children or others, and drug misuse or abuse by the patient, as well as household contacts or friends. Furthermore, prescribing policies should be clearly defined, including the number and frequency of refills, policy on early refills, and procedures for lost, damaged, or stolen medications. If UDTs or pill counts are to be performed periodically, this should be included in the agreement, as well as how medication refills and changes should be requested and obtained by the patient and handled by the office staff and providers (CDC, 2021b).
Documentation
Documentation is critical when administering and monitoring patients taking controlled substances, both for safety and legal reasons. Documentation in the medical record should be clear, concise, and include all details outlining dose adjustments or medication changes with associated justifications and equivalency calculations. Documentation should also include the effectiveness of treatments based on consistent pain and other assessments repeated at each visit and any adverse effects and related therapies. Documentation should also specify if the patient is adhering to treatment plans as outlined in the PPA and include the results of UDTs or pill counts. Any concerning or aberrant behavior should be carefully documented with as much detail as possible. Interviews with family members and caregivers can also be included in documentation records for those same reasons, with a clear plan for resolution and/or future monitoring (PAMI, 2020). Any letters sent to patients should be included in the patient's medical record, and office staff should carefully document any phone calls made or received. Document every time PDMP reports are reviewed and any concerning findings. A decision to terminate care needs to be documented thoroughly (Dydyk et al., 2023; Paul et al., 2021).
Termination of Chronic Opioid Therapy
Treating any medical condition aims to restore health and resume pre-illness ADLs; the same is true for terminating chronic opioid therapy. Termination is an intentional process that occurs when a patient has achieved most of the treatment goals and/or when therapy must end for other reasons. According to the FSMB (2017), continuation, modification, or termination of opioid therapy for pain is contingent on "the clinician's evaluation of (1) evidence of the patient's progress toward treatment objectives and (2) the absence of substantial risks or adverse events, such as signs of SUD and/or diversion" (FSMB, 2017, p.11).
The most common reasons for termination of long-term opioid therapy include the achievement of goals of therapy, treatment policy nonadherence, follow-up nonadherence, or concern for misuse/abuse or diversion. Other reasons include resolution of the underlying condition, intolerable adverse effects, inadequate analgesic effects, or a lack of improvement in the patient’s quality of life. Appropriate termination helps to avoid a perceived betrayal of trust or abuse of power, prevents harm, and conveys caring. The PPA plays a critical role in this process, and therefore termination must be addressed comprehensively in the initial contractual agreement and updated accordingly. Termination always carries the risk of exposing the patient to severe pain and sending the wrong message. A carefully structured taper should be given to anyone who is potentially physically dependent on their opioid to avoid withdrawal symptoms. Otherwise, a referral to an addiction specialist may be required for those on very high doses of opioids. Healthcare providers should reassure patients that this change does not indicate the end of their treatment, which can proceed with other modalities or through another provider if necessary (FSMB, 2017; Hooten, 2020).
Strategies for termination of chronic opioid therapy include the following:
- Establish open, honest communication and dialogue with the patient from the point of the initial consultation.
- Comprehensively address termination in the informed consent and PPA process and readdress or refer to it as necessary during therapy.
- Set realistic, time-sensitive goals at the beginning of treatment.
- Balance clinical judgment and individualization; incidents or events that cause concern regarding a pain agreement need to be interpreted within the context of the whole patient.
- Opioid tapers should be performed after a discussion with the patient. There is no “one way” to taper a patient. Generally, the longer the patient has been on opioids, the longer it will take for a successful taper.
- Avoid terminating the relationship when a patient is in crisis without referral to a specialized facility and a warm handoff to the receiving provider. If a patient is terminated while in crisis, it might be considered abandonment and escalate abhorrent behaviors.
- As part of the termination preparation process, the patient should be given information about other available resources (e.g., community resources, support groups, and nonpharmacological pain modalities). The healthcare provider should document the resources provided (Hooten, 2020).
Withdrawal symptoms can be managed with a2-adrenergic agonists such as clonidine (Catapres) or tizanidine (Zanaflex). An alternative is to transition the patient to a partial agonist, such as buprenorphine (Suboxone), or a different opioid agonist, such as methadone (Dolophine), and then taper at the above-referenced rate to avoid withdrawal symptoms. However, as previously mentioned, both buprenorphine (Suboxone) and methadone (Dolophine) require specialized training and/or certification to prescribe (Davis et al., 2019; HHS, 2019a).
References
Abril, L., Zamora, C., Cordero, M., Williams, A. R., & Friedman, B. W. (2022). The relative efficacy of seven skeletal muscle relaxants: An analysis of data from randomized studies. Journal of Emergency Med, 62(4), 455-461. https://doi.org/10.1016/j.jemermed.2021.09.025
Agrawal, S., & Khazaeni, B. (2023). Acetaminophen toxicity. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK441917/
American Association of Clinical Endocrinologists and American College of Endocrinology (2020). Clinical practice guidelines for the diagnosis and treatment of postmenopausal osteoporosis – 2020 update. Endocrine Practice, 26(Suppl 1), 1-46. https://doi.org/10.4158/GL-2020-0524SUPPL
American Association of Nurse Practitioners. (2022). Issues at a glance: Prescription drug
monitoring programs (PDMPs). https://www.aanp.org/advocacy/advocacy-resource/policy-briefs/issues-at-a-glance-prescription-drug-monitoring-programs-pdmp
American Geriatrics Society. (2019). American Geriatrics Society 2019 updated Beers
Criteria® for potentially inappropriate medication use in older adults. Journal of American Geriatric Society, 67(4), 674-694. https://doi.org/10.1111/jgs.15767
American Medical Association. (2021). AMA backs update to CDC opioid prescribing guidelines. https://www.ama-assn.org/press-center/press-releases/ama-backs-update-cdc-opioid-prescribing-guidelines
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders: Text revision, DSM-5-TR (5th ed.). American Psychiatric Publishing.
Amputee Coalition. (n.d.). Managing phantom pain. Retrieved April 24, 2023, from https://www.amputee-coalition.org/limb-loss-resource-center/resources-for-pain-management/managing-phantom-pain/
Bendtsen, L., Zakrzewska, J. M., Braschinsky, A. M., Donnet, D. A., Eide, P. K., Leal, P. R. L., Maarbjerg, S., May, T., Nurmikko, T., Obermann, M., Jensen, T. S., & Cruccu, G. (2019). European Academy of Neurology guideline on trigeminal neuralgia. European Journal of Neurology, 26(6), 831-849. https://doi.org/10.1111/ene.13950
Berger, A. M., & O’Neill (2022). Principles and practices of palliative care and supportive oncology (5th ed.). Wolters Kluwer
Bickley, L. S., Szilagyi, P. G., Hoffman, R. M., & Soriano, R. P. (2020). Bates’ guide to physical examination and history taking (13th ed.). Wolters Kluwer
Burns, M. J., Friedman, S. L., & Larson, A. M. (2023). Acetaminophen (paracetamol) poisoning in adults: Pathophysiology, presentation, and diagnosis. UpToDate. Retrieved April 22, 2023, from https://www.uptodate.com/contents/acetaminophen-paracetamol-poisoning-in-adults-pathophysiology-presentation-and-evaluation
Castelli, G., Desai, K. M., & Cantone, R. E. (2020). Peripheral neuropathy: Evaluation and differential diagnosis. American Family Physician, 1-2(12), 732-739. https://www.aafp.org/pubs/afp/issues/2020/1215/p732.html
Craske, M. G., (2017). Cognitive-behavioral therapy (2nd ed.). American Psychiatric Association.
The Centers for Disease Control and Prevention. (2019). About shingles (herpes zoster). https://www.cdc.gov/shingles/about/index.html
The Centers for Disease Control and Prevention. (2020a). Fibromyalgia. https://www.cdc.gov/arthritis/basics/fibromyalgia.htm
The Centers for Disease Control and Prevention. (2020b). Prevent opioid misuse. https://www.cdc.gov/opioids/patients/prevent-misuse.html
The Centers for Disease Control and Prevention. (2021a). Opioid basics: Commonly used terms. https://www.cdc.gov/opioids/basics/terms.html
The Centers for Disease Control and Prevention. (2021b). Prescription drug monitoring programs (PDMPs). https://www.cdc.gov/drugoverdose/pdmp/index.html
The Centers for Disease Control and Prevention. (2022a). Death rate maps & graphs. https://www.cdc.gov/drugoverdose/deaths/index.html
The Centers for Disease Control and Prevention. (2022b). Shingles (Herpes Zoster). https://www.cdc.gov/shingles/vaccination.html
The Centers for Disease Control and Prevention. (2023a). Guideline recommendations and guiding principles: 2022 clinical practice guideline recommendation. https://www.cdc.gov/opioids/healthcare-professionals/prescribing/guideline/recommendations-principles.html
The Centers for Disease Control and Prevention. (2023b). Lifesaving naloxone. https://www.cdc.gov/stopoverdose/naloxone/index.html
Cheattle, M. (2019). Risk assessment: Safe, opioid prescribing tools. https://www.practicalpainmanagement.com/resource-centers/opioid-prescribing-monitoring/risk-assessment-safe-opioid-prescribing-tools
Chou, R. (2023). Subacute and chronic low back pain: Nonpharmacologic and pharmacologic treatment. UpToDate. Retrieved April 25, 2023, from https://www.uptodate.com/contents/subacute-and-chronic-low-back-pain-nonpharmacologic-and-pharmacologic-treatment#!
Davis, M. P., Digwood, G., Mehta, Z., & McPherson, M. L. (2019). Tapering opioids: A comprehensive qualitative review. Annals of Palliative Medicine, 9(2), 586-610. http://dx.doi.org/10.21037/apm.2019.12.10
Derry, S., Rice, A. S. C., Cole, P., Tan, T., & Moore, R. A. (2017). Topical capsaicin (high concentration) for chronic neuropathic pain in adults (review). Cochrane Database of Systematic Reviews, 1, 1-67. https://doi.org/10.1002/14651858.CD007393.pub4
Desborough, M. J., & Keeling, D. M. (2017). The aspirin story – from willow to wonder drug. British Journal of Haematology, 177, 674-683. https://doi.org/10.1111/bjh.14520
Dowell, D., Ragan, K. R., Jones, C. M., Baldwin, G. T., & Chou, R. (2022). CDC clinical practice guideline for prescribing opioids for pain – United States, 2022. Morbidity and Mortality Weekly Report (MMWR), 71(No. RR-3), 1-95. http://dx.doi.org/10.15585/mmwr.rr7103a1
Dydyk, A. M., Sizemore, D. C., Haddad, L. M., Lindsay, L., & Porter, B. R. (2023). NP safe prescribing of controlled substances while avoiding drug diversion. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK564518/
Endo Pharmaceuticals. (2018). Lidoderm® (lidocaine patch 5%). https://www.accessdata.fda.gov/drugsatfda_docs/label/2018/020612s014lbl.pdf
Federation of State Medical Boards. (2017). Guidelines for the chronic use of opioid analgesics. https://www.fsmb.org/siteassets/advocacy/policies/opioid_guidelines_as_adopted_april-2017_final.pdf
Ghlichloo, I., & Gerriets, V. (2022). Nonsteroidal anti-inflammatory drugs (NSAIDs). StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK547742/
Heard, K., & Dart, R. (2022). Acetaminophen (Paracetamol) poisoning in adults: Treatment. UpToDate. Retrieved April 23, 2023, from https://www.uptodate.com/contents/acetaminophen-paracetamol-poisoning-in-adults-treatment
Hooten, W. M. (2020). Opioid management: Initiating, monitoring, and tapering. Phys Med Rehabil Clin N Am, 31(2), 265-277. https://doi.org/10.1016/j.pmr.2020.01.006
Hosseini, F., Mullins, S., Gibson, W., & Thake, M. (2022). Acute pain management for older adults. Clinical Medicine Journal, 22(4), 302-306. https://doi.org/10.7861/clinmed.22.4.ac-p
Hudspeth, R. S. (2016). Safe opioid prescribing for adults by nurse practitioners: Part 1. Patient
history and assessment standards and techniques. The Journal for Nurse Practitioners, 12(3), 141-148. https://doi.org/10.1016/j.nurpra.2015.10.012
Ignatavicius, D. D., Workman, L., Rebar, C. R., & Heimgartner, N. M. (2020). Medical-surgical nursing: patient-centered collaborative care. (10th ed.). Elsevier
International Association for the Study of Pain. (2020). Terminology. https://www.iasp-pain.org/resources/terminology/?navItemNumber=576#Pain
Lim, J., Choi, S., Lee, W., Jang, J., Moon, J., Kim, Y., & Kang, D. (2018). Cognitive-behavioral therapy for patients with chronic pain. Medicine (Baltimore), 97(23). e10867. https://doi.org/10.1097/MD.0000000000010867
McCaffery, M. (1968). Nursing practice theories related to cognition, bodily pain, and man-environment interactions. UCLA Students Store.
MrAnnoying. (2016). The biopsychosocial model of health [image]. Wikimedia. https://commons.wikimedia.org/wiki/File:Biopsychosocial_Model_of_Health_1.png
National Center for Drug Abuse Statistics. (2023). Drug overdose death rates. https://drugabusestatistics.org/drug-overdose-deaths/
National Coalition for Hospice and Palliative Care. (2018). Clinical practice guidelines for quality palliative care (4TH ed.). https://www.nationalcoalitionhpc.org/wp-content/uploads/2018/10/NCHPC-NCPGuidelines_4thED_web_FINAL.pdf
National Institute of Diabetes and Digestive Kidney Diseases. (2018). Diabetic neuropathy. https://www.niddk.nih.gov/health-information/diabetes/overview/preventing-problems/nerve-damage-diabetic-neuropathies/all-content
National Institute of Neurological Disorders and Stroke. (2020). Low back pain. https://www.ninds.nih.gov/sites/default/files/migrate-documents/low_back_pain_20-ns-5161_march_2020_508c.pdf
National Institute of Neurological Disorders and Stroke. (2023a). Pain. https://www.ninds.nih.gov/health-information/disorders/pain#3084_2
National Institute of Neurological Disorders and Stroke. (2023b). Trigeminal neuralgia. https://www.ninds.nih.gov/Disorders/All-Disorders/Trigeminal-Neuralgia-Information-Page
National Institute on Drug Abuse. (2020a). Misuse of prescription drugs research report. https://www.drugabuse.gov/publications/misuse-prescription-drugs/overview
National Institute on Drug Abuse. (2020b). Drugs, brains, and behavior: The science of addiction – Drug misuse and abuse. https://www.drugabuse.gov/publications/drugs-brains-behavior-science-addiction/drug-misuse-addiction#footnote
National Institute on Drug Abuse. (2021). Prescription opioids drug facts. https://nida.nih.gov/publications/drugfacts/prescription-opioids
Orandi, B. J., McLeod, M. C., MacLennan, P. A., Lee, W. M., Fontana, R. J., Karvellas, C. J., McGuire, B. M., Lewis, C. E., Terrault, N. M., Locke, J. E., & US Acute Liver Failure Study Group. (2023). JAMA, 329(9), 735-744. https://doi.org/10.1001/jama.2023.1080
Pain Assessment and Management Initiative. (2020). Pain management & dosing guide. https://pami.emergency.med.jax.ufl.edu/wordpress/files/2020/09/PAMI-Dosing-Guide-Nov.2.2020.pdf
Paul, A. K., Smith, C. M., Rahmatullah, M., Nissapatorn, V., Wilairatana, P., Spetea, M., Gueven, N., & Dietis, N. (2021). Opioid analgesia and opioid-induced adverse effects: A review. Pharmaceuticals, 14(11), 1091. https://doi.org/10.3390/ph14111091
Price, R., Smith, D., Franklin, G., Gronseth, G., Pignone, M., David, W. S., Armon, C., Perkins, B. A., Bril, V., Rae-Grant, A., Halperin, J., Licking, N., O’Brien, M., Wessels, S. R., MacGregor, L. C., Fink, K., Harkless, L. B., Colbert, L., Callaghan, B. C. (2021). Oral and topical treatment of painful diabetic polyneuropathy: Practice guideline update summary. Neurology, 98(1). https://doi.org/10.1212/WNL.0000000000013038
Qaseem, A., Wilt, T. J., Mclean, R. M., & Forciea, M. A. (2017). Noninvasive treatments for acute, subacute, and chronic low back pain: A clinical practice guideline from the American College of Physicians. Annals of Internal Medicine,166(7), 514-530. https://doi.org/10.7326/m16-2367
Rabow, M.W., Pantilat, S.Z., Shah, A., Poree, L., & Steiger S. (2020). Principles of pain management. In: M. A. Papadakis, S. J. McPhee, & M. W. Rabow (Eds.). Current medical diagnosis and treatment 2020. McGraw-Hill
Raja, S. N., Carr, D. B., Cohen, M., Finnerup, N. B., Flor, H., Gibson, S., Keefe, F., Mogil, J. S., Ringkamp, M., Sluka, K. A., Song, X., Stevens, B., Sullivan, M., Tutelman, P., Ushida, T., & Vader, K. (2020). The revised IASP definition of pain: Concepts, challenges, and compromises. Pain, 161(9), 1976-1982. https://doi.org/10.1097/j.pain.0000000000001939
Rikard, S. M., Strahan, A. E., & Schmit, K. M. (April 14, 2023). Chronic pain among adults – United States, 2019-2021. Morbidity and Mortality Weekly Report (MMWR), 72(15), 379-385. https://doi.org/10.15585/mmwr.mm7215a1
Runde, T. J., & Nappe, T. M. (2022). Salicylates toxicity. StatPearls [Internet], https://www.ncbi.nlm.nih.gov/books/NBK499879/
Schiller, E. Y., Goyal, A., & Mechanic, O. J. (2022). Opioid overdose. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK470415/
Schwenk, E. S. (2023). Nonopioid pharmacotherapy for acute pain in adults. UpToDate. Retrieved April 26, 2023, from https://www.uptodate.com/contents/nonopioid-pharmacotherapy-for-acute-pain-in-adults
Sheffler, Z. M., Patel, P., & Abdijadid, S. (2023). Antidepressants. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK538182/
Singh, D., & Saadabadi, A. (2022). Naltrexone. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK534811/
Substance Abuse and Mental Health Services Administration. (2018). SAMHSA opioid overdose prevention toolkit. https://store.samhsa.gov/sites/default/files/d7/priv/sma18-4742.pdf
Substance Abuse and Mental Health Services Administration. (2021). Key substance use and mental health indicators in the United States: Results from the 2021 National Survey on Drug Use and Health. https://www.samhsa.gov/data/sites/default/files/reports/rpt39443/2021NSDUHFFRRev010323.pdf
Substance Abuse and Mental Health Services Administration. (2023). Buprenorphine. https://www.samhsa.gov/medication-assisted-treatment/treatment/buprenorphine
Taylor, J. L., Regier, N. G., Li, Q., Liu, M., Szanton, S. L., & Sloasky, R. L. (2022). The impact of low back pain and vigorous activity on mental and physical health outcomes in older adults with arthritis. Frontiers in Pain Research (Lausanne), 3(886985). 1-10. https://doi.org/10.3389/fpain.2022.886985
Theriot, J., Sabir, S., & Azadfard, M. (2023). Opioid antagonists. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK537079/
The University of Florida Health. (n.d.). Pain assessment scales/tools. Retrieved April 22, 2023, from https://pami.emergency.med.jax.ufl.edu/resources/pain-assessment-scales/
US Department of Health and Human Services. (2017). HHS acting secretary declares public health emergency to address national opioid crisis. https://www.hhs.gov/about/news/2017/10/26/hhs-acting-secretary-declares-public-health-emergency-address-national-opioid-crisis.html
US Department of Health and Human Services. (2019a). HHS guide for clinicians on the appropriate dosage reduction or discontinuation of long-term opioid analgesics. https://www.cms.gov/About-CMS/Story-Page/CDCs-Tapering-Guidance.pdf
US Department of Health and Human Services. (2019b). Pain management best practices inter-agency task force report: Updates, gaps, inconsistencies, and recommendations. https://www.hhs.gov/sites/default/files/pmtf-final-report-2019-05-23.pdf
US Food & Drug Administration. (2018a). FDA drug safety communication: Prescription acetaminophen products to be limited to 325 mg per dosage unit; Boxed warning will highlight potential for severe liver failure. https://www.fda.gov/drugs/drug-safety-and-availability/fda-drug-safety-communication-prescription-acetaminophen-products-be-limited-325-mg-dosage-unit
US Food & Drug Administration. (2020a). Nonsteroidal anti-inflammatory drugs (NSAIDs). https://www.fda.gov/drugs/postmarket-drug-safety-information-patients-and-providers/nonsteroidal-anti-inflammatory-drugs-nsaids
US Food & Drug Administration. (2020b). Nonsteroidal anti-inflammatory drugs (NSAIDs): Drug safety communication – Avoid use of NSAIDs in pregnancy at 20 weeks or later. https://www.fda.gov/safety/medical-product-safety-information/nonsteroidal-anti-inflammatory-drugs-nsaids-drug-safety-communication-avoid-use-nsaids-pregnancy-20
US Food & Drug Administration. (2021). Pregnancy and lactation labeling (drugs) final rule. https://www.fda.gov/drugs/labeling-information-drug-products/pregnancy-and-lactation-labeling-drugs-final-rule
US Preventative Services Task Force. (2022). Aspirin use to prevent cardiovascular disease: US Preventative Services Task Force Recommendation Statement. JAMA, 327(16), 1577-1584. https://doi.org/10.1001/jama.2022.4983
Viatris Inc. (2022). Lyrica®: Pregabalin capsules. https://www.lyrica.com/en/fibromyalgia
Wager, T. D. (2022). Managing pain. Cerebrum, v.2022(Mar-Apr 2022). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9224345
Wald, A., & Johnston, C. (2022). Treatment and prevention of herpes simplex virus 1 in immunocompetent adolescents and adults. UpToDate. Retrieved April 23, 2023, from https://www.uptodate.com/contents/treatment-and-prevention-of-herpes-simplex-virus-type-1-in-immunocompetent-adolescents-and-adults
Wang, S., Han, C., Bahk, W., Lee, S., Patkar, A. A., Masand, P. S., & Pae, C. (2018). Addressing the side effects of contemporary antidepressant drugs: A comprehensive review. Chonnam Medical Journal, 54 (2), 101-112. https://doi.org/10.4068/cmj.2018.54.2.101 www.ncbi.nlm.nih.gov/pmc/articles/PMC5972123/
Watson, J. C. (2022a). Overview of pain. Merck Manual Professional Version. Retrieved April 23, 2023, from https://www.merckmanuals.com/professional/neurologic-disorders/pain/overview-of-pain
Watson, J. C. (2022b). Treatment of pain. Merck Manual Professional Version. Retrieved April 26, 2023, from https://www.merckmanuals.com/professional/neurologic-disorders/pain/treatment-of-pain
Webster, L. R. (2017). Risk factors for opioid-use disorder and overdose. Anesthesia Analgesia, 125(5), 1741-1748. https://doi.org/10.1213/ane.0000000000002496
Yam, M. F., Loh, Y. C., Tan, C. S., Adam, S. K., Manan, N. A. & Basir, R. (2018). General pathways of pain sensation and the major neurotransmitters involved in pain regulation. International Journal of Molecular Sciences, 19(8), 2164. https://doi.org/10.3390/ijms19082164