About this course:
This module provides an overview of sepsis, including risk factors, clinical features, and best practices for diagnosis and treatment to inform practice and help advanced practice registered nurses (APRNs) provide optimal care, patient education, and support improved patient outcomes and decreased mortality.
Course preview
Overview of Sepsis for APRNs
This module provides an overview of sepsis, including risk factors, clinical features, and best practices for diagnosis and treatment to inform practice and help advanced practice registered nurses (APRNs) provide optimal care, patient education, and support improved patient outcomes and decreased mortality.
By the completion of this learning activity, learners will be able to:
- Discuss the pathophysiology of sepsis.
- Identify the risk factors associated with sepsis.
- Describe the clinical manifestations of sepsis.
- Examine the diagnosis and treatment strategies for sepsis.
- Discuss the complications related to sepsis or its management.
Sepsis is one of the oldest described medical conditions. The term sepsis is derived from the ancient Greek term for “decomposition” or “decay.” The first documented use was in Homer’s poems around 2,700 years ago. Hippocrates used the term around 400 BCE to describe how meat decays and swamps release decomposing gases. He also used the term to describe how infected wounds become purulent. Still, the hypothesis that the host response, not the pathogen, was responsible for sepsis was not developed until the 1900s. The germ theory of disease was developed in the 1800s, which led to the recognition that sepsis originates from invading microorganisms. The first modern definition was attempted in the early 1900s. The term “blood poisoning” has been used for centuries, and it persists as a description of sepsis in the non-medical population. Understanding the actual cause and pathophysiology of sepsis has led to better diagnosis of and treatment for sepsis. Evidence has shown that the manifestations of sepsis can no longer be attributed solely to the infectious agent and the immune response but also to significant alterations in coagulation, immunosuppression, and organ dysfunction. Therefore, sepsis is defined as a clinical syndrome that has biological, physiological, and biochemical abnormalities caused by a dysregulated response to an infection (Berg & Gerlach, 2018; Gyawali et al., 2019).
Epidemiology
Sepsis is the body’s response to an infection and can lead to life-threatening complications. Given that anyone can get an infection and any infection can lead to sepsis, timely and accurate diagnosis and management of sepsis is critical. According to the World Health Organization (WHO), sepsis acquired in health care settings is one of the most common adverse events during care delivery. It is estimated that there are 48.9 million cases of sepsis annually worldwide. In addition, there are approximately 11 million sepsis-related deaths, accounting for 20% of all worldwide deaths. Almost half of these cases occur in children, with approximately 20 million cases and 2.9 million deaths occurring in those under 5 years old. Regional disparities regarding sepsis also exist globally, with approximately 85% of cases and deaths occurring in low- and middle-income countries (Centers for Disease Control and Prevention [CDC], 2023; WHO, 2023).
Sepsis is the most common cause of admissions to intensive care units (ICUs) and also the most common cause of death in adults admitted to ICUs in the US (Gauer et al., 2020). Although the management of sepsis has improved, the condition’s incidence is increasing as more drug-resistant organisms emerge. This increased incidence can also be attributed to patients being discharged from the hospital faster and possibly before manifestations of sepsis are apparent. According to the CDC, 1 in 3 patients who die in a hospital will die of sepsis (CDC, 2023). Every year, more than 1.7 million Americans develop sepsis, and almost 350,000 of these patients die during their hospitalization or are discharged to hospice. Sepsis is one of the most expensive diagnoses to treat in the US and accounts for more than $38 billion annually (CDC, 2023; Hollenbeak et al., 2023).
Sepsis and septic shock commonly occur in the US, and most cases begin before a patient enters the health care system. One cohort study of US adults who had sepsis and septic shock explored what types of health care exposures occurred during the 30 days before hospitalization (Fay et al., 2020). Most of the patients in the study (90.3%) were found to have community-onset sepsis (diagnoses within 3 days of hospital admission), and 60.7% of those patients had recent encounters with the health care system. The researchers found that 24.1% of patients had an outpatient encounter within 7 days of admission, and 42% of patients had received medical treatment, including antimicrobials, chemotherapy, wound care, dialysis, or surgery in the month before developing sepsis. The researchers concluded that early recognition and standardized treatment upon admission are important; however, exposures as opportunities to prevent sepsis (Fay et al., 2020).
Pathophysiology
Sepsis is a complex process that usually begins with a bacterial, fungal, or viral infection. Most of the time, sepsis results from a gram-positive bacterial infection. However, there has been an increased incidence of sepsis associated with gram-negative bacteria, viruses, and fungal infections, which more commonly occur in immunocompromised patients. Organisms that often cause sepsis include gram-negative (Klebsiella pneumoniae [K. pneumoniae], Pseudomonas aeruginosa [P. aeruginosa], and Escherichia coli [E. coli]) and gram-positive (Staphylococcus aureus [S. aureus] and Streptococcus pyogenes [S. pyogenes]) bacteria. Infections with antimicrobial-resistant organisms confer a higher risk of developing sepsis. Common antimicrobial-resistant organisms include vancomycin-resistant Enterococcus (VRE), carbapenem-resistant Enterobacterales (CRE [K. pneumoniae, E. coli, P. aeruginosa]), methicillin-resistant S. aureus (MRSA), and penicillin-resistant Streptococcus pneumoniae (S. pneumoniae). The incidence of fungal sepsis has increased over the past decade but remains lower than bacterial sepsis. Viruses can also cause sepsis, including influenza A and B, respiratory syncytial virus (RSV), human metapneumovirus, parainfluenza virus types 1 to 3, coronavirus, adenovirus, enterovirus, and rhinovirus. In about half of all sepsis cases, cultures are negative, and a causative organism is not identified (Fay et al., 2020; Hinkle et al., 2021; Neviere, 2023).
Sepsis exists on a continuum of severity, ranging from infection and bacteremia to sepsis and septic shock. A sepsis infection can progress to a critical situation over several days. As the infection advances, the pathological changes occur faster and become more severe. Control and prevention of sepsis are easier to achieve early in the infectious process, as sepsis that is not recognized early with quick intervention contributes significantly to the progression of septic shock, multiple organ dysfunction syndrome (MODS), and death. The risk of mortality can also range from moderate to substantial depending on the pathogen, host factors, and timeliness of recognition and treatment initiation. Although the site of infection is important to determine, as many as 30% of patients who have sepsis will never have an identifiable site of infection (Hinkle et al., 2021; Neviere, 2023).
An infection that is localized rarely leads to sepsis and shock. A healthy immune system and inflammatory response will confine and eliminate the invading organism when the invasion starts, preventing the infection from becoming worse or more widespread. White blood cells (WBCs) around the infection will secrete cytokines that trigger local inflammation, summoning other WBCs to kill invading...
...purchase below to continue the course
Sepsis is the systemic manifestation of infection that occurs when certain organisms have entered the bloodstream. Widespread inflammation is triggered. This response is called systemic inflammatory response syndrome (SIRS). The most recent guidelines for sepsis have removed SIRS from the definition because SIRS can occur in other disease processes. However, systemic inflammation is still part of the underlying pathophysiology of sepsis. The organisms in the bloodstream will enter other body areas, leading to the systemic inflammatory response and extensive hormonal, tissue, and vascular changes. Oxidative stress further impairs tissue perfusion and oxygenation. The circulating WBCs produce cytokines, which result in widespread vasodilation and blood pooling. This leads to early manifestations of mild hypotension, low urine output, and tachypnea, resulting in decreased cardiac output (CO). Body temperature may be elevated, but that varies depending on WBC function and the duration of the sepsis. A patient may have either a low-grade or a high-grade fever. Other patients may have a subnormal body temperature. SIRS is responsible for the fever and hypotension. Impaired oxygenation and tissue perfusion lead to decreased urine output and tachypnea. At this point, the patient usually presents with an elevated WBC count in their laboratory results, as expected, with a systemic infection. The cytokines also release lipoxygenase, leukotrienes, bradykinin, histamine, serotonin, and IL-2. The body opposes these with anti-inflammatory mediators (IL-4, IL-10), which results in a negative feedback mechanism (Forrester, 2023; Hinkle et al., 2021; Ignatavicius et al., 2023).
In addition to SIRS, pro-inflammatory and anti-inflammatory cytokines released during this response activate the coagulation system. Abnormal clotting and microthrombi formation in some organ capillaries cause hypoxia and reduce organ function. At this point, arteries and arterioles will dilate and decrease peripheral arterial resistance, so CO increases. This stage is called warm shock. If sepsis is diagnosed and treated at this point, organ damage is reversible. If undiagnosed and not treated, poor capillary flow and capillary obstruction from the microthrombi decrease oxygen delivery to tissues and impair the removal of carbon dioxide and other waste products. These toxic metabolites damage more cells and increase the production of inflammatory cytokines, leading to worsening SIRS and a damaging cycle of hypoxia and poor perfusion that will progress without intervention. The imbalance between the inflammatory response and the clotting and fibrinolysis cascades are considered critical components of the physiologic progression of sepsis. The early stage of sepsis has a short duration, and the clinical manifestations can be subtle, often leading to a missed or misdiagnosed condition. When identified and treated, the outcomes for SIRS and early sepsis are positive. When sepsis and SIRS are not recognized and treated, they will progress to septic shock (previously severe sepsis) (Forrester, 2023; Hinkle et al., 2021; Ignatavicius et al., 2023). Identifying criteria for detecting SIRS has been established and is shown in Table 1. The use of SIRS criteria to identify sepsis is not recommended since SIRS criteria may be present in many patients who do not develop infection, and the ability to predict death is poor when compared to other scores. SIRS may occur in various non-infectious conditions, including pancreatitis, thromboembolism, burns, surgery, autoimmune disorders, and vasculitis (Neviere, 2023). SIRS may also indicate an adaptive and appropriate host response to infection (Singer et al., 2016).
Table 1
SIRS Criteria
SIRS is clinically recognized by the presence of two or more of the following.
|
(Neviere, 2023)
Septic shock consists of the features described previously plus sepsis-induced organ dysfunction. All tissues are involved and considered hypoxic to some degree. At this point, some organs will be experiencing cell death and organ dysfunction. Microthrombi formation is widespread, and clots continue to form where they are not needed, expending the available platelets and clotting factors and resulting in a condition known as disseminated intravascular coagulation (DIC). The SIRS and cytokine release prompt capillary leakage, cell injury, and increased cell metabolism. Cellular damage reduces the body’s anti-clotting ability and triggers the formation of more clots, increasing DIC. Metabolism increases, which negatively affects the cellular uptake of oxygen. The stress response triggers the release of glucose from the liver, which causes hyperglycemia. The more severe a patient’s response is, the higher their blood glucose level will be. Even though this stage is severe and can last 24 hours or more, it is still often unrecognized. One reason may be the body’s compensatory mechanisms. Blood pooling and capillary leakage stimulate the heart, elevating the heart rate and blood pressure and increasing CO. The patient may have warm extremities, even with decreased tissue perfusion, and there will be little or no cyanosis. At this point, the patient’s WBC count is no longer elevated. Prolonged sepsis has exceeded the bone marrow’s ability to produce mature neutrophils and other WBCs. The patient will exhibit lower oxygen saturation, tachypnea, decreased or absent urine output, and changes in their level of consciousness (LOC) and cognition. Mortality in patients who have reached this stage is high, but aggressive intervention can prevent septic shock (Forrester, 2023; Hinkle et al., 2021; Ignatavicius et al., 2023).
Septic shock consists of MODS with organ failure and poor clotting with uncontrollable bleeding. The death rate among patients who have septic shock is high, as the patient has entered sepsis-induced hypotension that does not respond to fluid resuscitation. Vasodilation and capillary leakage will continue. Cardiac contractility is poor because of cardiac ischemia. Severe hypovolemic shock and decreased cardiac function result from the blood’s inability to clot due to DIC. The clinical manifestations resemble late-stage hypovolemic shock (Forrester, 2023; Hinkle et al., 2021; Ignatavicius et al., 2023).
Risk Factors and Comorbidities
Sepsis starts with an infection—most often pneumonia—that triggers a dysregulated host response. Other infections that commonly lead to sepsis include gastrointestinal (GI) infections, genitourinary (GU) infections, skin and soft tissue infections, and respiratory infections. Patients who are at exceptionally high risk for sepsis are those who have a compromised immune system or a central venous access device. Central lines in place for even a short period will provide a point of entry for microorganisms and may lead to central line-associated bloodstream infections (CLABSIs). Other invasive devices that increase the risk of sepsis include endotracheal tubes, urinary catheters, and drainage tubes. Various other factors or conditions can predispose to sepsis, including malnutrition, large wounds, trauma, burns, GI ischemia, invasive procedures, cancer, increased age (over 65 years old), infections with resistant microorganisms, chemotherapy, alcohol use disorder, diabetes mellitus (DM), obesity, chronic kidney disease (CKD), transplants, hepatitis, and HIV or AIDS. Essentially, patients who have many underlying conditions are at risk for sepsis. Prior treatment with antibiotics or corticosteroids also increases the risk of sepsis (Bokhari, 2023b; Gauer et al., 2020; Ignatavicius et al., 2023; Markwart et al., 2020).
Hospitalization may induce an altered human microbiome, especially when patients are treated with antibiotics. Patients who have a history of hospitalization have a three-fold increased risk of sepsis in the subsequent 90 days, with an even higher risk if the hospitalization was for an infection-related condition, such as Clostridium difficule (C. diff). Patients who are admitted to an ICU are at increased risk of sepsis, with approximately 50% of ICU patients having a nosocomial infection. In addition, patients who are obese and admitted to an ICU have a higher risk of infectious complications, including ventilator-associated pneumonia (VAP) and CLABSIs, and have an increased mortality rate from sepsis than individuals who are normal weight (Neviere, 2023). Postoperative sepsis is a complication of surgery. The patient-related risk factors associated with postoperative sepsis include preexisting conditions (heart failure, DM, CKD). Male patients are also at a higher risk of postoperative sepsis. Surgery-related risk factors for postsurgical sepsis include emergency surgery, inpatient hospital stay, perioperative blood transfusions, and open surgery (Plaeke et al., 2020).
Rehospitalization is common in patients who recover from sepsis. As many as 1 in 5 of these patients are rehospitalized within 30 days of discharge. Risk factors for rehospitalization after sepsis include increasing age, male sex, multiple comorbidities, non-elective admissions, and hospitalizations prior to sepsis admission. Patients who are not discharged home following their sepsis admission also have an increased risk of readmission. Sepsis-specific risk factors include those who have a GI site of infection, infections from extended-spectrum beta-lactamase (ESBL) bacteria, increased severity of sepsis, and prolonged initial hospital length of stay. Other characteristics that elevate a patient’s rehospitalization risk include lower socioeconomic strata, lower hemoglobin on discharge, use of total parenteral nutrition (TPN), and tracheostomy at sepsis admission (Shankar-Hari et al., 2020).
For children who have sepsis, risk factors for increased mortality include younger age (less than 1 year old), complex neurological conditions, infective endocarditis, immunodeficiency, HIV, burns, malignancy, and transplant status. Black and Hispanic children also have higher mortality rates with sepsis. Low-birth-weight neonates are also considered a high-risk population (Markwart et al., 2020; Thavamani et al., 2020). Neonatal sepsis is classified as early or late. Early neonatal sepsis appears within the first 72 hours after birth, and late neonatal sepsis begins after 72 hours. Early neonatal sepsis is acquired before or during childbirth, so the pathogens are usually obtained from the mother’s GU tract. Late neonatal sepsis occurs most often in newborns who require prolonged hospitalization. Risk factors for early neonatal sepsis include maternal Streptococcus agalactiae (S. agalactiae, group-B streptococcus, or GBS) colonization. Mothers who do not undergo prophylactic antibiotic treatment have a 25-fold higher risk of having a newborn who has early neonatal sepsis. Amniotic membrane rupture for over 18 hours and chorioamnionitis are also risk factors for early neonatal sepsis. Prematurity, low birth weight, invasive procedures, histamine-2 antagonists (H2 blockers), and prolonged antibiotic therapy are risk factors for late neonatal sepsis (Procianoy & Silveira, 2020).
Clinical Manifestations
Manifestations of sepsis can be subtle and are often mistaken for clinical manifestations of other disorders, including delirium, pancreatitis, pulmonary embolism, and cardiac dysfunction. The history and physical exam are critical when evaluating a patient for suspected sepsis and should focus on identifying risk factors for increased mortality and identifying the possible source of infection. Gathering information focused on finding the potential source of infection can facilitate focused treatment strategies. APRNs should ask about a recent history of hospitalization or illness. Table 2 outlines the presentation of common sources associated with sepsis, including their manifestations and associated microbiologic evaluation (Bullock & Benham, 2023; Forrester, 2023).
Early manifestations of sepsis may include fever (greater than 100.9 ˚ F [38.3˚ C]), diaphoresis, tachycardia (heart rate [HR] greater than 90 beats/minute or more than two standard deviations above the normal value for the patient’s age), and tachypnea (respiratory rate greater than 20 breaths/minute). During this early phase, blood pressure may be normal. Many patients will also describe non-specific manifestations and feel generally unwell. As sepsis worsens or septic shock develops, patients may experience confusion or decreased alertness, particularly in older adults. Neurological dysfunction, including confusion, delirium, drowsiness, seizures, and coma, happens in about half of patients who have sepsis and are admitted into an ICU. Other manifestations of a causative infection may also be present. As manifestations worsen, blood pressure will decrease (systolic blood pressure [SBP] less than 90 mm Hg or mean arterial pressure [MAP] less than 70 mm Hg), and initially, the skin will feel warm. Late manifestations of sepsis include cool and pale extremities, peripheral cyanosis, and mottling. Other manifestations (dyspnea, oliguria, obtundation, absent bowel sounds) may be present in patients who experience MODS. APRNs should also be aware that preexisting diseases or medications will modify some of these findings. For example, older adults, patients who have DM, and patients who are taking beta-blockers may not exhibit appropriate tachycardia in response to hypotension. Patients who have chronic hypertension may also develop critical hypoperfusion at a blood pressure that is higher than in healthy patients, known as relative hypotension (Cavaillon et al., 2020; Forrester, 2023; Gauer et al., 2020; Neviere, 2023).
Clinical manifestations of early and late neonatal sepsis include apnea, difficulty breathing, cyanosis, fast or slow heart rate, poor perfusion, irritability, lethargy, hypotonia, seizures, vomiting, abdominal distension, food intolerance, gastric residue, hepatomegaly, unexplained jaundice, inability to regulate body temperature, petechiae, and purpura. APRNs should be aware that pediatric patients can develop severe and prolonged tachycardia without associated hypotension until acute decompensation occurs (Bokhari, 2023a; Neviere, 2023; Procianoy & Silveira, 2020).
Table 2
Initial Evaluation of Common Sources Associated With Sepsis
Site | Manifestations | Initial Microbiologic Evaluation |
Upper respiratory tract | Pharyngeal inflammation with exudate with or without swelling and lymphadenopathy | Aerobic throat culture |
Lower respiratory tract | Pleuritic chest pain, productive cough, consolidative auscultatory findings | Aerobic sputum culture, urinary antigen testing (Legionella, pneumococcus), rapid influenza |
Wound or burn | Swelling, erythema, drainage (pus) | Gram stain and culture of drainage |
Bone | Swelling, warmth, pain, decreased use | Magnetic resonance imaging (MRI), blood culture, bone culture by interventional radiology (IR) |
Joint | Swelling, warmth, pain, decreased range of motion | Arthrocentesis with cell counts, Gram stain, and culture |
GI | Abdominal pain, distention, nausea, vomiting | Stool culture (Salmonella, Shigella, Campylobacter, C. diff) |
Urinary tract | Dysuria, urgency, back pain | Urine culture |
Genital | urinary frequency, cloudy urine, dysuria, and urgency Female: vaginal discharge, lower abdominal pain Male: prostatic tenderness | Female: endocervical and high vaginal swabs Male: urine Gram stain and culture |
Central nervous system | Manifestations of meningeal irritation | Cerebrospinal fluid cell count, protein, glucose, Gram stain, and culture |
Vascular catheters (arterial, central venous) | Redness or drainage at the insertion site | Blood culture (from catheter and peripheral) and culture of tip (if removed) |
(Bokhari, 2023b; Neviere, 2023)
The identification of an organism on culture for a patient who has suspected sepsis is supportive of the diagnosis but is not required. Since up to 50% of patients who have sepsis will not have a positive culture, it is not included in diagnostic criteria. Similarly, the identification of the organism is helpful in the selection of antimicrobials but is not required to begin treatment. There are no specific radiologic signs that specifically identify sepsis other than those findings associated with a specific site infection, such as pneumonia. Similarly, laboratory tests may be non-specific and are often associated with the underlying cause of sepsis or MODS (Bokhari, 2023b; Neviere, 2023).
Diagnosis
Sepsis has been challenging to define as a diagnosis. In the hope of finding a consistent diagnosis for treatment and clinical trials, a formal definition was developed by the American College of Chest Physicians and the Society of Critical Care Medicine (SCCM). This definition has been modified as the understanding of sepsis has become more precise. These definitions are not diagnostic of sepsis since they do not comprehensively include specific criteria for infection identification. The first definition of sepsis, or Sepsis-1, was developed in 1991 and focused on the patient demonstrating manifestations of SIRS (fulfilling two or more of the SIRS criteria as seen in Table 1) as a response to infection. Sepsis-1 was defined as an infection or suspected infection that led to the onset of SIRS. Sepsis-2 criteria were defined in 2001 and were essentially unchanged from the original Sepsis-1 definition. The patient had to satisfy at least two of the SIRS criteria along with a suspected or confirmed infection. Sepsis-3 is the latest definition of sepsis, published in 2016. This update confirmed that while nonspecific SIRS criteria (pyrexia, neutrophilia) often facilitate the diagnosis of infection, the established use of two SIRS criteria to identify sepsis was "unanimously unhelpful" (Singer et al., 2016, p. 803). The revised definition establishes sepsis as “life-threatening organ dysfunction caused by a dysregulated host response to infection” (Singer et al., 2016, p. 801). They suggest operationalizing organ dysfunction using the Sequential (sepsis-related) Organ Failure Assessment (SOFA) score that is increased by two or more points. Severe sepsis was defined as sepsis in the presence of new-onset organ dysfunction, but this was replaced in Sepsis 3 with an updated definition of septic shock. Sepsis 3 defines septic shock as a subset of sepsis characterized by profound underlying circulatory and cellular/metabolic abnormalities leading to greater than 40% mortality risk. It is often identified clinically by persistent hypotension requiring vasopressor therapy to maintain a MAP of at least 65 mm Hg and serum lactate levels greater than 2 mmol/L (18 mg/dL) despite sufficient fluid and volume resuscitation (Marik & Taeb, 2017; Neviere, 2023; Singer et al., 2016).
There is no single diagnostic test or screening tool for sepsis, nor does a single set of criteria identify sepsis with perfect accuracy. In addition, APRNs should be aware that sepsis definitions are not unanimously accepted, with the Centers for Medicare and Medicaid Services (CMS) still supporting the previous definition. The Adult Sepsis Event (ASE) offers one method of retrospectively defining sepsis (not diagnosing it). The ASE captures the widest variety of patients who have hCW sepsis. To receive a diagnosis of sepsis, a patient must have demonstrated two components of criteria A and organ dysfunction from criteria B, as summarized in Table 3 (CDC, 2018).
Table 3
Adult Sepsis Event (ASE)
Criteria A: Presumed Infection |
Blood culture (regardless of the result) and at least four qualifying antimicrobial days (QAD), starting 2 days before and 2 days after the collection of the blood culture |
Criteria B: Organ Dysfunction (at least one or more of the following within the 2 days before or 2 days after collection of blood culture) |
Initiation of a new vasopressor infusion (dopamine [Intropan], epinephrine [Adrenalin], norepinephrine [Levophed], phenylephrine [Vazculep], or vasopressin [Vasostrict]) |
Initiation of invasive mechanical ventilation |
Doubling of serum creatinine or greater than or equal to 50% decrease in estimated glomerular filtration rate (GFR) over baseline (excluding patients who have end-stage renal disease [ESRD]) |
Total bilirubin greater than 2 mg/dL and increased by 100% from baseline |
Platelet count less than 100 cells/µL and over 50% decline from baseline |
Optional: serum lactate greater than 2 mmol/L |
(CDC, 2018)
The ASE supports the surveillance of adult patients in an acute hospital setting and the tracking of sepsis incidence and outcomes within a facility. The resulting data can be used for quality-improvement initiatives or epidemiology and public health research. The ASE is not recommended for the surveillance of pediatric patients as it has not been validated in this population (CDC, 2018).
Staging and Scoring
In addition to multiple definitions, many scoring and staging systems have been developed for sepsis. These scoring and staging systems identify the severity and predict morbidity and mortality in patients who have sepsis. There is a wide variation in the diagnostic accuracy of these tools, with many of them having poor predictive values. While there are many scoring systems, this module will focus on the SOFA score, the Quick SOFA (qSOFA), the National Early Warning Score (NEWS), the Modified Early Warning Score (MEWS), and the Predisposition, Insult/Infection, Response, and Organ dysfunction (PIRO) staging system. The qSOFA and NEWS are the two most commonly used scores for the identification of early sepsis (Evans et al., 2021; Neviere, 2023).
The surviving sepsis guidelines recommend that health care systems use performance improvement programs for sepsis that include sepsis screening for acutely ill, high-risk patients with standard procedures for treatment. When these programs are in place, they are associated with better adherence to sepsis bundles and a reduction in mortality. The specific components of these programs do not appear as important as the presence of a program that includes sepsis screening and metrics. Although there is a wide variation in the sensitivity and specificity of these tools, they are important in early identification and timely intervention for patients who have sepsis (Evans et al., 2021).
SOFA is a simple scoring system that notes the number and severity of failure in six organ systems, including the respiratory system (i.e., PaO2/FiO2), coagulation (i.e., platelet count), cardiovascular system (i.e., MAP), liver (i.e., bilirubin level), kidneys (i.e., creatinine and/or urine output), and neurological system (i.e., Glasgow Coma scale). It was developed in 1994 to describe the degree of organ failure over time. Scores range from 0 to 24 (0-4 per organ system), and higher scores predict a higher possibility of mortality. The SOFA score should be calculated on admission before the initiation of treatment and then every 24 hours for daily monitoring of acute morbidity of patients who are in an ICU. Clinical guidelines define MODS as acute changes in the SOFA score of 2 or more points due to the infection. While originally developed to measure morbidity and not outcomes, the developers acknowledged that measurements of morbidity are associated with predicting mortality (CDC, 2018; Lambden et al., 2019; Marik & Taeb, 2017; Neviere, 2023; Vafaei et al., 2019; Vincent et al., 1996).
The SOFA score is a better predictor of inpatient mortality of patients who are in an ICU and have suspected infection than the SIRS criteria. In addition to the SOFA score, the qSOFA was developed as a simplified method of identifying patients who have sepsis and are at risk of a prolonged ICU stay and mortality. Since the qSOFA does not require laboratory results, it may be more useful when evaluating patients with sepsis at the bedside. It is a better mortality predictor for those with suspected infection who are not in the ICU (Forrester, 2023; Lehman & Dendache, 2020). The qSOFA is summarized below in Table 4.
Table 4
qSOFA Score
qSOFA Criteria | Points |
Respiratory rate greater than 22/minute | 1 |
Change in mental status (Glasgow Coma Score less than 15) | 1 |
SBP less than 100 mm Hg | 1 |
(Evans et al., 2021; Forrester, 2023)
A qSOFA score greater than 2 points indicates multiorgan dysfunction. While the qSOFA score is a simplified method for screening, recent literature has found that it may not be as accurate for early risk assessment. Studies have found that the qSOFA is more specific but less sensitive than the SIRS criteria for early identification of infection-induced organ dysfunction. The 2021 surviving sepsis guidelines caution against using the qSOFA and SIRS criteria as both may not be ideal screening tools for sepsis. They put forth a new strong recommendation that the qSOFA not be used as a single screening tool for sepsis or septic shock and recommend the NEWS or MEWS (Evans et al., 2021).
The NEWS score is the most commonly used early warning score worldwide and is the preferred score for screening for sepsis. NEWS is an aggregate scoring system derived from six physiologic parameters, including respiratory rate, oxygen saturation, the need for supplemental oxygen, SBP, heart rate, LOC or new confusion, and body temperature. LOC is measured using the AVPU (Alert, Voice, Pain, Unresponsive) scale. A score is allocated for each parameter with the magnitude of the score reflecting how much the parameter varies from the norm. The aggregate score (0 to 20) represents the risk of death from sepsis and ranges from 0 to 4 (low risk), 5 to 6 (medium risk), and 7 or more (high risk). See Table 5 for the NEWS criteria (Doyle, 2018; Neviere, 2023).
Table 5
NEWS Criteria
Physiologic Parameter | 3 | 2 | 1 | 0 | 1 | 2 | 3 |
Respiratory rate (breaths/minute) | ≤8 | 9 to 11 | 12 to 20 | 21 to 24 | ≥25 | ||
Oxygen saturation | ≤91% | 92% to 93% | 94% to 95% | ≥96% | |||
Supplemental oxygen | Yes | No | |||||
Systolic blood pressure (mmHg) | ≤90 | 91 to 100 | 101 to 110 | 111 to 219 | ≥220 | ||
Heart rate (beats/minute) | ≤40 | 41 to 50 | 51 to 90 | 91 to 110 | 111 to 130 | ≥131 | |
Level of consciousness | A | V, P, or U | |||||
Temperature (° F [° C]) | ≤95 (35) | 95.2 to 96.8 (35.1 to 36) | 97 to 100.4 (36.1 to 38) | 100.6 to 102.2 (38.1 to 39) | ≥102.4 (39.1) |
(Almutary A, et al., 2020, Doyle, 2018; Neviere, 2023)
Infection and Drug Resistance 2020 13 3843-3851. Originally published by, adapted and used with permission from Dove Medical Press Ltd.
The MEWS tool is based on the NEWS score; it uses physiological parameters to identify patients at increased risk for catastrophic deterioration, ICU admission, and/or death. The MEWS is used throughout many health care organizations as part of nursing assessments, although individual health care systems often modify the parameters and threshold for a critical score. The MEWS score added urine output (mL/kg/hr) as a parameter, removed oxygen saturation and the need for supplemental oxygen from the original NEWS scale, and modified the scoring of other parameters to make them more or less sensitive. The original MEWS scale was designed to trigger provider notification for a score of 4 or more out of 17 in surgical patients (Doyle, 2018; Gardner-Thorpe, 2006).
The PIRO system was suggested in 2001 at the Sepsis-2 International Conference, published in 2003, and fully developed in 2008 to predict 28-day mortality, ICU admission, and the development of multiorgan dysfunction in patients admitted to the ICU. The respiratory rate, heart rate, and bands are evaluated as well as organ dysfunction, SBP, and platelet count. The PIRO score is simple, making it more practical for busy emergency departments (EDs), as it is based on four main components that can be quickly assessed. Since its development, three more PIRO scores have been validated for risk stratification or staging in sepsis—the Moreno PIRO (using PIR only), Howell PIRO, and Rubulotta PIRO (File, 2022; Howell et al., 2011; Moreno et al., 2008; Rathour et al., 2015; Rubulotta et al., 2009; Songsangjinda & Khwannimit, 2020; Vafaei et al., 2019).
The Howell PIRO criteria and scoring system incorporates patient predisposition factors (i.e., age, skilled nursing facility residency, and the presence of certain underlying conditions such as COPD, liver disease, and malignancy). The user categorizes the infection as skin/soft tissue, pneumonia, or other. The Response categories require the input of the patient's respiratory rate, heart rate, and percent of bands. The final category (i.e., organ dysfunction) requires the patient's systolic blood pressure (SBP), blood urea nitrogen (BUN), lactate level, platelet count, and whether the patient is exhibiting signs of respiratory failure/hypoxemia. Individual criterion are given scores ranging from 0-4, with a higher total score indicating a higher risk of mortality in hospitalized patients with suspected infection (Howell et al., 2011; Rathour et al., 2015).
The Surviving Sepsis Campaign (SSC) App provides a screening tool for identifying patients who have sepsis. The app allows users to set up alerts for the sepsis bundles and quickly access guidelines and the Surviving Sepsis website. The app is available for iOS and Android devices. The app also directs users to the SCCM’s content and website (SCCM, 2021).
Treatment and Management of Care
The management of sepsis requires prompt recognition, appropriate antimicrobial use, hemodynamic support, and infection control. The management of sepsis is moving away from strict protocols in favor of guidelines for individualized care. Recommendations from the SSC guidelines committee are often used to guide the care of patients who have sepsis and septic shock (Dugar et al., 2020; Evans et al., 2021; Schmidt et al., 2024).
Initial Management
The management and treatment of sepsis have evolved considerably over the last two decades. However, mortality is still a concern with sepsis management, indicating that improvements in care are still needed. Therapies for the management and treatment of sepsis focus on the infection, host response, and organ dysfunction. Early aggressive medical therapy is essential for patients who have suspected sepsis. Securing the patient’s airway, correcting hypoxemia, and establishing venous access for quick administration of fluids and antimicrobials are priorities in the initial management of patients who have sepsis or septic shock. The patient should have venous access established as soon as possible. Peripheral venous access may be sufficient, but many patients will require central venous access at some point. The administration of resuscitative fluids and antimicrobials should not be delayed while waiting on a central line (Bullock & Benham, 2023; Evans et al., 2021; Schmidt et al., 2024).
A history and examination as well as laboratory tests and imaging studies will often be obtained simultaneously while venous access is attained, and the patient’s airway is stabilized. Vital signs should be obtained immediately and frequently to monitor for deterioration. For any patient who has manifestations of hypoxia, supplemental oxygen and continuous pulse oximetry should be initiated (peripheral SpO2 target is 90% to 96%). Non-invasive ventilation, high-flow oxygen, or intubation and mechanical ventilation may be necessary to support oxygenation and increased work of breathing (Evans et al., 2021; Schmidt et al., 2024). The following laboratory and imaging tests should be acquired within 45 minutes of presentation.
- Complete blood count (CBC) with differential
- Comprehensive metabolic profile (CMP)
- Liver function tests
- Coagulation studies, including D-dimer
- Serum lactate and procalcitonin
- Peripheral blood cultures from at least two sites
- Urinalysis
- Tissue, wound, or other cultures from suspected sources of infection (see Table 2)
- Arterial blood gas
- Imaging of the suspected site of infection (chest x-ray, computed tomography [CT] of the chest or abdomen) (Evans et al., 2021; Schmidt et al., 2024)
Although the quick collection of laboratory and microbiological testing is important, the initiation of fluids and antibiotics should not be delayed if these cannot be obtained. Cultures should not be drawn from indwelling or central vascular access catheters. These are often colonized with skin flora and will increase the likelihood of a false-positive culture result. If blood cultures are drawn from an intravenous (IV) line, a second specimen should be obtained from another peripheral venipuncture site (Evans et al., 2021; Schmidt et al., 2024).
Fluid Resuscitation
Timely, effective fluid resuscitation is critical for patients with sepsis-induced tissue hypoperfusion. Initial resuscitation should begin immediately. For resuscitation from sepsis-induced hypoperfusion or septic shock, administer at least 30 mL/kg of IV crystalloid fluid starting within the first hour and concluding within the first 3 hours. Beyond this, additional fluids should be given accordingly based on a reassessment of the patient’s hemodynamic status. In a retrospective analysis, it was found that patients who did not receive 30 mL/kg of IV crystalloids within the 3 hours of sepsis onset were at increased risk of mortality and ICU length of stay, along with delayed resolution of hypotension. The SSC guidelines recommend using balanced crystalloids (lactated Ringers) instead of normal saline to reduce the risk of hyperchloremic metabolic acidosis, renal vasoconstriction, increased cytokine levels, and acute kidney injury (AKI). Reassessment should include clinical examination and evaluation of at least heart rate, blood pressure, central venous pressure (CVP), arterial oxygen saturation, respiratory rate, temperature, and urine output. However, heart rate, CVP, and SBP alone are poor indicators of fluid status. Dynamic measures have a better diagnostic accuracy at predicting fluid responsiveness. These measures include passive leg raising combined with CO measurement, fluid challenges against stroke volume, systolic pressure or pulse pressure, and an increase of stroke volume in response to changes in intrathoracic pressure. When an elevated serum lactate level is present, fluid resuscitation should be administered to decrease the lactate to a normal level. The evaluation of any other available information or variables, including invasive and noninvasive monitoring, should be included. SSC guidelines recommend an initial target MAP of 65 mm Hg. If advanced hemodynamic monitoring is not available, the SSC guidelines recommend using temperature of the extremities, skin mottling, and capillary refill time (Evans et al., 2021; Schmidt et al., 2024).
Most patients will require continued fluid administration following initial resuscitation. This administration should be balanced with the risk of fluid accumulation and overload. Fluid resuscitation beyond the initial 30 mL/kg should be administered in prescribed, rapidly infused boluses (500 mL). The patient’s response is assessed before and after each bolus by objective measures of stroke volume and CO. The patient should be evaluated for manifestations of pulmonary edema. IV therapy can be repeated until blood pressure and signs of tissue perfusion are acceptable, the patient demonstrates manifestations of pulmonary edema, or the care team decides fluid is not augmenting perfusion. Albumin is recommended in those who receive large volumes of crystalloids, but its high cost precludes its routine use for fluid resuscitation initially. Starches, such as hydroxyethyl starch (HES), and gelatin are not recommended due to a lack of proven effectiveness (Evans et al., 2021; Schmidt et al., 2024).
Antimicrobials
For the treatment of an unconfirmed infection, the SSC guidelines recommend continuously re-evaluating for alternative diagnoses and discontinuing antimicrobials if an alternative cause is determined and infection is ruled out. Routine microbiologic cultures are obtained before initiating antimicrobial therapy in patients who have suspected sepsis or septic shock. Appropriate microbiologic cultures should include at least two sets of blood cultures, including aerobic and anaerobic. However, microbiologic cultures should not delay the initiation of antimicrobials by more than 45 minutes. Given that there is no gold standard for diagnosing sepsis, it can be challenging to determine when the cause is infectious versus non-infectious. This can present challenges when determining whether it is appropriate to discontinue antimicrobials. Continuous reassessment of the need for antimicrobials is recommended (Evans et al., 2021; Schmidt et al., 2024).
IV antibiotics should be administered as soon as sepsis is diagnosed. Each hour delay is associated with an increase in patient mortality. Studies have also shown an increase in organ injury with delays in antibiotic treatment, especially for patients who have septic shock. The SSC guidelines recommend that antimicrobials be initiated immediately (within 1 hour) for anyone who has confirmed or probable sepsis or shock. For patients who have possible sepsis without shock, the SSC guidelines recommend a rapid assessment to determine infectious or non-infectious etiologies to determine the need for antimicrobials (administration within 3 hours). Delays in the initiation of antimicrobials are often related to organizational factors, such as the hospital drug-delivery chain. Quality improvement initiatives, such as defined order sets for suspected sepsis, can address delays due to drug delivery. A patient factor that can delay the initiation of antimicrobial treatment is difficulty with vascular access. Intramuscular preparations of antimicrobials are available and can be used when vascular access cannot be established promptly. Procalcitonin levels are not suggested to guide antimicrobial initiation (Evans et al., 2021; Schmidt et al., 2024).
Empiric broad-spectrum antimicrobial therapy is recommended to cover more possible pathogens. Once the culture results are obtained and the pathogen is identified, treatment can be narrowed. Awaiting culture results causes a significant delay, increasing the risk of patient morbidity and mortality. The empiric antimicrobial therapy chosen will depend on the patient’s history (chronic organ failure, current medications, the use of antimicrobials in the past three months, patient allergies), clinical status, epidemiologic factors (is the infection considered community-acquired or hospital-acquired and typical local pathogens), comorbidities (the presence of immunodeficiency due to neutropenia, splenectomy, HIV, defects of immunoglobulin), and the site of infection. In addition, the APRN should assess the risk factors for multidrug-resistant organisms (MDROs; i.e., recent hospital stay, IV antibiotics, recurrent skin infections, chronic wounds, the presence of invasive devices, hemodialysis, prior infections with MDROs). The APRN should obtain a detailed medical and social history to identify proper antimicrobial therapy (Evans et al., 2021; Schmidt et al., 2024).
Empiric combination therapy is recommended with at least two antibiotics of different classes in patients who have severe infections or septic shock. The antimicrobials should target the most likely bacterial pathogen. This combination therapy should not be routinely used for bacteremia and sepsis without shock. Also, combination therapy is not recommended routinely for neutropenic sepsis. Often, a broad-spectrum carbapenem such as meropenem (Merrem), imipenem/cilastatin (Primaxin), or doripenem (Doribax) will be used. Another option is an extended-range penicillin/beta-lactamase inhibitor combination such as piperacillin/tazobactam (Zosyn) or ticarcillin/clavulanate (Timentin). Several third-generation or higher cephalosporins (ceftriaxone [Rocephin], cefepime [Maxipime]) are also recommended as part of a multidrug regimen. The APRN should consider the risk of resistance to broad-spectrum beta-lactams and carbapenems among gram-negative bacteria in community and health care-acquired infections. The addition of antimicrobials that will cover gram-negative pathogens is recommended for critically ill patients who have sepsis, especially if MDROs are suspected. The SSC guidelines recommend using two antimicrobials with gram-negative coverage for patients who are at high risk for MDROs (one agent in those at low risk). Vancomycin (Vancocin), daptomycin (Cubicin), linezolid (Zyvox), or teicoplanin (Targocid) can be used when MRSA is suspected. However, empiric antimicrobials for MRSA are not recommended for patients who are at low risk for MRSA. If Pseudomonas is likely, ceftazidime (Fortaz), cefepime (Maxipime), imipenem (Primaxin), meropenem (Merrem), piperacillin/tazobactam (Zosyn), a fluoroquinolone, aminoglycoside, or monobactam should be included. If Legionella is suspected, the addition of a macrolide or fluoroquinolone should be considered (Evans et al., 2021; Schmidt et al., 2024).
Another pathogen to consider is the Candida species, which leads to a fungal infection. Patients who are at risk for Candida infections include those who are immunocompromised; those who have prolonged invasive vascular devices, TPN, or necrotizing pancreatitis; or those who had recent major surgery, extended broad-spectrum antibiotics therapy, a lengthy hospital or ICU stay, or recent fungal infection. Empiric use of antifungals such as anidulafungin (Eraxis), micafungin (Mycamine), or caspofungin (Cancidas) is preferred in patients who have severe illness or neutropenia, especially those who have septic shock and are at increased risk of a fungal infection. Triazoles can be used for hemodynamically stable patients, those who are not seriously ill, and patients who have not had previous triazole exposure. Amphotericin B (Abelcet or Ambisome) is an alternative in patients who cannot take echinocandins. An infectious disease specialist should be consulted. Outcomes for patients who have sepsis can be improved with the early involvement of infectious disease specialists (Evans et al., 2021; Schmidt et al., 2024).
Once the pathogen has been identified, the antimicrobial therapy should be narrowed to the most effective agent, as indicated by sensitivity results. Approximately 50% of patients diagnosed with sepsis do not have a diagnosed causative pathogen. If cultures are drawn after the initiation of antimicrobial therapy, this can affect culture and sensitivity results. Even if cultures are negative, antimicrobials should be de-escalated based on clinical improvement. If an infection is not found, antimicrobial therapy should be stopped to decrease the possibility that antimicrobial-resistant pathogens will develop. The decision to continue, reduce, or stop antimicrobial treatments should be made on a case-by-case basis using the best clinical judgment (Evans et al., 2021; Schmidt et al., 2024).
The most recent recommendations caution against sustained systemic antimicrobial administration for prophylaxis in patients who are in inflammatory, non-infectious states (severe pancreatitis, burn injuries). Avoiding systemic antimicrobial therapy when there is no suspected infection can minimize the likelihood of infection with an antimicrobial-resistant pathogen (Evans et al., 2021; Schmidt et al., 2024).
Antimicrobial dosing should be based on pharmacokinetic and pharmacodynamic principles and specific drug properties in patients who have sepsis. There are several factors to consider when determining optimal dosing for critically ill patients who have sepsis. They have an increased frequency of hepatic and renal dysfunction. Furthermore, aggressive fluid resuscitation causes a rapid expansion in extracellular volume and increases the volume of distribution for most antimicrobials, resulting in suboptimal drug levels. Antimicrobial therapy in patients who have sepsis should be initiated with a high loading dose of each antimicrobial agent used. Prolonged infusions are favored over conventional bolus infusions. Peak plasma targets should be monitored for continued treatment. Aminoglycosides attain peak drug plasma concentration with once-daily dosing. Once-daily dosing with aminoglycosides can preserve renal function. The recommended target for a vancomycin (Vancocin) trough is 15 to 20 mg/L. A higher loading dose (25 to 30 mg/kg) is recommended to reach the target trough. For beta-lactams such as piperacillin/tazobactam (Zosyn), the dosing should be more frequent (every 6 or 8 hours) to sustain therapeutic plasma concentrations. A pharmacy consultation is beneficial in calculating loading doses and adjusting dosages based on peak and trough levels (Evans et al., 2021; Schmidt et al., 2024).
When combination therapy is used, and culture results are not helpful, the antimicrobials should be tapered based on clinical improvement and professional judgment. Some observational studies have demonstrated that early tapering of multidrug antimicrobials is associated with equal or superior clinical outcomes for sepsis and septic shock. While there is a consensus on the recommendation for early tapering of multiple antimicrobials, there are no precise criteria for triggering the decrease in medications. Decreasing the antimicrobial therapy should be based on the patient’s clinical progress, infection resolution, and the fixed duration of the prescribed therapy. A duration of 3 to 8 days may be adequate for most patients. The SSC guidelines recommend daily assessment for de-escalation of antibiotics. Longer courses of treatment are appropriate in patients who are not demonstrating improvement in clinical response or for undrainable infection, bacteremia with Staphylococcus aureus, fungal or viral infections, or immunological deficiencies (Evans et al., 2021; Schmidt et al., 2024).
Procalcitonin is undetectable in healthy states. However, it rises rapidly in response to pro-inflammatory stimuli, especially bacterial infection. The measurement of serum procalcitonin is used in many parts of the world during the diagnosis of acute infection, helping define the duration of antimicrobial therapy. The procalcitonin level directly correlates with the severity of illness. The SSC guidelines recommend not using procalcitonin to decide when to start antimicrobials and instead use only clinical evaluation. However, procalcitonin levels are recommended to support the decision to shorten antimicrobial therapy in patients who have sepsis. Procalcitonin levels can also inform the decision to discontinue antibiotics in patients who had suspected sepsis but limited or no evidence of infection. The SSC guidelines suggest combining procalcitonin levels with clinical assessment data to decide when to discontinue antimicrobials in patients who have sepsis or septic shock with adequate source control, but the optimal duration of therapy is unclear (Evans et al., 2021; Schmidt et al., 2024).
Source Identification and Control
A potential specific anatomical diagnosis of infection that would require source control should be rapidly identified or excluded via focused history and physical examination. If source control is required, this should be performed as soon as practical (within 12 hours). This is to include abscess drainage, debridement of infected necrotic tissue, removal of an infected device, or repair of gastrointestinal perforation, ischemic bowel, or volvulus. Other foci of infection may include pyelonephritis with obstruction or abscess, empyema, septic arthritis, cholangitis, and cholecystitis. Prompt removal of any intravascular access device that is a suspected source of sepsis is recommended once another vascular access has been established. Central venous catheters (CVCs) and other intravascular devices are a possible source of sepsis. Although implanted or tunneled catheter-related infections may be treated with prolonged antimicrobial therapy if removal is not feasible, catheter removal is preferred. Advanced imaging studies, such as computed tomography (CT), or ultrasound may be helpful. Sample collection (bronchoalveolar lavage, fluid aspiration, urine culture) may also be indicated (Evans et al., 2021; Schmidt et al., 2024).
Vasopressor and Inotropic Therapy
Vasopressor therapy is another fundamental component of sepsis or septic shock treatment. The goal of vasopressor therapy is to correct hypotension and improve organ perfusion in those who remain hypotensive despite adequate fluid resuscitation or develop cardiogenic pulmonary edema. Norepinephrine (Levophed) is the first-line vasopressor recommended by the SSC guidelines. It is a potent alpha-1 adrenergic agent that improves hypotension more effectively in patients who have septic shock due to a stronger vasoconstrictive effect on arteries and results in reduced mortality and a lower risk of arrhythmias. Other frequently used vasopressors are epinephrine (Adrenalin), vasopressin (Vasostrict), dopamine (Intropin), and dobutamine (Dobutrex). Vasopressin (Vasostrict) can be added to norepinephrine (Levophed) with the intent of increasing the MAP to the desired level instead of escalating the norepinephrine dose (0.25 to 0.5 microgram/kg/min). It is an antidiuretic hormone that may be appropriate in patients who have significant tachycardia as it lacks any beta-adrenergic effects. For patients who have an inadequate MAP despite norepinephrine (Levophed) and vasopressin (Vasostrict), the SSC guidelines recommend adding epinephrine (Adrenalin). It tends to have more of an effect on heart rate and contractility than norepinephrine (Levophed) but less vasoconstriction. Dopamine (Intropin) is generally avoided but may be considered as an alternative to norepinephrine (Levophed) in those who have significant bradycardia or a low risk of tachyarrhythmias as it causes more tachycardia and arrhythmias than norepinephrine (Levophed). Low-dose dopamine (Intropin) should not be used for renal protection but can be helpful in patients who have compromised systolic function. Dopamine (Intropin) may also have immunosuppressive tendencies. Dobutamine (Dobutrex) can be added to norepinephrine in patients who have evidence of persistent hypoperfusion related to low CO despite adequate fluid status as it seems to have a strong inotropic effect despite being a vasodilator. It is considered a beta-adrenergic inotrope. All patients requiring vasopressors should have central venous access and an arterial catheter placed as soon as possible if resources are available, especially if blood pressures are labile or restoration of perfusion is expected to be protracted. Vasopressors can be administered peripherally for a short period in a vein proximal to or within the antecubital fossa until central access is secured. With patients who have septic shock, measurements of blood pressure using a cuff can be inaccurate. An arterial cannula provides a more accurate measurement (Evans et al., 2021; Schmidt et al., 2024; Shi et al., 2020). Initial and maintenance dosing for these agents include the following.
- norepinephrine (Levophed) 5 to 15 mcg/minute (0.05 to 0.15 mcg/kg/minute) with a maintenance dose of 2 to 80 mcg/minute (0.025 to 1 mcg/kg/minute)
- epinephrine (Adrenalin) 1 to 15 mcg/minute (0.01 to 0.2 mcg/kg/minute) with a maintenance dose of 1 to 40 mcg/minute (0.01 to 0.5 mcg/kg/minute)
- dopamine (Inotropin) 2 to 5 mcg/kg/minute with a maintenance dose of 2 to 20 mcg/kg/minute
- vasopressin (Vasostrict) 0.03 units/minute with a maintenance dose of 0.01 to 0.04 units/minute
- dobutamine (Dobutex) 2 to 5 mcg/kg/minute with a maintenance dose of 2 to 10 mcg/kg/minute (Schmidt et al., 2024)
- phenylephrine (Neo-Synephrine) 40 to 160 mcg/minute (0.5 to 2 mcg/kg/minute) until stable, then 20 to 400 mcg/minute (0.25 to 5 mcg/kg/minute)
Glucocorticoid Therapy
Glucocorticoids are not recommended for routine use in patients who have sepsis but are frequently provided to patients who have septic shock. Fluid resuscitation and vasopressors should be used first to restore hemodynamic stability. If vasopressors are still required (epinephrine or norepinephrine greater than or equal to 0.25 mcg/kg/minute for at least 4 hours after initial administration) to maintain MAP, IV hydrocortisone (Solu-Cortef) is recommended at 200 mg per day intravenously. Moderate-quality evidence showed accelerated resolution of shock and an increase in vasopressor-free days. Several trials have shown elevated hyperglycemia and hypernatremia in patients who have septic shock and receive hydrocortisone (Solu-Cortef) therapy. Routine labs should include measurements for these values in patients receiving hydrocortisone (Solu-Cortef) therapy (Evans et al., 2021; Schmidt et al., 2024). Glucocorticoid therapy may also be indicated in patients who present with adrenal insufficiency, as evidenced by cortisol levels (Forrester, 2023).
Blood Products
For patients who have sepsis, red blood cell (RBC) transfusions should only occur once the hemoglobin concentration decreases to under 7 g/dL in adults unless there are extenuating circumstances (severe hypoxemia, acute hemorrhage, myocardial ischemia). Erythropoietin should not be used to treat sepsis-associated anemia. Fresh frozen plasma (FFP) is not recommended to correct clotting abnormalities when there is no bleeding or planned invasive procedure. Current recommendations indicate that FFP should be transfused in patients who have diagnosed deficiencies in coagulation factors in the presence of active bleeding. Prophylactic platelet transfusions should occur when counts are below 10,000/mm3(10x109/L), even if there are no signs of apparent bleeding. If the patient has a significant risk for bleeding and the counts are less than 20,000/mm3(10x109/L), prophylactic platelet transfusions are appropriate. Platelet transfusions are also appropriate if the patient has active bleeding or an invasive procedures planned with a platelet count under 50,000/mm3(10x109/L). IV immunoglobulin is not recommended in patients who have sepsis. Antithrombin—an abundant anticoagulant circulating in plasma—is also not recommended for treatment in patients who have. The drop in antithrombin plasma activity at the beginning of sepsis can result in DIC. Trials with antithrombin for adult patients who have sepsis have not demonstrated beneficial results with patient mortality, as antithrombin was associated with an increased risk of bleeding. Polymixin B hemoperfusion through an extracorporeal circuit for purification purposes is not recommended (Evans et al., 2021; Schmidt et al., 2024).
Oxygenation and Mechanical Ventilation
All patients who have sepsis should receive continuous monitoring with pulse oximetry with supplemental oxygen. The patient’s condition may require assistance with oxygenation or ventilation due to the increased work of breathing. Supplemental oxygen delivery should be attempted first. If this is insufficient, noninvasive ventilation (NIV) and high-flow oxygen (HFNC) can be used to avoid complications from invasive mechanical ventilation. The SSC guidelines recommend the use of HFNC over NIV for sepsis-induced hypoxemic respiratory failure due to the risk of gastric insufflation, aspiration, facial skin breakdown, and excessively high tidal volumes. HFNCs allow for warming and humidification of secretions, high flow rates, washout of nasopharyngeal dead space, and modest positive airway pressure effects. The risks and benefits of NIV versus intubation should be considered individually because the evidence does not indicate that either is superior for the management of sepsis-induced hypoxemic respiratory failure (Evans et al., 2021; Schmidt et al., 2024).
If mechanical ventilation is deemed necessary for respiratory support in adult patients who have sepsis-induced acute respiratory distress syndrome (ARDS), a low target tidal volume (6 mL/kg of predicted body weight) is recommended. Plateau pressures of less than or equal to 30 cm H20 are recommended over higher plateau pressures. In adults who have moderate to severe sepsis-induced ARDS, higher positive end-expiratory pressure (PEEP) is recommended over lower PEEP to open lung units and promote gas exchange. Transient increases in transpulmonary pressure are designed to open collapsed, airless alveoli. These are called recruitment maneuvers and include temporary increases in airway pressure during mechanical ventilation. During tidal ventilation, some collapsed alveoli are adjacent to alveoli that are still inflated. When the alveoli are inflated, injuries can occur between the tissue. The cyclic collapse and re-expansion of each breath cause shear-induced injury. Furthermore, some alveoli remain inflated through the cycle and can become overinflated. The trauma of each cycle of expansion can cause cytokine release and contribute further to multiorgan failure and mortality. Recruitment maneuvers open collapsed lung tissue and prevent a cyclic collapse. Traditional recruitment maneuvers are recommended for adult patients who have sepsis-induced moderate to severe ARDS. Opening the atelectatic alveoli improves gas exchange. Care should be taken to prevent the overdistention of aerated lung units, leading to ventilator-induced lung injury and transient hypoxemia. The use of sustained continuous positive airway pressure (CPAP) has been shown to improve survival and reduce severe hypoxia. Recruitment maneuvers combined with higher levels of PEEP can be beneficial in patients who have severe hypoxemia. Any patient who receives this therapy should be monitored closely, and the recruitment maneuvers can be discontinued if the patient’s condition deteriorates. Recruitment can also occur without performing recruitment maneuvers by removing mucous plugs with suction or bronchoscopy, chest physiotherapy, and prone positioning. Incremental PEEP titration or strategy, such as non-traditional recruitment maneuvers, is not recommended (Evans et al., 2021; Schmidt et al., 2024).
Prone instead of supine positioning can be beneficial for adult patients who have moderate-severe sepsis-induced ARDS and a PaO2/FiO2 ratio below 200. Prone positioning during the first 36 hours of intubation for more than 12 hours a day has been shown to improve survival in these patients due to improved oxygenation and lung compliance. Prone positioning can be associated with accidental dislodgement of the endotracheal tube and an increased likelihood of pressure injuries because prone positioning limits the repositioning options to prevent pressure injuries (Evans et al., 2021).
Neuromuscular blocking agents (NMBAs) should be used for under 48 hours in adults who have moderate-to-severe sepsis-induced ARDS and a PaO2/FiO2 ratio below 150. The SSC guidelines recommend intermittent NMBA boluses over continuous infusion. NMBAs improve chest wall compliance and expansion, prevent respiratory desynchrony, and reduce peak airway pressure. Reduced oxygen consumption may also result from muscle paralysis by decreasing the work of breathing and the blood flow to respiratory muscles. Continuous or intermittent sedation should be minimized for patients who have sepsis and are mechanically ventilated. Succinylcholine (Anectin) and rocuronium (Zemuron) are often used when a rapid effect is desired. Rocuronium (Zemuron) is typically dosed at 0.6 to 1.2 mg/kg to get the same onset with a longer duration than succinylcholine (Anectin). Rocuronium (Zemuron) and vecuronium (Norcuron) can be antagonized with sugammadex (Bridion) at a dose of 16 mg/kg. Even with the pharmacological reversal, the patient may experience dangerous periods of hypoxia or hypoventilation due to opioid or sedative drugs that were possibly co-administered to facilitate rapid sequence intubation. Succinylcholine (Anectin) is the only depolarizing NMBA available and is typically dosed at 1 to 2 mg/kg for intubation purposes. It functions by competing with acetylcholine at the postsynaptic nicotinic receptors. It causes skeletal muscle fasciculations immediately after administration and can lead to malignant hyperthermia and transient hyperkalemia. It is typically reversed by administering an acetylcholinesterase inhibitor (neostigmine [Bloxiverz] or edrophonium [Enlon]). Nurse-directed protocols incorporating a sedation scale improve patient outcomes and decrease sedative use. Another method used to reduce sedation use is daily sedation interruption. Beta-2 agonists are also not recommended to treat patients who have sepsis-induced ARDS without bronchospasms. The routine use of a pulmonary artery catheter is also not recommended in patients who have sepsis-induced ARDS. When these patients are ready for weaning from mechanical ventilation, spontaneous breathing trials and weaning protocols should be used (Evans et al., 2021; Renew et al., 2020). Please see the NursingCE course on The Basics of Ventilator Weaning for additional information on weaning patients from mechanical ventilation.
Sepsis patients who are mechanically ventilated should have the head of their bed kept between 30 and 45 degrees to decrease the risk of aspiration and prevent the development of ventilator-associated pneumonia. The risk of developing ventilator-associated pneumonia is high in patients receiving enteral feedings. Patients should not receive enteral feedings while supine and should only be laid flat when necessary for procedures, hemodynamic measurements, or during episodes of hypotension (Evans et al., 2021).
Blood Glucose
Hyperglycemia, hypoglycemia, and increased glycemic variability are associated with increased mortality in patients who have sepsis. A protocol should be used to manage blood glucose in ICU patients who have sepsis. Insulin should be initiated when two consecutive blood glucose levels are greater than 180 mg/dL for a target glucose range of 144 to 180 mg/dL. Insulin infusion can be initiated at 1 to 4 units/hour and titrated to effect. Blood glucose levels should be monitored every 1 to 2 hours until glucose levels and insulin infusion rates are stable. Once stable, the patient’s blood glucose can be monitored every 4 hours in patients receiving continuous insulin infusions. Capillary blood glucose levels may not accurately depict arterial or plasma glucose levels; therefore, arterial blood rather than capillary blood is recommended for point-of-care testing in patients who have arterial catheters (Evans et al., 2021; Forrester, 2023).
Dialysis
Renal replacement therapy may be necessary for patients who have sepsis and AKI. The indications for renal replacement therapy are volume overload, metabolic acidosis, hyperkalemia, hyponatremia, hyperphosphatemia, encephalopathy, pericarditis, and persistent or progressive AKI. The standard thresholds for initiating renal replacement therapy include a pH of less than 7.1 to 7.2 or a serum bicarbonate level of less than 12 to 15 mmol/L. Renal replacement therapy may be needed earlier in mechanically ventilated patients to prevent severe acidemia that results from the combination of metabolic and respiratory acidosis. Renal replacement therapy is not recommended when not indicated. Multiple modes of renal support can be used, such as conventional intermittent hemodialysis (IHD), prolonged intermittent renal replacement therapy (PIRRT), and continuous renal replacement therapy (CRRT). Rapid solute clearance and ultrafiltration are used in IHD during brief treatments lasting 3 to 5 hours. The continuous therapies remove fluid gradually, with solute clearance happening over prolonged times. PIRRT treatments usually last between 8 and 16 hours and provide solute clearance faster than CRRT. CRRT and PIRRT are often used in patients who are hemodynamically unstable, but preference may vary with the facility (Evans et al., 2021; Tandukar & Palevsky, 2019).
Bicarbonate therapy (sodium bicarbonate) is not recommended to improve hemodynamics and reduce vasopressor requirements in patients experiencing hypoperfusion-induced lactic acidemia with a pH greater than 7.15. However, in the subset of patients who have severe metabolic acidemia (pH less than or equal to 7.2) and AKI (AKI Network score of 2 or 3), there is low-quality evidence to support the use of IV bicarbonate. Acutely ill patients who have sepsis should also receive pharmacological venous thromboembolism (VTE) prophylaxis with unfractionated heparin (UFH) or low-molecular-weight heparin (LMWH) unless contraindicated. The American Society of Hematology (ASH) recommends pharmacological prophylaxis in acute medical patients admitted to the hospital with increased VTE risk and acceptable bleeding risk. LMWH is preferred over UFH or direct oral anticoagulants (DOACs) secondary to its once-daily dosing regimen and reduced rate of complications. LMWHs (enoxaparin [Lovenox], dalteparin [Fragmin]) are subcutaneous medications that work by inhibiting thrombin and factor Xa. Treatment with both pharmacological and mechanical prophylaxis is not recommended. Mechanical prophylaxis (sequential compression device, foot pumps) in place of pharmaceutical prophylaxis is preferred in acute medical patients admitted to the hospital with an increased risk of bleeding (Evans et al., 2021; Schünemann et al., 2018).
Stress Ulcer Prophylaxis
Stress ulcers often develop in the GI tract of patients who are critically ill. These ulcers can be associated with significant morbidity and mortality. Patients who are at the highest risk for GI ulcers include those who are on mechanical ventilation for over 48 hours and those who have impaired clotting. Stress ulcer prophylaxis is essential in patients who have sepsis and risk factors for gastrointestinal bleeding. Proton pump inhibitors or H2 blockers are recommended. Proton pump inhibitors are used more frequently than H2 blockers and are more effective at preventing GI bleeding. The routine monitoring of gastric residual volume is not recommended unless the patient has a feeding intolerance or is at high risk for aspiration (Evans et al., 2021).
Nutrition
Patients who have sepsis and can tolerate enteral feedings should receive early enteral nutrition (within 72 hours). Parenteral nutrition, either alone or in conjunction with enteral nutrition, should be avoided due to its invasive nature and potential complications, such as an increased risk of infection. Enteral feeding intolerance is a common problem in critically ill patients, occurring in one-third of patients in the ICU, and is associated with adverse outcomes. Vomiting, aspiration of gastric contents, or high gastric residual volumes are seen with enteral feeding intolerance. This intolerance is more common in patients who have gastroparesis or diabetes or those receiving sedatives or vasopressors. During the first 7 days, the initiation of IV glucose and advancement of enteral feedings as tolerated are recommended along with prokinetic agents such as metoclopramide (Reglan) in patients who have feeding intolerance. A post-pyloric feeding tube is an option for nutritional support in patients who have feeding intolerance or a high risk of aspiration. These patients may require parenteral nutrition to meet their nutritional goals. Other treatments that have been used include omega-3 fatty acids and IV selenium. These measures are not recommended due to insufficient evidence. Similarly, arginine supplementation can lead to vasodilation and hypotension and is not recommended in patients who have sepsis. Glutamine levels are reduced in patients who have sepsis, and exogenous supplementation can improve the gut mucosa. The clinical significance of these findings and their benefit for patients who have sepsis have not been established (Evans et al., 2021; Seres, 2024).
Monitoring
Some patients who have sepsis will require admission to the ICU, such as those receiving vasopressor therapy or mechanical ventilation, and stable patients not exhibiting manifestations of shock may be transferred to the floor, assuming a quick response to fluid/antibiotic therapy. The decision to admit a patient who has sepsis to the ICU should be made within 6 hours, according to the SSC (Evans et al., 2021; Schmidt et al., 2024). All patients who have sepsis should receive close monitoring for improved MAP, urine output, vital signs (heart rate, respiratory rate, temperature, pulse oximetry), skin color, and mental status. Many patients who have sepsis require a CVC and an arterial catheter for monitoring purposes. Arterial catheters may be appropriate for patients who have labile blood pressure or unreliable sphygmomanometer readings or those on vasopressors or if dynamic measures of fluid responsiveness are desired. Common target measurements are MAP of greater than or equal to 65 mm Hg, although a target range for MAP (60 to 70 mm Hg as recommended) can be used instead of a specific number. A CVC may be appropriate when large volume fluid infusions or vasopressors are anticipated, peripheral access is subpar, or CVP or ScvO2 are desired for monitoring the hemodynamic response. If a CVC is being used to monitor fluid status and vital signs, a CVP target of 8 to 12 mm Hg and ScvO2 greater than or equal to 70% are recommended. While pulmonary artery catheters are not commonly recommended in patients who have sepsis, if one is used, the pulmonary artery occlusion pressure (PAOP) should be 12 to 15 mm Hg. Urine output should be greater than or equal to 0.5 mL/kg/hour (Forrester, 2023; Schmidt et al., 2024).
Dynamic measures of fluid response (respiratory changes in the vena cava diameter, radial artery pulse pressure, aortic blood flow peak velocity, left ventricular outflow tract velocity-time integral, carotid or brachial artery blood flow velocity) may be more accurate, although the effect on patient outcomes has not been proven clinically. For accuracy, patients should be in sinus rhythm with sufficient tidal volume during passive ventilation. An increase in CO in response to the passive leg-raising (PLR) maneuver can accurately predict fluid responsiveness in patients who have an irregular rhythm or those actively breathing. The maneuver should begin with the patient in the recumbent position. The patient’s trunk is lowered simultaneously as their bilateral lower extremities are raised (as shown in Figure 1). Then, CO (not just blood pressure) should be assessed directly for 1 minute by echocardiography, esophageal Doppler, arterial pulse contour analysis, or contour analysis of the volume clamp-derived arterial pressure after performing the maneuver. Patients who respond to fluid therapy based on hemodynamic or laboratory measures should undergo fluid therapy de-escalation and weaning of vasopressor support to avoid volume overload and pulmonary edema. This process may also require the careful administration of diuretics (Evans et al., 2021; Forrester, 2023; Schmidt et al., 2024).
Figure 1
Passive Leg Raise Maneuver
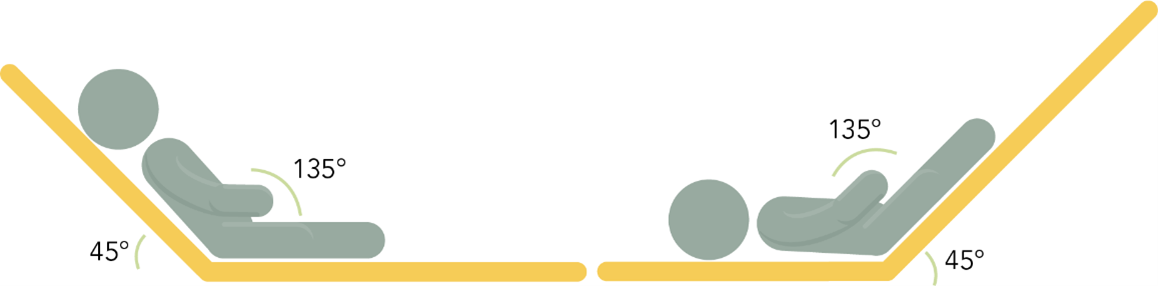
Serum lactate levels may be followed every 6 to 8 hours until the value has fallen to normal levels (0.5 to 1 mmol/L, termed lactate clearance) with a target of 10% to 20% clearance each time. Studies are unclear on the benefits of this approach because lactate can be a poor marker of tissue perfusion. Also, epinephrine (Adrenalin) can increase aerobic lactate production and make the use of lactate clearance-guided resuscitation impossible. Current recommendations consider lactate unhelpful in determining the restoration of perfusion with the following exception: a rising serum lactate level should prompt a reevaluation of the adequacy of perfusion, as elevated lactate levels can indicate poor perfusion and increased mortality (Forrester, 2023; Schmidt et al., 2024).
Arterial blood gases should be followed to determine gas exchange and the presence of acidosis, pulmonary edema, and complications (pneumothorax, ARDS, VTE). Routine laboratory values should be evaluated with particular attention paid to the platelet count, serum chemistries, and liver function tests. These may be performed every 6 hours until the values reach baseline. If hyperchloremia occurs, the IV solution should be switched to a low-chloride or buffered solution. Repeat CBC and additional cultures are typically useful in monitoring indices of infection (Forrester, 2023; Schmidt et al., 2024).
Sepsis Bundles
The SSC has developed bundles that are interventions and treatments that promote improved outcomes when implemented together. In 2008, the SSC created the severe sepsis 3-hour resuscitation bundle and the 6-hour septic shock bundle. These interventions are to be completed in 3 or 6 hours, depending on the bundle chosen. In 2018, these bundles were combined into a single hour-1 bundle (Gyawali et al., 2019). The hour-1 bundle is designed to encourage the health care team to obtain blood cultures, administer empiric antimicrobials, start fluid resuscitation, measure lactate levels, and initiate vasopressor therapy quickly if clinically indicated. The hour-1 bundle’s goal is to have interventions begin in the first hour after a patient’s sepsis diagnosis; they are not expected to be completed during the first hour. The hour-1 bundle includes the following interventions.
- Measure lactate level or remeasure if the initial lactate was elevated.
- Obtain blood cultures before initiating antimicrobials.
- Administer broad-spectrum antimicrobials.
- Initiate the rapid administration of 30 mL/kg crystalloid IV fluids for hypotension or lactate levels greater than 4 mmol/L.
- Begin vasopressor therapy in patients who are hypotensive during or after fluid resuscitation to maintain MAP greater than 65 mm Hg (SCCM, 2019).
The hour-1 bundle requires nurses and clinicians to act quickly when sepsis or septic shock is recognized in a patient. The time to treatment should be minimized because sepsis and septic shock are medical emergencies. The patient should be monitored for a clinical response to the interventions, and their sepsis status should be communicated in hand-offs (SCCM, 2019).
Goals of Care
The goals of care and the prognosis should be discussed with the patient and their family. Patients who have sepsis and multiorgan system failure have a high mortality rate, and some who survive may have a poor quality of life (QOL). The treatment goals for a patient in the ICU who has sepsis should be realistic, even though the outcome for these patients may be difficult to predict. End-of-life planning is essential, and palliative care should be discussed early and implemented when appropriate, especially if the patient was experiencing declining health before the diagnosis of sepsis. The goals of care should be established and discussed with the patient and their family as early as possible but no later than 72 hours after ICU admission. Even though patients can experience decreased QOL, patients who survive sepsis long-term often report being satisfied with their QOL and state they would undergo ICU treatment again. In this context, patient-specific conversations and goals of care are needed. While a formal palliative care consultation is not routinely suggested in all patients who have sepsis or septic shock, principles of palliative medicine should be integrated into the plan of care and may include a formal consultation if prudent (Evans et al., 2021; Prescott & Angus, 2018).
Special Populations
Sepsis is the fourth leading cause of maternal death in the US. The best way to manage sepsis in pregnancy is unknown, but most experts recommend the same guidelines outlined above. The regular physiological changes that occur during pregnancy complicate the evaluation and management of sepsis. The health care team should be aware of the altered hemodynamics of pregnancy when evaluating patient data and establishing goals. Physiologic anemia of pregnancy results from an increase in plasma volume without a proportional increase in red blood cell count, impairing the oxygen supply to tissues. Pregnant patients have an increased risk of aspiration due to delayed gastric emptying and elevation of the diaphragm, complicating intubation. The elevated diaphragm causes decreased residual volume, decreased oxygenation, and a faster rate of desaturation. Pregnancy can also increase WBC count. Preeclampsia can further increase a person’s WBC count, which complicates the diagnosis of infection. The increased heart rate and CO during pregnancy can elevate the risk of hypoperfusion and may mask the manifestations of sepsis. Increased clotting factors and von Willebrand factor elevate a pregnant patient’s risk of DIC and VTE. Ureteral dilation increases the risk of pyelonephritis, but the increased renal plasma flow and glomerular filtration rate during pregnancy may mask renal injury in sepsis (Bridwell et al., 2019; Schmidt et al., 2024).
Pregnancy is usually an exclusion criterion for clinical trials and studies of sepsis. Pregnancy was an exclusion criterion in the studies that established SOFA and qSOFA, so no studies have validated the use of these scoring systems in pregnant populations. The scoring systems used in pregnant patients who have sepsis are the Modified Early Obstetric Warning Score (MEOWS) and the Sepsis in Obstetrics Score (SOS). The MEOWS scale includes the same parameters as the original 2006 MEWS with adjusted scoring in each category, and the noted use of oxygen saturation in lieu of urine output. Out of a total score of 0-18, a MEOWS score of 6 and above indicates high risk, 4 or 5 is moderate risk, and a score of 3 or below is low risk. The SOS score incorporates many of the same clinical details as the MEOWS (HR, RR, SBP, temperature, and SaO2). However, instead of mental status/level of consciousness, the SOS incorporates the patient's laboratory results (WBC count, percentage of bands, and lactic acid [lactate] level). The SOS score ranges from 0-27, with a score of 6 or above indicating high risk (Bridwell et al., 2019).
Sepsis is also a leading cause of morbidity, mortality, and health care resource consumption for children worldwide. Across the globe, approximately 1.2 million cases of childhood sepsis happen each year. Mortality for pediatric patients who have sepsis ranges from 4% to 50% and depends on the severity of illness, risk factors, and geographic location. Most pediatric patients who die from sepsis experience shock or MODS. Many of these deaths occur during the initial 48 to 72 hours of treatment. The International Pediatric Sepsis Consensus Conference published a definition for sepsis, severe sepsis, and septic shock in children in 2005. This definition and criteria were based on findings in adult sepsis at the time, with modifications for physiology based on the age and maturation of the patient. There have been attempts to change the pediatric definition to match that of 2016's Sepsis-3 for adults. However, no official update has occurred; therefore, the 2005 definition still applies to pediatric sepsis (Weiss et al., 2020). The definition of severe sepsis consists of the following:
- two or more SIRS criteria
- confirmed or suspected infection
- cardiovascular dysfunction, ARDS, or two or more non-cardiovascular organ system dysfunctions (Weiss et al., 2020)
The 2005 conference defined septic shock in children as severe sepsis (above) with cardiovascular dysfunction as evidenced by hypotension, treatment with vasopressors, or impaired perfusion (Weiss et al., 2020).
The SSC updated the International Guidelines for the Management of Septic Shock and Sepsis-Associated Organ Dysfunction in Children in 2020. These pediatric guidelines apply to all patients from greater than or equal to 37 weeks of gestation at birth to 18 years of age who have sepsis or septic shock. They define septic shock as severe infection leading to cardiovascular dysfunction as evidenced by hypotension, treatment with vasopressors, or impaired perfusion. Sepsis-associated organ dysfunction in children is defined as severe infection leading to cardiovascular or noncardiovascular organ dysfunction (Weiss et al., 2020). The guidelines for treating septic shock and sepsis-associated organ dysfunction in children are similar to the recommendations for adults. The SSC has published the Initial Resuscitation Algorithm for Children, which provides systemic screening for sepsis in pediatric patients and care guidance for settings with and without ICU services. The algorithm has been endorsed by many professional organizations, including the American Academy of Pediatrics (Weiss et al., 2020).
The 2020 SSC guidelines for children suggest that protocols and guidelines for the management of children who have sepsis be implemented (Weiss et al., 2020). Specifics largely mirror the adult guidelines, such as obtaining blood cultures prior to antimicrobial administration, empiric broad-spectrum antimicrobial therapy within the first hour for those who have septic shock (3 hours for those who have sepsis without shock) using dosing strategies based on pharmacokinetics/pharmacodynamic principles, and daily assessments to facilitate narrowing antimicrobials once culture and sensitivity data are available. Fluid bolusing up to 40 to 60 mL/kg (10 to 20 mL/kg per bolus) of balanced/buffered crystalloids is recommended over the first hour in facilities with ICU-level resources. If ICU resources are unavailable, maintenance fluids should be given to those children who do not have hypotension, and up to 40 mL/kg (10 to 20 mL/kg per bolus) are recommended over the first hour for children who have hypotension. The SSC guidelines suggest the use of advanced hemodynamic monitoring (CO, cardiac index, systemic vascular resistance, ScvO2) in addition to bedside clinical variables and lactate level trends to guide resuscitation in children who have sepsis. They were unable to recommend a first-line vasopressor in children but recommended the use of epinephrine (Adrenalin) or norepinephrine (Levophed) over dopamine (Intropin) and suggested adding vasopressin (Vasostrict) if high doses of catecholamines are required to maintain or optimize perfusion. They were unable to make a recommendation regarding the use of an indicator in children. NIV should be trialed prior to intubation. Etomidate (Amidate) should be avoided, but a neuromuscular blocking agent should be administered during intubation. Inhaled nitric oxide (iNO) is not routinely recommended unless as a rescue therapy, and prone positioning should be trialed in children. They were unable to make a recommendation regarding the use of recruitment maneuvers in children. A blood glucose target range recommendation was not able to be reached, but insulin therapy should not be used to maintain a blood glucose level below 140 mg/dL. Early enteral feeding is recommended, but prokinetic agents for feeding intolerance and prophylaxis for stress ulcers are not recommended. Similarly, routine pharmacological prophylaxis for VTE is not recommended in children (Weiss et al., 2020).
Health Promotion and Prevention
The best management for sepsis and septic shock is prevention. It is crucial to evaluate all patients’ risks for sepsis. This is especially important for older patients, as the death rate in patients over 65 years old is nearly double the rate of younger adults. Using medical and surgical asepsis as appropriate during invasive procedures is paramount. Patients should have IV access lines and indwelling urinary catheters removed as soon as they are no longer required, and patients on ventilators should be weaned as soon as possible. Sepsis complicates many conditions that bring patients to acute care settings, so it should always be considered a possibility. Protocols in the ED can identify patients who have early sepsis on admission and improve the timing for treatment initiation. Patients discharged home after invasive procedures should be taught manifestations of local infection and early sepsis. Using a thermometer, they should take their temperature twice a day or when feeling unwell. Patients should also be taught to take antibiotics as prescribed for the entire course (Ignatavicius et al., 2023).
Surveillance methods are recommended for administrative, program, and clinical practices for quality-improvement projects. A pre-assessment of a facility’s sepsis practices helps interpret the surveillance results and provides a basis to create recommendations for improving patient care (CDC, 2018). Administrative and program procedures to review include the following.
- sepsis education and awareness campaigns
- sepsis compliance efforts
- ED, hospital ward, or ICU sepsis teams
- presence of sepsis code teams
- antibiotic stewardship and systematic antibiotic practices
- use of electronic health record prediction tools, alerts, order sets, and protocols related to sepsis
- sepsis billing and coding practices (CDC, 2018)
Clinical practices to review include the following.
- ED sepsis diagnosis and triage practices
- hospital ward or ICU screening practices
- presence of and compliance with sepsis protocols and bundles
- clinical trial or quality improvement initiatives
- referral or transfer of patients who have sepsis to other hospitals (CDC, 2018)
Hand hygiene is one of the most effective infection-prevention measures. The WHO emphasizes hand hygiene during five periods.
- before contact with a patient
- before a procedure is performed
- after the risk of exposure to biological fluids
- after contact with a patient
- after contact with areas near a patient (Procianoy & Silveira, 2020)
Complications
Of the patients who survive sepsis and are discharged from the hospital, half recover fully, a third will die in the following year, and one-sixth of the patients will have severe persistent impairments. These patients will develop an average of one to two new functional limitations, such as the inability to perform activities of daily living like bathing or dressing independently. They also have triple the prevalence of moderate to severe cognitive impairment and a high rate of mental health disorders, including anxiety, depression, and posttraumatic stress disorder. Around 40% of the patients will be readmitted to the hospital within 90 days of being discharged. Patients who survive sepsis have an increased risk of recurrent infections, acute renal failure, and new cardiovascular events. There are many reasons for the deterioration of health after sepsis, such as a rapid progression of preexisting, chronic health conditions, residual organ damage, and impaired immune function. Patients who had poor health before developing sepsis and those who experienced septic shock have higher rates of complications after hospital discharge (Prescott & Angus, 2018).
Patients commonly contract hospital-acquired infections while being treated for sepsis. A nosocomial infection usually develops in the late phase of sepsis, particularly in the lungs. The development of this nosocomial infection is not related to the primary site of infection from which sepsis developed. Instead, the main contributing factor is likely sepsis-related immunosuppression from depressed cytokine responses and lymphocyte apoptosis. Reactivation of dormant viral infections has also been documented. Risk factors for the development of nosocomial infections include increased age, high illness severity scores, an extended ICU stay, and respiratory insufficiency. Central lines and endotracheal intubation also increase the risk of nosocomial infections after sepsis (Denstaedt et al., 2018).
Encephalopathy and a depressed LOC are other frequent complications of sepsis. Patients may acquire neurological damage related to sepsis in various ways, including cerebral ischemia, metabolic changes, and brain inflammation, leading to long-term impairments in memory, attention span, and verbal fluency. Thus, their ability to return to work or school may be limited. Many patients who survive sepsis enter a state of chronic critical illness driven by persistent inflammation, immunosuppression, and catabolism syndrome. The pathophysiology of these conditions is not entirely understood. After experiencing sepsis, other manifestations reported by patients include pain, numbness, visual disturbances, hair loss, dental problems, and problems with their fingernails. Amputation due to gangrene in a limb is an extreme complication of sepsis that results from cardiovascular shock, circulatory dysfunction, or high dosages of vasopressors. Nerve conduction can become impaired due to a loss of axonal fibers during sepsis, leading to critical illness neuropathy. A similar mechanism can also induce sepsis-related myopathy. In this context, paired neuropathy and myopathy are called ICU-acquired weakness and can worsen patient outcomes. ICU-acquired weakness may not improve for up to a year after discharge or become permanent (Cavaillon et al., 2020; Loftus, 2017; Prescott & Angus, 2018; Schmidt et al., 2024).
Patients who survive sepsis have reported a lower QOL in comparison with the average population. These patients often cannot resume their prior roles and activities. If they were employed before developing sepsis, only 43% return to work within a year. Only 33% of patients who lived independently before developing sepsis can return to living independently within 6 months of discharge. For the family members of patients who survive sepsis, their role often shifts to that of a caregiver. One study of those caring for a partner or family member after surviving sepsis found that rates of depression in the caregivers increased by 14% (Prescott & Angus, 2018).
Implications for Advanced Practice Nursing
The APRN’s role in managing sepsis is not well defined in existing guidelines. Nurses have reported deficits in their ability to recognize and respond to patients who have suspected sepsis. The development and implementation of nurse-inclusive sepsis guidelines have been suggested to address the deficits identified in the nurse’s role in sepsis care (Harley et al., 2019). In multiple studies, nurses were authorized to initiate order sets for lactate levels and blood cultures or begin fluid boluses when sepsis was suspected. Nurse-directed care that promotes sepsis’s early identification and treatment reduces the in-hospital sepsis mortality rate (Ferguson et al., 2019; Harley et al., 2019; Moore et al., 2019).
Most of the research on sepsis focuses on patients in ED and ICU settings; however, many patients develop sepsis while on general medical-surgical units in hospitals. Health care providers in all hospital settings must be familiar with the early warning signs of sepsis to improve survival rates. Screening and early recognition of sepsis in at-risk patients can prevent further progression of the sepsis cycle. APRNs should know their facility’s screening tools and protocols for treatment to facilitate early recognition and rapid initiation of treatment. In addition to improved survival, earlier treatment may also result in fewer long-term complications. Furthermore, infection prevention can be accomplished by encouraging patients to manage their chronic conditions. APRNs should always follow hand hygiene recommendations and medical and surgical asepsis protocols as recommended (CDC, 2023; Creed & Spiers, 2020; Prescott & Angus, 2018).
To prevent complications in patients who survive sepsis, APRNs should identify any new physical, cognitive, and mental problems and refer these patients for appropriate treatment. Long-term medications should be reviewed and adjusted based on organ functioning and the patient’s condition. Changes in renal function, weight, and fluid balance often occur with sepsis, potentially altering the dosage and suitability of previous medications. Patients should be evaluated for treatable conditions to prevent secondary infections or rehospitalization, such as aspiration, heart failure, or renal failure. If a patient had poor health before sepsis and experienced deterioration of their condition, hospice care might be an option to consider with the family (Prescott & Angus, 2018).
Because of the multiple complications and changes a patient may experience after sepsis, early referrals to subspecialists and ancillary services may be needed. Various factors affect each patient’s ability to follow up and carry out treatment plans, such as weakness, cognitive impairment, loss of income, and caregiver availability. These should all be considered when developing discharge plans. Referrals to address the most significant problems may be prioritized, and then additional referrals can be made. Patients and their caregivers should be educated about sepsis and any possible complications they may experience, and they should be offered peer support resources. The SCCM recently developed in-person, online, and telephone-based support groups for patients who survive critical illness and their families. ICU diaries are non-medical accounts of the patient’s hospitalization. They are written by staff and family members and have been shown to reduce post-traumatic stress disorder manifestations when given to patients and caregivers a month after the patient’s ICU stay (Prescott & Angus, 2018).
To prevent reinfection and readmission, APRNs should counsel patients about their risk of infection and recurrent sepsis and evidence-based suggestions on how to reduce this risk if available. Patients should be encouraged to receive all appropriate vaccinations. The APRN should review the early manifestations of infection and encourage the patient to seek medical care for suspected infection. Patients should recognize the early indications that infection has progressed to sepsis, including decreased urine output, changes in the LOC, cyanosis, and mottling skin. APRNs may need to schedule telephone or in-person follow-up appointments to monitor patient improvement after discharge. Because many patients experience a worsening of chronic conditions after an episode of sepsis, APRNs should perform a medication review of and reassess each patient’s doses and need for medications (diuretics, beta-blockers, angiotensin-converting enzyme inhibitors). Finally, APRNs should reinforce the importance of regular laboratory testing, such as chemistry panels, to monitor renal and hepatic function (Prescott & Angus, 2018).
References
Berg, D. & Gerlach, H. (2018). Recent advances in understanding and managing sepsis. F1000Research, 7(F1000 Faculty Reviews), 1570. https://doi.org/10.12688/f1000research.15758.1
Bokhari, A. M. (2023a). Bacterial sepsis clinical presentation. https://emedicine.medscape.com/article/234587-clinical#b4
Bokhari, A. M. (2023b). Bacterial sepsis overview. https://emedicine.medscape.com/article/234587-overview#a8
Bridwell, R. E., Carius, B. M., Long, B., Oliver, J. J., & Schmitz, G. (2019). Sepsis in pregnancy: Recognition and resuscitation. The Western Journal of Emergency Medicine, 20(5), 822–832. https://doi.org/10.5811/westjem.2019.6.43369
Bullock, B. & Benham, M. D. (2023). Bacterial sepsis. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK537054
Cavaillon, J., Singer, M., & Skirecki, T. (2020). Sepsis therapies: Learning from 30 years of failure of translational research to propose new leads. EMBO Molecular Medicine, 12, e10128. https://doi.org/10.15252/emmm.201810128
Centers for Disease Control and Prevention. (2018). Hospital toolkit for adult sepsis surveillance. https://www.cdc.gov/sepsis/pdfs/Sepsis-Surveillance-Toolkit-Aug-2018_508.pdf
Centers for Disease Control and Prevention. (2023). Sepsis: What is sepsis? https://www.cdc.gov/sepsis/what-is-sepsis.html
Creed, F. & Spiers, C. (2020). Care of the acutely ill adult: A essential guide for nurses (2nd ed.). Oxford University Press.
Denstaedt, S., Singer, B., & Standiford, T. (2018). Sepsis and nosocomial infection: Patient characteristics, mechanisms, and modulation. Frontiers in Immunology, 9. https://doi.org/10.3389/fimmu.2018.02446
Doyle, D. J. (2018). Clinical early warning scores: New clinical tools in evolution. The Open Anesthesia Journal, 12, 26–33. http://dx.doi.org/10.2174/2589645801812010026
Dugar, S., Choudhary, C., & Duggal, A. (2020). Sepsis and septic shock: Guideline-based management. Cleveland Clinic Journal of Medicine, 87(1), 53–64. https://doi.org/10.3949/ccjm.87a.18143
Evans, L., Rhodes, A., Alhazzani, W., Antonelli, M., Coopersmith, C. M., French, C., Machado, F. R., Mcintyre, L., Ostermann, M., Prescott, H. C., Schorr, C., Simpson, S., Wiersinga, W. J., Alshamsi, F., Angus, D. C., Arabi, Y., Azevedo, L., Beale, R., Beilman, G., . . . Levy, M. (2021). Surviving sepsis campaign: International guidelines for management of sepsis and septic shock 2021. Critical Care Medicine, 49(11), e1063–e1143. https://doi.org/10.1097/CCM.0000000000005337
Fay, K., Sapiano, M., Gokhale, R., Dantes, R., Thompson, N., Katz, D., Ray, S., Wilson, L., Perlmutter, R., Nadle, J., Godine, D., Frank, L., Brousseau, G., Johnston, H., Bamberg, W., Dumyati, G., Nelson, D., Lynfield, R., DeSilva, M., . . . Epstein, L. (2020). Assessment of health care exposures and outcomes in adult patients with sepsis and septic shock. Journal of the American Medical Association Network Open, 3(7). https://doi.org/10.1001/jamanetworkopen.2020.6004
Ferguson, A., Coates, D., Osborn, S., Blackmore, C., & Williams, B. (2019). Early, nurse-directed sepsis care. American Journal of Nursing, 119(1), 52–58. https://doi.org/10.1097/01.NAJ.0000552614.89028.d6
File, T. M., Jr. (2022). Morbidity and mortality associated with community-acquired pneumonia in adults. UpToDate. Retrieved January 23, 2024, from https://www.uptodate.com/contents/morbidity-and-mortality-associated-with-community-acquired-pneumonia-in-adults
Forrester, J. D. (2023). Sepsis and septic shock. https://www.merckmanuals.com/professional/critical-care-medicine/sepsis-and-septic-shock/sepsis-and-septic-shock
Gardner-Thorpe, J., Love, N., Wrightson, J., Walsh, S., & Keeling, N. (2006). The value of Modified Early Warning Score (MEWS) in surgical in-patients: A prospective observational study. Annals of the Royal College of Surgeons of England, 88(6), 571–575. https://doi.org/10.1308/003588406X130615
Gauer, R., Forbes, D., & Boyer, N. (2020). Sepsis: Diagnosis and management. American Family Physician, 101(7), 409–418. https://www.aafp.org/afp/2020/0401/p409.html
Gyawali, B., Ramakrishna, K., & Dhamoon, A. S. (2019). Sepsis: The evolution in definition, pathophysiology, and management. SAGE Open Medicine, 7. https://doi.org/10.1177/2050312119835043
Harley, A., Johnston, A., Denny, K., Keijzers, G., Crilly, J., & Massey, D. (2019). Emergency nurses’ knowledge and understanding of their role in recognizing and responding to patients with sepsis: A qualitative study. International Emergency Nursing, 43, 106–112. https://doi.org/10.1016/j.ienj.2019.01.005
Hinkle, J. L., Cheever, K. H., & Overbaugh, K. (2021). Brunner & Suddarth’s textbook of medical-surgical nursing (15th ed.). Wolters Kluwer.
Hollenbeak, C. S., Henning, D. J., Geeting, G. K., Ledeboer, N. A., Faruqi, I. A., Pierce, C., Thomas, C. B., & O’Neal, H. R., Jr. (2023). Cost and consequences of a novel emergency department sepsis diagnostic test: The IntelliSep Index. Critical Care Explorations, 5(7), e0942. https://doi.org/10.1097%2FCCE.0000000000000942
Howell, M. D., Talmor, D., Schuetz, P., Hunziker, S., Jones, A. E., & Shapiro, N. I. (2011). Proof of principle: the predisposition, infection, response, organ failure sepsis staging system. Critical Care Medicine, 39(2), 322–327. https://doi.org/10.1097/CCM.0b013e3182037a8e
Ignatavicius, D., Rebar, C. R., & Heimgartner, N. M. (2023). Medical-surgical nursing: Patient-centered collaborative care (11th ed.). Elsevier.
Lambden, S., Laterre, P., Levy, M., & Francois, B. (2019). The SOFA score—development, utility, and challenges of accurate assessment in clinical trials. Critical Care, 23(374). https://doi.org/10.1186/s13054-019-2663-7
Lehman, B. & Dandache, P. (2020). Disease management: Sepsis. Cleveland Clinic Center for Continuing Education. http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/infectious-disease/sepsis
Loftus, T., Mira, J., Ozrazgat-Baslanti, T., Ghita, G., Wang, Z., Stortz, J., Brumback, B., Bihorac, A., Segal, M., Anton, S., Leeuwenburgh, C., Mohr, A., Efron, P., Moldawer, L., Moore, F., & Brakenridge, S. (2017). Sepsis and critical illness research center investigators: Protocols and standard operating procedures for a prospective cohort study of sepsis in critically ill surgical patients. BMJ Open, 7(7). https://doi.org/10.1136/bmjopen-2016-015136
Marik, P. E. & Taeb, A. M. (2017). SIRS, qSOFA and new sepsis definition. Journal of Thoracic Disease, 9(4), 943–945. https://doi.org/10.21037/jtd.2017.03.125
Markwart, R., Saito, H., Harder, T., Tomczyk, S., Cassini, A., Fleischmann-Struzek, C., Reichert, F., Eckmanns, T., & Allegranzi, B. (2020). Epidemiology and burden of sepsis acquired in hospitals and intensive care units: A systemic review and meta-analysis. Intensive Care Medicine, 46(8), 1536–1551. https://doi.org/10.1007/s00134-020-06106-2
Moore, W., Vermuelen, A., Taylor, R., Kihara, D., & Wahome, E. (2019). Improving 3-hour sepsis bundled care outcomes: Implementation of a nurse-driven sepsis protocol in the emergency department. Journal of Emergency Nursing, 45(6), 690–698. https://doi.org/10.1016/j.jen.2019.05.005
Moreno, R. P., Metnitz, B., Adler, L., Hoechtl, A., Bauer, P., Metnitz, P. G., & SAPS 3 Investigators (2008). Sepsis mortality prediction based on predisposition, infection and response. Intensive Care Medicine, 34(3), 496–504. https://doi.org/10.1007/s00134-007-0943-1
Neviere, R. (2023). Sepsis syndromes in adults: Epidemiology, definitions, clinical presentation, diagnosis, and prognosis. UpToDate. Retrieved January 18, 2024, from https://www.uptodate.com/contents/sepsis-syndromes-in-adults-epidemiology-definitions-clinical-presentation-diagnosis-and-prognosis
Plaeke, P., DeMan, J., Coenen, S., Jorens, P., DeWinter, B., & Hubens, G. (2020). Clinical- and surgery-specific risk factors for postoperative sepsis: A systematic review and meta-analysis of over 30 million patients. Surgery Today, 50, 427–439. https://doi.org/10.1007/s00595-019-01827-4
Prescott, H. & Angus, D. (2018). Enhancing recovery from sepsis: A review. Journal of the American Medical Association, 319(1), 62–75. https://doi.org/10.1001/jama.2017.17687
Procianoy, R. & Silveira, R. (2020). The challenges of neonatal sepsis management: The challenges in managing neonatal sepsis. Journal of Pediatrics, 96(1), 80–86. https://doi.org/10.1016/j.jped.2019.10.004
Rathour, S., Kumar, S., Hadda, V., Bhalla, A., Sharma, N., & Varma, S. (2015). PIRO concept: Staging of sepsis. Journal of Postgraduate Medicine, 61(4), 235–242. https://doi.org/10.4103/0022-3859.166511
Renew, J., Ratzlaff, R., Hernandez-Torres, V., Brull, S., & Prielipp, R. (2020). Neuromuscular blockade management in the critically ill patient. Journal of Intensive Care, 8(37). https://doi.org/10.1186/s40560-020-00455-2
Rubulotta, F., Marshall, J. C., Ramsay, G., Nelson, D., Levy, M., & Williams, M. (2009). Predisposition, insult/infection, response, and organ dysfunction: A new model for staging severe sepsis. Critical Care Medicine, 37(4), 1329–1335. https://doi.org/10.1097/CCM.0b013e31819d5db1
Schmidt, G., Mandel, J., & Bell, T. D. (2024). Evaluation and management of suspected sepsis and septic shock in adults. UpToDate. Retrieved January 29, 2024, from https://www.uptodate.com/contents/evaluation-and-management-of-suspected-sepsis-and-septic-shock-in-adults
Schünemann, H. J., Cushman, M., Burnett, A. E., Kahn, S. R., Beyer-Westendorf, J., Spencer, F. A., Rezende, S. M., Zakai, N. A., Bauer, K. A., Dentali, F., Lansing, J., Balduzzi, S., Darzi, A., Morgano, G. A., Neumann, I., Nieuwlaat, R., Yepes-Nuñez, J. J., Zhang, Y., & Wiercioch, W. (2018). American Society of Hematology 2018 guidelines for management of venous thromboembolism: Prophylaxis for hospitalized and nonhospitalized medical patients. Blood Advances, 2(22), 3198–3225. https://doi.org/10.1182/bloodadvances.2018022954
Seres, D. (2024). Nutrition support in intubated critically ill adult patients: Enteral nutrition. UpToDate. Retrieved March 4, 2024, from https://www.uptodate.com/contents/nutrition-support-in-intubated-critically-ill-adult-patients-enteral-nutrition
Shankar-Hari, M., Saha, R., Wilson, J., Prescott, H., Harrison, D., Rowan, K., Rubenfeld, G., & Adhikari, N. (2020). Rate and risk factors for rehospitalization in sepsis survivors: Systematic review and meta-analysis. Intensive Care Medicine, 46, 619–636. https://doi.org/10.1007/s00134-019-05908-3
Shi, R., Hamzaoui, O., De Vita, N., Monnet, X., & Teboul, J. (2020). Vasopressors in septic shock: Which, when, and how much? Annals of Translational Medicine. 8(12), 794. https://doi.org/10.21037/atm.2020.04.24
Singer, M., Deutschman, C. S., Seymour, C. W., Shankar-Hari, M., Annane, D., Bauer, M., Bellomo, R., Bernard, G. R., Chiche, J. D., Coopersmith, C. M., Hotchkiss, R. S., Levy, M. M., Marshall, J. C., Martin, G. S., Opal, S. M., Rubenfeld, G. D., van der Poll, T., Vincent, J. L., & Angus, D. C. (2016). The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA, 315(8), 801–810. https://doi.org/10.1001/jama.2016.0287
Society of Critical Care Medicine. (2019). Hour-1 bundle: Initial resuscitation for sepsis and septic shock. Surviving Sepsis Campaign. https://www.sccm.org/sccm/media/PDFs/Surviving-Sepsis-Campaign-Hour-1-Bundle.pdf
Society of Critical Care Medicine. (2021). Surviving sepsis campaign 2021 adult guidelines. Surviving Sepsis Campaign. https://www.sccm.org/SurvivingSepsisCampaign/Guidelines/Adult-Patients
Songsangjinda, T. & Khwannimit, B. (2020). Comparison of severity score models based on different sepsis definitions to predict in-hospital mortality among sepsis patients in the Intensive Care Unit. Medicina Intensiva, 44(4), 226–232. https://doi.org/10.1016/j.medine.2018.12.007
Tandukar, S. & Palevsky, P. M. (2019). Continuous renal replacement therapy: Who, when, why, and how. Chest, 155(3), 626–638. https://doi.org/10.1016/j.chest.2018.09.004
Thavamani, A., Umapathi, K., Dhanpalreddy, H., Khatana, J., Chotikanatis, K., Allareddy, V., & Roy, A. (2020). Epidemiology, clinical and microbiologic profile and risk factors for inpatient mortality in pediatric severe sepsis in the United States from 2003 to 2014: A large population analysis. The Pediatric Infectious Disease Journal, 39(9), 781–788. https://doi.org/10.1097/INF.0000000000002669
Vafaei, A., Heydari, K., Hashemi-Nazari, S., Izadi, N., & Zadeh, H. (2019). PIRO, SOFA, and MEDS scores in predicting one-month mortality of sepsis patients: A diagnostic accuracy study. Archives of Academic Emergency Medicine. 7(1), e59. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6905425
Vincent, J., Moreno, R., Takala, J., Willatts, S., De Mendonça, A., Bruining, H., Reinhart, C., Suter, P., & Thijs, L. (1996). The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. Intensive Care Medicine, 22(7), 707–710. https://doi.org/10.1007/BF01709751
Weiss, S., Peters, M., Alhazzani, W., Agus, M., Flori, H., Inwald, D., Nadel, S., Schlapbach, L., Tasker, R., Argent, A., Brierley, J., Carcillo, J., Carrol, E., Carroll, C., Cheifetz, I., Choong, K., Cies, J., Cruz, A., De Luca, D., . . . Tissieres, P. (2020). Surviving sepsis campaign international guidelines for the management of septic shock and sepsis-associated organ dysfunction in children. Pediatric Critical Care Medicine, 21(2), 52–106. https://doi.org/10.1097/PCC.0000000000002198
World Health Organization (2023). Sepsis. https://www.who.int/news-room/fact-sheets/detail/sepsis